Difference between revisions of "Dirofilaria immitis"
| Line 93: | Line 93: | ||
In both dogs and cats, routine haematology, biochemistry and urinalysis should be performed. Most parameters are usually within normal limits, but an anaemia can often be seen. Eosinophilia and basophilia are also common, and when seen together suggests occult dirofilariasis or allergic lung disease <sup>1, 3</sup>. Eosinophilia peaks as L5 enter the pulmonary arteries and subsequently varies. An inflammatory leukogram is also possible<sup>3</sup>. Hyperglobulinemia due to antigenic stimulation is an inconsistent finding<sup>1, 3</sup>. Right-sided heart failure or immune-complex glomerulonephritis can lead to hypoalbuminaemia and, very occasionally, nephrotic syndrome<sup>1</sup>. Because of this, it is possible for urinalysis to reveal proteiunuria<sup>1, 3</sup>. Haemoglobinaemia and haemoglobinuria are associated with caval syndrome<sup>3</sup>. | In both dogs and cats, routine haematology, biochemistry and urinalysis should be performed. Most parameters are usually within normal limits, but an anaemia can often be seen. Eosinophilia and basophilia are also common, and when seen together suggests occult dirofilariasis or allergic lung disease <sup>1, 3</sup>. Eosinophilia peaks as L5 enter the pulmonary arteries and subsequently varies. An inflammatory leukogram is also possible<sup>3</sup>. Hyperglobulinemia due to antigenic stimulation is an inconsistent finding<sup>1, 3</sup>. Right-sided heart failure or immune-complex glomerulonephritis can lead to hypoalbuminaemia and, very occasionally, nephrotic syndrome<sup>1</sup>. Because of this, it is possible for urinalysis to reveal proteiunuria<sup>1, 3</sup>. Haemoglobinaemia and haemoglobinuria are associated with caval syndrome<sup>3</sup>. | ||
| − | There are several methods for the specific demonstration of ''Dirofilaria immitis'' in the animal. Firstly, direct microscopic examination allows rapid identification microfilariae in a drop of fresh blood as their movements can vigorously displace the surrounding red blood cells<sup>2</sup>. Despite being quick, simple and inexpensive, this test is not sufficiently sensitive to provide a definitive diagnosis, particularly when there is a low concentration of microfilariae in the bloodstream. Filtration methods therefore exist to facilitate the microscopic demonstration of microfilariae. These include the modified Knott's test, which involves haemolysis, centrifugation and staining with methylene blue before direct examination. Tests such as this are more | + | There are several methods for the specific demonstration of ''Dirofilaria immitis'' in the animal. Firstly, direct microscopic examination allows rapid identification microfilariae in a drop of fresh blood as their movements can vigorously displace the surrounding red blood cells<sup>2</sup>. Despite being quick, simple and inexpensive, this test is not sufficiently sensitive to provide a definitive diagnosis, particularly when there is a low concentration of microfilariae in the bloodstream. Filtration methods therefore exist to facilitate the microscopic demonstration of microfilariae<sup>2, 3</sup>. These include the modified Knott's test, which involves haemolysis, centrifugation and staining with methylene blue before direct examination. Tests such as this are more sensitive than merely examining a drop of blood, and the morphology of microfilariae can be clearly seen. Sensitivity in comparison to other methos is still, however, low and so microfilarial identification tests are often reserved for confirmation of weak positive antigen tests and determination of microfilarial status prior to treatment with a microfilaricide<sup>3</sup>. Cats frequently lack circulating microfilariae, and so direct micrscopic examination is of little use in this species. |
| − | sensitive than merely examining a drop of blood, and the morphology of microfilariae can be clearly seen. | ||
Antigen tests | Antigen tests | ||
Revision as of 09:15, 26 August 2010
| This article is still under construction. |
Also known as: heartworm disease.
Do not confuse with: Angiostrongylus vasorum, angiostrongylosis.
Description
Dirofilaria immitis is a nematode parasite that causes heartworm disease in dogs, cats and ferrets. Heartworm disease is transmitted by mosquito bites and there are more than 70 species of mosquito that are able to transmit infection; Aedes, Anopheles and Culex are the most common vector species. Heartwoem disease has been reported in many countries with temperate and is particularly prevalent in the USA, Canada, and southern Europe. The introduction of the PETS travel scheme has increased the concern over Dirofilariasis in the UK.
Dirofilarias does have zoonotic potential: infected mosquitos can transmit Dirofilaria immitis to humans, but the infection does not become patent. The infective larvae instead reach the lungs, become encapsulated, and die causing granulomatous reactions called "coin lesions" in the process. These are only imporant because they may be confused with neoplastic metastasis to the lungs on radiography1.
