Difference between revisions of "Bluetongue Virus"
| Line 52: | Line 52: | ||
==Pathogenesis== | ==Pathogenesis== | ||
| − | + | ||
| − | + | The pathogenesis of BTV infection is similar in sheep and cattle, and most probably, all species of ruminants [4,19,21,26]. There are marked differences in the severity of disease that occurs in different ruminant species after BTV infection, however, with cattle being especially resistant to expression of BT disease. After cutaneous instillation of virus through the bite of a BTV-infected Culicoides vector the virus travels to the regional lymph node where initial replication occurs. The virus then is disseminated to a variety of tissues throughout the body where replication occurs principally in mononuclear phagocytes and endothelial cells. Viremia in BTV-infected ruminants is highly cell associated, and viremia is prolonged but not persistent especially in cattle [4,8,31]. The virus promiscuously associates with all blood cells, thus titers of virus in each cell fraction are proportionate to the numbers of each cell type; specifically, BTV is quantitatively associated most with platelets and erythrocytes and, because of the short lifespan of platelets, virus is most associated with erythrocytes late in the course of BTV infection of ruminants. BTV infection of erythrocytes facilitates both prolonged infection of ruminants and infection of hematophagous insect vectors that feed on viremic ruminants [9,10]. Interestingly, BTV nucleic acid may be detected by polymerase chain reaction (PCR) in the blood of infected cattle and sheep for many months after it no longer can be detected by virus isolation in cell culture or inoculation of susceptible sheep. Furthermore, ruminant blood that contains BTV nucleic acid as determined by PCR assay, but not infectious BTV as determined by virus isolation, is not infectious to vector insects even by intrathoracic inoculation [8,20,34]. | |
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
==Diagnosis== | ==Diagnosis== | ||
Revision as of 17:03, 20 August 2010
| This article is still under construction. |
Description
Bluetongue is a non-contagious, arthropod-borne disease of ruminants, caused by bluetongue virus (BTV). The clinical severity of disease is variable, but is characterised by inflammation of mucous membranes, haemorrhages and oedema1. Although cattle are the main reservoir of infection, sheep are more severely affected and often suffer a cyanotic tongue, lending the disease its name. The virus has been isolated from hosts and vectors on all continents(excluding Antartica)2, despite being initially recognised in Africa in the late 19th and early 20th centuries3. Originally thought to be a disease of tropical and sub-tropical regions, bluetongue has shown a propensity to become established in temperate areas, and in recent years has spread North, through the Mediterranean Basin, to become endemic in many European countries including the UK. Although BTV's transmission and epidemiology is dependent on insect vectors, bluetongue greatly influences the global trade of ruminants as it is included on the Office International des Epizooties List A of animal diseases4.
Aetiology
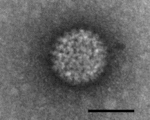
Bluetongue virus is a species of the genus Orbivirus, within the Reoviridae family. The Reoviridae are non-enveloped and possess a double-stranded RNA genome contained in an outer-shelled icosohedral capsid. The BTV genome is arranged into 10 segments and encodes 7 structural and 4 non-structural viral proteins2. The BTV receptor is currently unknown, but is proposed to included sialic acid and junctional adhesion molecules. After interaction with this receptor, the virus enters an endolysosome where the capsid is partially digested to allow the genome into the cell. Replication begins at this partially uncoated stage since the virus particles contain all the necessary enzymes5. First, the dsRNA is transcribed to form positive sense RNA, of which some is delivered to cytoplasm for ribosomal translation and the remainder is packaged into partially assembled virions. Complementary negative sense RNA is then formed in the virions, to give a dsRNA genome. Complete virus particles are released from the cell.
All BTV’s share group antigens, which can be demonstrated by agar gel diffusion tests, fluorescent antibody tests and the group reactive ELISA1. There are 24 distinct serotypes, which are are distinguished by epitopes on the outer capsid protein VP24, encoded by L2, the only serotype-specific BTV gene. Serotypes are differentiated using serum neutralisation tests, although there is some degree of cross-reactivity between serotypes1. Numerous strains of bluetongue virus also exist, and these are characterised by molecular analysis.
Hosts
All ruminants are susceptible to bluetongue virus infection, including sheep, goats, cattle, deer, buffaloes, camels and antelopes. Sheep are most severely affected, and disease is occasionally seen in goats. Although cattle BTV infection is significant in the epidemiology of disease, the condition is generally subclinical in this host. Mortalities in white-tailed deer due to bluetongue1.
