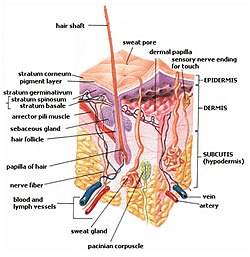
Equine Integumentary System - Horse Anatomy
| This article is still under construction. |
Skin
Epidermis
The epidermis is a stratified squamous epithelium and is composed of 4 cell layers anchored to a basal lamina of connective tissue. Keratinocytes migrate through the epidermis from the basal layer. This migration begins in the stratum basale, then moves up through the stratum spinosum, stratum granulosum and the stratum corneum.
Stratum basale
The deepest layer of the epidermis is the stratum basale. It consists of a single layer of columnar epithelium which is adhered to the basal lamina. Nutrition is supplied from the underlying capillaries of the dermis. Migration of cells towards the surface begins here.
Stratum spinosum
Above the stratum basale is the stratum spinosum. Spinous cells are large polygonal cells with prominent desmosomal intercellular filaments, which act like bridges between the cells. When cells move into this layer, they shrink and move apart. Keratinisation begins in the stratum spinosum and continues in the stratum granulosum.
Stratum Granulosum
External to the stratum spinosum, lies the stratum granulosum. Granular cells are thin, flattened keratinocytes with variably prominent keratohyaline granules. At its outer surface, the stratum granulosum secretes oragnelles called lamellar bodies, which are composed of lipid and enzymes which fuse with the plasma membrane and help to form the water concentration gradient that leads to transepidermal water loss.
Stratum Corneum
The outer layer, stratum corneum, consists of anucleate, thin cells filled with keratin filaments and proteins that form a cell envelope resistant to solvents and enzymes; there is also a permeability barrier to water and ions. The cells of the stratum corneum are embedded in a lipid-rich matrix which helps to hold the cells together, while the desmosomes that were present in lower layers have disappeared. For the stratum corneum to maintain a constant thickness, there is a constant turnover of exfoliated corneocytes, being replaced by new corneocytes. Enzymes in the lamellar bodies from the stratum granulosum help to break down the intercellular lipid 'glue' that holds the cells in place and there is also some degradation of desmosomes.
Cells of the Epidermis
- Langerhans' cells
These are dentritic cells derived from bone marrow. They act as antigen presenting cells in the epidermis as part of the mononuclear phagocyte immune system. Langerhans' cells express MHC I and II molecules and immunoglubulin Fc receptors and are a key feature of delayed hypersensitivity responses.
- Melanocytes
These are also dentritic cells and are derived from the neural crest. They are immersed in the epidermis where they form close contact with a defined number of keratinocytes - an epidermal-melanin unit. Melanin is composed of 2 types: eumelanin which is black-brown and phaeomelanin which is reddish-brown. Melanocytes produce pigment in melanosome structures which are membrane-bound structures involved in the transfer of pigment to keratinocytes. An important function of melanin is UV protection and absence of pigment confers increased sensitivity to UV damage.
- Merkel cells
These are part of the sensory apparatus of the skin and are located within the stratum basale of the epidermis where they act as slow-adapting mechanoreceptors. They are usually closely associated with the afferent myelinated nerve fibres, arranged in a plate-like structure with the base of the Merkel cell, together forming a Merkel's corpuscle.
Dermis
The epidermis interfaces with the underlying dermis at the basement membrane zone (BMZ). The binding includes anchoring junctions called hemidesmosomes and focal adhesions. The former comprise extra cellular matrix (ECM) proteins such as laminin-5 and collagen type IV molecules, which form the lamina densa part of the BMZ, while the lamina lucida is composed of Collagen type V. Collagen type VII is important in forming anchoring fibrils between the dermis and the basal lamina.
The dermis consists of dense fibrous tissue composed of collagen type I, III and V, with some elastin fibres and provides a supporting mattress for the carriage of blood vessels, lymphatic vessels, nerves and sensory receptors, hair follicles, sebaceous and sweat glands, with circulating white cells.
Cutaneous Appendages
Eyelids
The palpebral margin is thicker than the remainder of the eyelid and cilia grow from the margin. There are various glands in the region, including Moll's glands that are modified sweat glands, associated with the cilia. Meibomian glands, Zeis glands associated with the cilia and the lacrimal glands together produce the tear film.
Hair
All hair has a similar structure: an outer cuticle, a cortex containing pigmentation, an inner medulla and a root or bulb from which the hair grows out of the follicle to form the shaft.
Each hair follicle has a sebaceous gland and an arrector pili muscle associated with it.
Hair follicles are divided into three parts:
- The infundibulum corresponds to the area from the opening of the sebaceous duct to the surface of the skin.
- The isthmus is the area between the opening of the sebaceous duct and the attachment of the arrector pili muscle.