Life Cycle
Dirofilaria immitis adults reach maturity and sexually reproduce in the pulmonary arteries and right ventricle. Adult males are around 15cm in length, and females are around 25cm1. After mating, female worms release larvae known as microfilariae (or L1) into the circulation. When a mosquito takes a blood meal from the infected dog or cat, microfilariae are ingested. Mosquitos are true intermediate hosts for Dirofilaria immitis, since microfilariae require a period of maturation to L2 then L3 in the vector. The duration of this development depends upon environmental conditions. For example, maturation at 30°C takes around 8 days, but when temperatures are down to 18°C, this takes around one month2. Below 14°C, development is halted and resumes when temperatures rise. In cooler climates, this means that transmission of heartworm disease to new canine or feline hosts can only occur in warmer months.
Once matured, L3 in the mosquito migrate to the labium, from which they erupt onto the host's skin as the mosquito feeds. Larvae then migrate into the bite wound and, as most dogs are highly susceptible to heartworm disease, most L3 then establish infection. It takes 2-3 days for L3 to moult to L4, which remain in the subcutaneous tissues for up to two months before becoming young adults (L5) and migrating to the pulmonary arteries.
Cats differ from dogs in that they are more resistant to infection with Dirofilaria immitis. A lower percentage of exposed cats develop adult infections, and when this does occur the burden is usually low1. L5 in the pulmonary arteries also have a relatively short (2 year) survival time in cats.
Pathogenesis
Heartworm disease primarily affects the cardiopulmonary system and the severity and extent of lesions depends several factors. These include the number and location of adult worms1, 2, the duration of infection, and the level of activity of the host1. Parasites in the pulmonary arteries cause mechanical irritation, leading to endothelial damage, proliferation of the intima and perivascular cuffing with inflammatory cells. This results in narrowing and occlusion of the vessels which in turn causes pulmonary hypertension. A combination of pulmonary hypertension and inflammatory mediators can lead to in an increase in the permeability of pulmonary vessels, giving periarterial oedema and intersitial and alveolar infiltrates. Eventually, irreversible interstitial fibrosis arises.
Sequelae to heartworm infection include pulmonary thromboembolism, which can either occur due to the death and metastasis of adult worms, or due to platelet aggregation induced by the parasite. In severe cases, live nematodes can migrate to the right ventricle, right atrium and caudal vena cava. The resulting incompetence of the tricuspid valve, augmented by concurrent pulmonary hypertension, leads to signs of right-sided heart failure. Flow of erythrocytes through the mass of parasites formed can also cause haemolysis and thus haemoglobinaemia. This combination of acute right-sided heart failure and intravascular haemolysis is referred to as "caval syndrome", which in severe cases can also be characterised by thromboembolic events and disseminated intravascular coagulation. Due to the smaller numbers of adult worms, caval syndrome is less common in cats2.
In cats, heartworm disease generally causes a diffuse pulmonary infiltrate and an eosinophilic pneumonia2. Adult worms may die and embolise to the lungs, resulting in severe haemorrhage and oedema of the affected lobe. Immature nematodes have also been known to migrate to sites other than the pulmonary arteries and heart such as the CNS, eye and subcutaneous tissues. These ectopic infections are far more common in cats than in dogs, suggesting that D. immitis is not well adapted to feline hosts.
Signalment
Dirofilaria immitis infection affects dogs more commonly than cats, and risk is greatest in outdoor animals. Dogs of any age may be affected, but infections are most common in 3 to 8 year old dogs, and medium and large breeds are over-represented1, 3. In cats, there are no breed or age predispositions, but males are more frequently affected3. Ferrets may also contract dirofilariasis; there are no age or sex predilections1.
Diagnosis
Clinical Signs
In dogs, historical findings at the time of presentation can vary. Some animals are asymptomatic, or cough only occasionally. In countries where heartworm is endemic, animals may be routinely tested for dirofilariasis at the end of the high-risk season, when weather becomes cooler3. Therefore, positive laboratory testing may be the first indication of disease1. More obvious signs may be seen depending on the severity of disease. Generally, the onset of heartworm disease is insidious, and clinical signs are related either to a high parasite burden, or to an allergic response to the parasite2. Affected dogs most often show coughing, and dyspnoea/tachypnoea, exercise intolerance, loss of condition and syncope may also be seen. In severe cases the pulmonary vessels may rupture, leading to haemoptysis or epistaxis. There is a tendency for signs to only manifest during exercise, and so patients with a sedentary lifestyle may never show overt disease. Right-sided congestive heart failure may ensue when worm burden is high, and signs can include jugular disension, ascites, marked exercise intolerance and hepatomegaly. A systolic murmur is sometimes audible on cardiac auscultation.