Pigs and horses do not become infected with BTV, but may act as a food source for the Culicoides midges that transmit bluetongue virus to ruminants. Their habitats may also provide areas suitable for vector breeding.
Transmission and Epidemiology
BTV is transmitted by biting insects. Although vertical and venereal transmission between ruminant hosts can occur, it is insignificant in the overall epidemiology of bluetongue.
Vectors
The arthropod vector for bluetongue virus is the Culicoides biting midge. These insects take blood meals from vertebrate hosts and breed in damp, dung-enriched soil enriched, and so are abdunant in the vicinity of domestic livestock. Once eggs are laid in soil, Culicoides progresses through four larval stages and pupates before becoming an adult midge. The lifecycle is greatly influenced by temperature: in temperate regions such as Britain, the adult midge population declines in October and is absent by December. The fourth larval stage overwinters, and adults re-appear the following April. The environment affects the activity of adult midges in a variety of ways. Culicoides survive around 10 days in warm weather but up to one month when conditions are cooler and are most active at night, from an hour before sunset to an hour after sunrise. Activity is decreased by windy conditions, and increased during the day when the weather is dull. Bluetongue virus replicates more rapidly in vector species when temperatures are warmer.
Classically, the major vector for BTV is Culicoides imicola. This midge is found throughout Africa, the Middle East, southern Asia, Portugal, Greece, Corsica, Sardinia, Sicily and areas of Italy1, and its distribution appears to be extending northwards. However, C. imicola has not yet been demonstrated in the United Kingdom. The Culicoides species found in the British Isles are C. pulicais and C. obsoletus, which are also common across central and northern Europe. Knowledge of the distribution of these species in the UK is incomplete but the insects tend to gather where breeding sites and hosts occur in tandem, with the highest midge concentrations in areas containing cattle, horses and pigs. Removal of livestock decreases populations of Culicoides by a factor of 10 to 201, but some persist by feeding on wild animals and man. Hill sites have fewer midges as climatic conditions are less favourable, and sheep have a less positive influence on distribution.
In Britain, studies are ongoing to determine midge distribution, seasonal incidence and the competency of the various Culicoides species to act as BTV vectors.
Vector Competence
Certain information can help inferences be made regarding BTV vectors in Britain. Both C. obsoletus and C. pulicaris have been implicated in transmission before. Previously, BTV has been isolated from C. obsoletus in Cyprus, and African horse sickness virus (another Orbivirus) in Spain. C. obsoletus and C. pulicaris were also the most abundant Culicoides species detrected in the 1999 BTV epizootic in Greece and Bulgaria, and so are strongly suspected of acting as vectors in this case. They may also have mediated outbreaks in Serbia, FYR Macedonia, Croatia and Bosnia in 2001-2002, where C. imicola has not been recorded. Both species are therefore contenders to transmit bluetongue virus in the UK.
A British population of C. obsoletus has been shown to have and oral susceptibility rate of less than 2%1, suggesting that C. obsoletus is likely to be an inefficient or minor vector of BTV in the UK. However, it is possible that a high abundance or survival rate may compensate for this low vector competence. Indeed, C. brevitarsis, the major Australian vector of BTV, has an extremely low experimental competency yet is an effective vector in the field.
Two other Culicoides species, C. nuberculous and C. impunctatus, exist in mainland Europe and the UK, and have been experimentally infected with bluetongue virus.
Epidemiology
Althbough bluetongue virus is capable of infecting any ruminant, cattle are the main amplifying and maintenance hosts and are most abundantly fed on by Culicoides vectors. Infection of sheep with BTV is therefore usually preceded by widespread infection of cattle and an increase in vector density1.
Although vertical and venereal transmission of bluetongue is possible, only to the presence of competent insect vectors influences the epidemiology of BTV2. This is illustrated by the fact that bluetongue virus is limited to geographical areas where competent vectors are present and that transmission only occurs at times of the year when conditions are favourably for vector activity1. In Britain, transmission occurs mainly in late summer and autumn. Once bluetongue virus is transmitted to a vertebrate host, there are two possible outcome: either the host may die, or an immune response is mounted against the virus and renders the host resistant to re-infection. Either way, animals quickly become "unavailable" for BTV infection as the virus spreads, particularly where livestock populations are small. This presents a hurdle that must be surmounted if bluetongue virus is to persist in an area. By movement of infected vectors or viraemic animals, BTV can become established in new locations with naive hosts in order to overcome this obtascle. This means that even in zones where bluetongue virus is endemic, persistence dynamic and comprises perpetually shifting "hot spot" of infection1. Creation of an enzootic zone is only possible in locations where adult midges are present throughout the year since bluetongue cannot be maintained through vertebrate-vertebrate or vector transovarial transmission. Any points where vectores are absent from the system must not exceed the maximum duration of viraemia in the ruminant host, otherwise the last infected vertebrate will have died or recovered by the time new vectors are availble for onwards transmission.