- The inferior segment extends from the attachment of the arrector pili muscle to the dermal hair papilla.
The hair follicle originates from a peg of epidermal cells that grows down into the underlying dermis, where it forms a hair cone over a piece of dermis called the dermal papilla. The papilla provides the blood and nerve supply for the growing hair. From the hair cone, the cells keratinise and form a hair. As the hair grows up through the epidermis to the skin's surface, the cells at the point of the cone die, forming a channel, the hair follicle.
Hair Types
Guard Hairs
These are generally stiff and straight and form the outer haircoat of an animal. They are uniformly distributed across the skin surface and give the haircoat a smooth appearance. The smoothness of the coat is important in allowing rain to fall from the surface without penetrating deeper to the epidermis and causing loss of body temperature. The oily coating of the haircoat comes from the secretions of the sebaceous glands in the epidermis, associated with the hair follicle. This also contributes to the ‘waterproofing’ of the haircoat. Each hair consists of an outer cuticle, with a cortex and innermost medulla. It is composed of highly keratinised, dead epithelial cells, with the arrangement into the 3 layers conferring flexibility. The arrector pili muscle is attached to the proximal end of the follicle and the dermis close to the point at which the hair is externalised. Involuntary contraction of this muscle in cold ambient temperatures causes erection of the hairs to trap warm air against the skin, thus providing insulation. This can also be induced by the ‘fight or flight’ mechanism of the sympathetic nervous system. Modifications of the guard hairs in horses include the coarse hair of the mane, tail and the tufts of hair ('feathers') around the fetlock region.
Wool Hairs
These are thin, wavy, soft hairs that form the undercoat of animals. They are often much more numerous than the tough guard hairs and usually shorter. Their number increases in winter when they serve to keep the body warm.
Tactile Hairs
Tactile hairs are associated with a sensory function and are much thicker and stiffer than other hairs. They are mainly found on the face and can also be referred to as whiskers or vibrissae. Their follicles are much deeper into the hypodermis than guard or wool hairs and possess a venous sinus and nerve endings with mechanoreceptors. During embryonic development, they appear before other hair types. These hairs are mostly found on the face, near the eyes and on the upper lip.
Tylotrich Hairs
These large hair follicles are rapidly adapting mechanoreceptors. They may be present anywhere on the body. These structures consist of a single large hair, surrounded by neurovascular tissue at the level of the sebaceous gland.
Skin Glands
Sweat Glands
Sweat is considered to be the product of apoptosis releasing cell contents into the gland lumen, together with secretion where exocytosis, microapocrine blebbing, transcellular and perhaps paracellular processes involved in varying degrees. Sweat is composed of secretions and cellular debris and includes inorganic ions, water, immunoglobulins, amino acids and waste products including urea and lactic acid. Equine sweat is rich in proteins including glycoproteins, albumin and gammaglobulins, which cause the sweat to froth and the horse is said to "lather up".
Sebaceous Glands
One or more sebaceous glands surround each hair follicle at a point about 1/3 of its length beneath the skin's surface. Each gland is composed of numerous acini attached to a common excretory duct through which they discharge their secretions (sebum) onto the hair shaft and epidermis. In the skin and eyelids such glands release the cell contents together with secretory products with holocrine secretion. This secretion involves apoptosis in which the secretory products and cell debris are released into the gland lumen. The secretory products vary from species to species and include various fatty acids, diglycerides, cholesterol, diesters, wax esters and giant-ring lactones. The function of sebum is that of an emolient of the hair and skin, preventing excessive dryness. It may combine with sweat to form an emulsion within the stratum corneum and a form of cement around the hair pores preventing bacterial invasion of the epidermis. Sebum is also released from the glands during piloerection, as the action of the arrector pili muscle squeezes the gland as it raises the hair.
Specialised Glands
Specialised glands in the horse exist in the frog.
Mammary Glands
The mamma (pleural = mammae) is the glandular structure associated with a papilla (teat) and may contains two ducts in the mare. The udder is a term designating all the mammae in the mare. The mammary glands of the mare are close together, forming a small udder in the inguinal region. There is an intermammary groove separating the left and right halves. Each half comprises a single mammary complex, which each has two mammary units. The lobes are the internal compartments of the mamma, separated by adipose tissue. The lobes are divided into lobules, consisting of connective tissue containing alveoli, which are clusters of milk secreting cells. The lactiferous ducts are large ducts conveying milk from the alveoli to the lactiferous sinus. The openings of the lactiferous ducts convey milk formed in the alveolus to the gland sinus.
The lactiferous sinus (milk sinus) is the milk storage cavity within the teat and glandular body. The gland sinus is part of the milk sinus within the glandular body and the teat sinus is part of the milk sinus within the teat.