A classification system for the presentation of heartworm disease exists1, outlined in the table below.
Asymptomatic or mild disease
| |
Moderate disease
| |
Severe disease
| |
Caval syndrome
|
Caval syndrome is a very severe form of heartworm disease that can occur in dogs and cats. It is characterised by respiratory distress, signs of right-sided heart failur, intravascular haemolysis and haemoglobinuria. Disseminated intravascular coagulation frequently occurs, and the syndrome is often fatal.
In cats, most infections are asymptomatic. However, sudden death can occasionally occur. This may be preceded by an acute respiratory crisis, thought to be due to parasitic thromboembolism and obstruction of a major pulmonary artery1, 2. When clinical signs are less acute, they are vague and may include anorexia, weight loss and letheargy. Intermittent coughing and dyspnoea can appear similar to feline asthma. Syncope may also occur, and cats may vomit. The cause of this vomiting is undetermined3.
Radiography
In dogs, thoracic radiography provides good information on disease severity and is useful for screening dogs showing clinical signs compatible with D. immitis infection1. However, thoracic radiograph do not neccessarily reflect the current worm burden: radiographic signs of advanced disease can persist long after an infection has run its course4. Conversely, dogs with high burdens may be inactive and thus show few clinical signs or radiographic changes. Radiographic signs are mild-to-moderate in class II disease, but become more obvious in class III infections. The main pulmonary artery is enlarged,sup>1, 4, and the caudal lobar vessels appear tortuous1 Ill-defined, fluffy infiltrates are apparent, and often surroung in the caudal lobar vessels. Right-sided cardiomegaly may be appreciated, and pleural and peritoneal effusions can be noted if right-sided congestive heart failure occurs4.
Cardiac changes on thoracic radiography are less common in cats than dogs. The caudal lobar veins are enlarged (greater than 1.5 times the width of the ninth ribe), and the pulmonary arteries are blunted and tortuous3, 5. Patchy parenchymal infiltrates may be seen in the region of vessels in animals showing respiratory signs1, 3. Enlargement of the main pulmonary artery cannot normally be seen in cats, as it is has a relatively midline position and is thus obscured by the cardiac silhouette1, 5. Right-sided cardiomegaly is not considered a typical finding in the cat5.
Echocardiography
In dogs, echocardiography is not particularly useful as a diagnostic tool for heartworm disease. In severe, chronic pulmonary hypertansion, right ventricular hypertrophy, septal flattening, underloading of the left heart, and high-velocity tricuspid and pulmonic regurgitation may be seen1. With caval syndrome or high-burden infections, worms may be visualised in the right heart and vena cava.
Echocardiography is more important in cats than dogs because of the increased difficulty of diagnosis and the fact that this test can have a high sensitivity depending on operater experience1. Specificity is 100%5, and the test can help exclude or confirm other primary cardiac diseases such as hypertrophic cardiomyopathy3. Worms can usually be visualised as parallel hyperechoic lines1, and are seen in the right atrium and ventricle and main pulmonary artery1, 3, 5.
Electrocardiography
The ECG of infected dogs is usually normal. Right ventricular hypertrophy patterns are seen when there is severe, chronic pulmonary hypertension and are associated with overt or impending right-sided CHF (ascites). Heart rhythm disturbances are usually absent or mild, but atrial fibrillation is an occasional complication in dogs with Class III disease.
Laboratory Tests
In both dogs and cats, routine haematology, biochemistry and urinalysis should be performed. Most parameters are usually within normal limits, but an anaemia can often be seen. Eosinophilia and basophilia are also common, and when seen together suggests occult dirofilariasis or allergic lung disease 1, 3. Eosinophilia peaks as L5 enter the pulmonary arteries and subsequently varies. An inflammatory leukogram is also possible3. Hyperglobulinemia due to antigenic stimulation is an inconsistent finding1, 3. Right-sided heart failure or immune-complex glomerulonephritis can lead to hypoalbuminaemia and, very occasionally, nephrotic syndrome1. Because of this, it is possible for urinalysis to reveal proteiunuria1, 3. Haemoglobinaemia and haemoglobinuria are associated with caval syndrome3.