In some areas, bluetongue can occur in annual bouts. This may be due to new introduction of virus each year from adjacent areas where the disease is endemic, via the transportation of Culicoides on the wind for up to 100 kilometres. Alternatively, this could be the manifestation of low-level persistence.
Introduction of bluetongue virus to a new area has the potential to occur in several ways. Firstly, infected animals may be transported to the region, and local insect vectors could spread and perpetuate BTV infection within naive animals. It is also possible that local vectors could acquire BTV from infected animals in neighbouring areas, where there is a cross-over in the distribution of Culicoides species. Finally, infected vectors can be acquired from areas where bluetongue infection exists. Culicoides can be transported considerable distances on the wind, and it is also conceivable that the distribution of competent vectors may expand to colonise previously unpopulated areas under the influence of climate change.
Bluetongue virus infection was first confirmed in the UK in September 2007 when a veterinarian spotted suspicious clinical signs on a cattle holding near Ipswich6. It is believed that BTV-laden vectors were dispersed to the UK on the wind, since meteorological conditions on 4th August 2007 were capable of carrying midges from northern Europe to East Anglia. This would be expected to produce disease at a point that would coincide with the first case, given the time necessary for clinical detection to occur.
Pathogenesis
The pathogenesis of BTV infection is similar in sheep and cattle, and most probably, all species of ruminants [4,19,21,26]. There are marked differences in the severity of disease that occurs in different ruminant species after BTV infection, however, with cattle being especially resistant to expression of BT disease. After cutaneous instillation of virus through the bite of a BTV-infected Culicoides vector the virus travels to the regional lymph node where initial replication occurs. The virus then is disseminated to a variety of tissues throughout the body where replication occurs principally in mononuclear phagocytes and endothelial cells. Viremia in BTV-infected ruminants is highly cell associated, and viremia is prolonged but not persistent especially in cattle [4,8,31]. The virus promiscuously associates with all blood cells, thus titers of virus in each cell fraction are proportionate to the numbers of each cell type; specifically, BTV is quantitatively associated most with platelets and erythrocytes and, because of the short lifespan of platelets, virus is most associated with erythrocytes late in the course of BTV infection of ruminants. BTV infection of erythrocytes facilitates both prolonged infection of ruminants and infection of hematophagous insect vectors that feed on viremic ruminants [9,10]. Interestingly, BTV nucleic acid may be detected by polymerase chain reaction (PCR) in the blood of infected cattle and sheep for many months after it no longer can be detected by virus isolation in cell culture or inoculation of susceptible sheep. Furthermore, ruminant blood that contains BTV nucleic acid as determined by PCR assay, but not infectious BTV as determined by virus isolation, is not infectious to vector insects even by intrathoracic inoculation [8,20,34].
Diagnosis
The typical clinical signs of bluetongue enable a presumptive diagnosis, especially in areas where the disease is endemic. Suspicion is confirmed by the presence of petechiae, ecchymoses, or hemorrhages in the wall of the base of the pulmonary artery and focal necrosis of the papillary muscle of the left ventricle. These highly characteristic lesions are usually obvious in severe clinical infections but may be barely visible in mild or convalescent cases. These lesions are often described as pathognomonic for bluetongue, but they have also been observed occasionally in other ovine diseases such as heartwater, pulpy kidney disease, and Rift Valley fever. Hemorrhages and necrosis are usually found where mechanical abrasion damages fragile capillaries, such as on the buccal surface of the cheek opposite the molar teeth and the mucosa of the esophageal groove and omasal folds. Other autopsy findings include subcutaneous and intermuscular edema, skeletal myonecrosis, myocardial and intestinal hemorrhages, hydrothorax, hydropericardium, pericarditis, and pneumonia. In many areas of the world, bluetongue in sheep, and especially in other ruminants, is subclinical and, therefore, laboratory confirmation based on virus isolation in embryonated chicken eggs, susceptible sheep, or cell cultures, or the identification of viral RNA by PCR is necessary. The identity of isolates may be confirmed by the group-specific antigen-capture ELISA, immunofluorescence, immunoperoxidase, serotype-specific virus neutralization tests, or hybridization with complementary gene sequences of group- or serotype-specific genes. For virus isolation, blood (10-20 mL) is collected as early as possible from febrile animals into an anticoagulant such as heparin, sodium citrate, or EDTA and transported at 4°C to the laboratory. For longterm storage where refrigeration is not possible, blood is collected in oxalate-phenol-glycerin (OPG). Blood to be frozen should be collected in buffered lactose peptone and stored at or below -70°C. Blood collected at later times during the viremic period should not be frozen, as lysing of the RBC or thawing releases the cell-associated virus, which may then be neutralized by early humoral antibody. The virus does not remain stable for long at -20°C. In fatal cases, specimens of spleen, lymph nodes, or red bone marrow are collected and transported to the laboratory at 4°C as soon as possible after death. A serologic response in ruminants can be detected 7-14 days after infection and is generally lifelong. Current recommended serologic techniques for the detection of bluetongue virus antibody include agar gel immunodiffusion and competitive ELISA. The latter is the test of choice and does not detect cross-reacting antibody to other orbiviruses, especially anti-EHDV (epizootic hemorrhagic disease virus) antibody. Various forms of virus neutralization test, including plaque reduction, plaque inhibition, and microtiter neutralization can be used to detect type-specific antibody.