The teat is the projecting part of the mammary gland containing part of the milk sinus. The papillary duct (teat canal) is the canal leading from the teat sinus to the teat opening and may be single or multiple. The ostium (teat opening) is the opening of the papillary duct and the exit point for milk or entrance point for bacteria. The sphincter consists of muscular fibres surrounding the teat opening that prevent milk flow except during suckling or milking. The teats are short in the mare. In late pregnancy, sebacious secretions, epithelial debris and colustrum escape and accumulate around the teat; giving it a waxy appearance. This 'waxing up' can be a sign of impending parturition.
Vasculature
Arteries
The main blood supply to the inguinal mammary glands is from the external pudendal artery. This arises indirectly from the external iliac artery via the deep femoral artery. The external pudendal artery passes through the inguinal canal.
Veins
The thoracic and cranial abdominal mammary glands drain via cranial superficial epigastric veins into the internal thoracic vein. Caudal abdominal and inguinal mammary glands drain via caudal superficial epigastric veins into the external pudendal vein.
Lymphatics
The more caudal mammary glands drain to the superficial inguinal lymph node and the more cranial mammary glands to the axillary or sternal lymph nodes.
Innervation
Somatic innervation is via the ventral rami of the spinal nerves. Mammary branches of the pudendal nerve supply the caudal aspect of the udder. There is sympathetic innervation to the blood vessels and teat sphincter smooth muscle. Mammary glands also have major influence from endocrine hormones.
Hoof
Introduction
The hoof is defined from a physiologic perspective as the modified skin covering the tip of the digit and all enclosed structures. The hoof provides protection to the distal limb and is formed by keratinisation of the epithelial layer and modification of the underlying dermis. The keratin in the epidermis, when thickened and cornified, is referred to as horn. Horn makes up the outer surface if the hoof and is particularly resistant to mechanical and chemical damage.
The origin of the hoof is as a form of protection to the distal phalanx and stems from local modifications of the epidermis, dermis and subcutaneous layers. The hoof also acts as a shock-absorber in that the hoof acts to reduce the concussion of foot impact on the structures of the distal limb. It has also been suggested that the elastic nature of components of the hoof may aid the return of blood to the heart.
General Structure and Layering of the Hoof
Wall
The wall of the hoof is the element of the hoof that is visible. The wall of the hoof is widest at the distal aspect of the hoof, i.e. at the toe. The wall of the hoof decreases in width laterally and medially (around the quarters of the hoof). There is an outer layer of thin but dense horn that is shiny and acts to reduce evaporation from the horn and therefore prevent dehydration of the other layers of the horn. There is an intermediate layer which represents the main structure of the wall and is composed of amorphous horn reinforced with many tubular shaped horn rods. Finally, there is an inner lamellar layer where there are interdigitating lamellae of horn and dermal lamellae which ensure the hoof itself is firmly anchored to the distal phalanx. The bond between the horn and the underlying dermis is a living bond that gradually allows the wall of the hoof to slide in a distal direction towards the ground where the distal border is worn away via contact with the ground.
Periople
The periople is a small band of soft tissue found over the proximal surface of the wall of the hoof. The periople represents the junction between the wall and the skin of the limb. The periople is responsible for the production of the outer layer of the wall (above). The periople segment extends around the proximal edge of the wall and in horses covers the bulb of the heel and part of the frog.
Coronary Dermis Segment
The wall of the hoof is created at the coronary dermis and grows in a distal direction from the coronary dermis. The coronary dermis is studded with many papillae which are directed towards the ground in the direction of growth. The epidermis covering these papillae produce horn tubules which are embedded into amorphous inter-tubular horn. This inter-tubular horn is created by the spaces between the papillae within the coronary dermis. The combination of both of these horn types ensures the horn has sufficient strength.
The pigmentation of the hoof is derived from melanocytes found in the coronary epidermis. Any pigmentation in the hoof will be most pronounced in the outer part of the hoof wall as the deeper layers of the hoof usually contain fewer melanocytes. It is this unpigmented element of the hoof that forms the white line in the sole of hoofs and is particularly important in horses as a landmark for shoeing.
Sole Segment
The sole represents the part of the foot in contact with the ground. The keratin found in the sole is formed from the epidermis on the underside of the distal phalanx and can grow to a thickness of around 10mm. The keratin found on the sole is much more easily worn down or abraded than that of the wall of the hoof. The equine sole has a central frog.
Frog-Bulb Segment
The equine bulb is formed from keratin in the same manner as the sole and again this keratin is softer and more liable that the keratin found in the hoof wall. The frog ensures that the wall of the hoof is forced outwards when weight is put on the limb thus ensuring that the 'hoof mechanism' functions correctly and ensuring circulatory flow around the hoof and back towards the heart.
Further information on the equine hoof, with particular reference to its role within the musculoskeletal system, can be found here.
{{Template:Learning
|OVAM = Equine Skin Histology 1
Equine Skin Histology 2