Clinical Signs
The course of the disease in sheep can vary from peracute to chronic, with a mortality rate of 2-30%. Peracute cases die within 7-9 days of infection, mostly as a result of severe pulmonary edema leading to dyspnea, frothing from the nostrils, and death by asphyxiation. In chronic cases, sheep may die 3-5 wk after infection, mainly as a result of bacterial complications, especially pasteurellosis, and exhaustion. Mild cases usually recover rapidly and completely. The major production losses include deaths, unthriftiness during prolonged convalescence, wool breaks, and possibly reproductive loss. In sheep, bluetongue virus causes vascular endothelial damage, resulting in changes to capillary permeability and subsequent intravascular coagulation. This results in edema, congestion, hemorrhage, inflammation, and necrosis. The clinical signs in sheep are typical. After an incubation period of 4-6 days, a fever of 105-107.5°F (40.5-42°C) develops. The animals are listless and reluctant to move. Clinical signs in young lambs are more apparent, and the mortality rate is higher (up to 30%). About 2 days after onset of fever, additional clinical signs such as edema of lips, nose, face, submandibular area, eyelids, and sometimes ears; congestion of mouth, nose, nasal cavity, conjunctiva, and coronary bands; and lameness and depression may be seen. A serous nasal discharge is common, later becoming mucopurulent. The congestion of nose and nasal cavity produces a “sore muzzle” effect, the term used to describe the disease in sheep in the USA. Sheep eat less because of oral soreness and will hold food in their mouths to soften before chewing. They may champ to produce a frothy oral discharge at the corners of the lips. On close examination, small hemorrhages can be seen on the mucous membranes of the nose and mouth. Ulceration develops where the teeth come in contact with lips and tongue, especially in areas of most friction. Some affected sheep have severe swelling of the tongue, which may become cyanotic (‘blue tongue”) and even protrude from the mouth. Animals walk with difficulty as a result of inflammation of the hoof coronets. A purple-red color is easily seen as a band at the junction of the skin and the hoof. Later in the course of disease, lameness or torticollis is due to skeletal muscle damage. In most affected animals, abnormal wool growth resulting from dermatitis may be observed. The pathogenesis of bluetongue in cattle seems to differ from that in sheep and is based on immediate IgE hypersensitivity reactions. Clinical signs in cattle are rare but may be similar to those seen in sheep. They are usually limited to fever, increased respiratory rate, lacrimation, salivation, stiffness, oral vesicles and ulcers, hyperesthesia, and a vesicular and ulcerative dermatitis. Susceptible cattle and sheep infected during pregnancy may abort or deliver malformed calves or lambs. The malformations include hydranencephaly or porencephaly, which results in ataxia and blindness at birth. White-tailed deer and pronghorn antelope develop severe hemorrhagic disease leading to sudden death. Pregnant dogs abort or give birth to stillborn pups and then die in 3-7 days.
Laboratory Tests
Pathology
Complete loss of integrity of epithelium. Uncommon.
- Characteristic of Bluetongue Virus,
- Epithelium lost and haemorrhage produces blue / black discoloration of the tongue, hence the name.
- Grossly:
- Infarctions -> necrosis
- Haemorrhage
- Histologically:
- Necrosis -> calcification or regeneration (depends on age of lesion)
Treatment
- BTV is NOTIFIABLE
- Vigilance in recognizing clinical signs
- Restriction of movement:
- Protection Zone: 100km radius around infected premises, movement within zone allowed but not in or out
- Vaccination within PZ using appropriate serotype is encouraged but still voluntary
- Surveillance Zone: 50km radius beyond PZ
- Protection Zone: 100km radius around infected premises, movement within zone allowed but not in or out
- Vector control: ectoparasiticides, etc.
Prophylactic immunization of sheep remains the most effective and practical control measure against bluetongue in endemic regions. Three polyvalent vaccines, each comprising 5 different bluetongue virus serotypes attenuated by serial passage in embryonated hens’ eggs followed by growth and plaque selection in cell culture, are widely used in southern Africa and elsewhere, should epizootics of bluetongue occur. A monovalent modified live virus vaccine propagated in cell culture is available for use in sheep in the USA. Live-attenuated vaccines should not be used during Culicoides vector seasons because they may transmit the vaccine virus(es) from vaccinated to nonvaccinated animals, eg, other ruminant species. This may result in reassortment of genetic material and give rise to new viral strains. Abortion or malformation, particularly of the CNS, of fetuses may follow vaccination of ewes and cows with attenuated live vaccines during the first half and the first trimester of pregnancy, respectively. Passive immunity in lambs usually lasts 4-6 mo. The control of bluetongue is different in areas where the disease is not endemic. During an outbreak, when one or a limited number of serotypes may be involved, vaccination strategy depends on the serotype(s) that are causing infection. Use of vaccine strains other than the one(s) causing infection affords little or no protection. The vector status, potential risk from vaccine virus reassortment with wild-type viral strains, virus spread by the vectors to other susceptible ruminants, and reversion to virulence of vaccine virus strains or even the production of new serotypes also should be considered. Although a number of noninfectious vaccines are in development, they are not yet commercially available. Control of vectors by using insecticides or protection from vectors by moving animals into barns during the evening hours lowers the number of Culicoides bites and subsequently the risk of exposure to bluetongue virus infection.
Links
- Defra - Bluetongue
- BTV Control in Cattle and Sheep (Intervet)
- Institute for Animal Health - Bluetongue
- Bluetonguevirus.org - BTV information and resource portal
References
- DEFRA (2002) Technical Review - Bluetongue : The Virus, Hosts and Vectors.
- Gibbs, E P J and Geiner, E C (1994) The Epidemiology of Bluetongue. Comparative Immunology, Microbiology and Infectious Diseases, 17(3-4), 207-220.
- Spreull, J (1905) Malarial catarrhal fever (bluetongue) of sheep in South Africa. Journal of Comparative Pathology and Therapeutics, 18, 321-337.
- MacLachlan, N J (2004) Bluetongue: A Review and Global Overview of the Only OIE List a Disease that is Endemic in North America. Proceedings of the 55th Annual Meeting of the American College of Veterinary Pathologists (ACVP) and 39th Annual Meeting of the American Society of Clinical Pathology (ASVCP), p1237.
- Carter, G R and Wise, D J (2005) A Concise Review of Veterinary Virology, IVIS.
- IAH (2008) Institute for Animal Health - Bluetongue Research Programme
- Mullens, B A et al (1995) Effects of temperature on virogenesis of bluetongue virus serotype 11 in Culicoides variipennis sonorensis. Medical and Veterinary Entomology, 9, 71-76.
- Gould, A R and Hyatt, A D (1994) The orbivirus genus: diversity, structure, replication and phylogenetic relationships. Comparative Immunology, Microbiology and Infectious Diseases, 1, 163-188.
- Merck & Co (2008) The Merck Veterinary Manual (Eighth Edition), Merial.
- Dal Pozzo, F et al (2009) Bovine infection with bluetongue virus with special emphasis on European serotype 8. The Veterinary Journal, 182(2), 142-151.
- MacLachlan, N J et al (2009) The Pathology and Pathogenesis of Bluetongue. Journal of Comparative Pathology, 141(1), 1-16.
- Barratt-Boyes, S M and MacLachlan, N J (1995) Pathogenesis of bluetongue virus infection of cattle. Journal of the American Veterinary Medical Association, 206(9), 1322-1329.
- Afshar, A (2004) Bluetongue: Laboratory Diagnosis. Comparative Immunology, Microbiology and Infectious Diseases, 17(3-4), 221-242.
- Gould, E A and Higgs, S (2009) Impact of climate change and other factors on emerging arbovirus diseases. Transactions of the Royal Society of Tropical Medicine and Hygiene, 103(2), 109-121.
- MacLachlan, N J (1994) The pathogenesis and immunology of bluetongue virus infection of ruminants. Comparative Immunology, Microbiology and Infectious Diseases, 17(3-4), 197-206.