There are several methods for the specific demonstration of Dirofilaria immitis in the animal. Firstly, direct microscopic examination allows rapid identification microfilariae in a drop of fresh blood as their movements can vigorously displace the surrounding red blood cells2. Despite being quick, simple and inexpensive, this test is not sufficiently sensitive to provide a definitive diagnosis, particularly when there is a low concentration of microfilariae in the bloodstream. Filtration methods therefore exist to facilitate the microscopic demonstration of microfilariae2, 3. These include the modified Knott's test, which involves haemolysis, centrifugation and staining with methylene blue before direct examination. Tests such as this are more sensitive than merely examining a drop of blood, and the morphology of microfilariae can be clearly seen. Sensitivity in comparison to other methos is still, however, low and so microfilarial identification tests are often reserved for confirmation of weak positive antigen tests and determination of microfilarial status prior to treatment with a microfilaricide3. Cats frequently lack circulating microfilariae, and so direct micrscopic examination is of little use in this species.
Antigen tests ELISA antigen tests detect specific circulating proteins released by the reproductive tract of mature female worms. These are available as either in-house or laboratory tests and their sensitivity and specificity approach 100 per cent (see top table on page 354). The antigen levels become undetectable eight to 12 weeks after adulticidal therapy and this should be taken into account when re-screening for heartworm disease or evaluating the response to treatment. Small worm burdens, the presence of immature females or male-only infections are common causes of low antigen titres and false negative results, especially in cats, where these circumstances occur more frequently. In dogs, specific agglutination and immunochromatography techniques are also available. An antigen test performed too soon after infection (first six to seven months) may yield false negative results because of the low antigen levels in the circulating blood.
Antibody tests are currently available for routine screening of feline heartworm infection, either as in-house or laboratory tests (see table below). The presence of antibodies provides information about previous exposure, but not necessarily current infection. Consequently, antibody tests are more useful to help rule out infection rather than confirm it. These tests are no longer used in dogs given their low specificity and the availability of highly reliable antigen tests. PCR-based tests Polymerase chain reaction (PCR)-based tests offer a very sensitive and specific diagnostic tool for routine identification of mature and immature adult worms, especially in unconventional hosts. However, at present, these tests are not widely available.
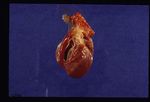
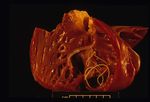
Pathology
On post-mortem examination, the right side of the heart is found to be enlarged. There is proliferation of the pulmonary arterial myointima, as well as pulmonary thromboembolism and haemorrhage. If right-sided congestive heart failure was present in life, the hepatomegaly and hepatic congestion will be seen.
Treatment
Adulticidal Treatment
Decisions in the treatment of heartworm disease are dependent on the severity of infection. A scheme exists to classify patients in terms of disease severity2. Class one patients have subclinical heartworm disease, and carry an excellent prognosis following treatment wiht adulticidal drugs. Class two animals show mild to moderate clinical signs and similar radiographic changes. These animals may respond positively to treatment. Dogs with class 3 disease have severe clinical signs, such as persistent coughing, dyspnoea, right-sided heart failure or haemoptysis, and these are reflected by severe radiographic signs. These cases have a high risk of pulmonary thromboembolism and so prognosis is guarded and the benefits of adulticidal treatment should be considered carefully.
Even low grade infections in cats may result in pulmonary thromboembolism with adulticidal treatment, and spontaneous remission is seen in some cats. Because of this, symptomatic treatment (cage rest, oxygen supplementation, fluid therapy, bronchodilators and dexamethasone) may be more appropriate in sick cats, and clinically well cats can merely be monitored regularly for remission. Adulticidal treatment should only be considered in cats that fail to respond to supportive treatments but are in a stable condition.
Adulticidal treatment involves the administration of a new generation arsenical compound, melarsomine dihydrochloride (Immiticide, Merial; this product is not licensed for use in the UK). Melarsomine is less nephrotoxic and hepatotoxic than its predecessor thiacetarsamide, and has a higher efficacy. Melarsomine is injected intramuscularly into the lumbar muscles at a recommended dose of 2-5 mg/kg, repeated after 24 hours. However, only a single dose should be administered to class 3 dogs, to kill just a proportion of worms and hence minimise the risk of pulmonary thromboembolism. If the patient remains stable, the standard adulticidal protocol can be administered one month later. In the week following the administration of melarsomine, the likelihood of pulmonary thromboembolism can be minimised with cage rest and corticosteroids at anti-inflammatory doses. If adulticidal treatment is declined by the owner, monthly administration of prophylactic doses of ivermectin may represent a reasonable option because it will prevent further infection and may kill some adult nematodes. Patients with severe caval syndrome may benefit from physical removal of worms from the right side of the heart and the main pulmonary artery using flexible crocodile or basket-type retrieval forceps. This procedure is complex, requires general anaesthesia and fluoroscopic imaging, but may reduce the risk of thromboembolism following subsequent adulticidal treatment.
Microfilaricidal Treatment
No drugs are specifically approved for microfilaricidal treatment of Dirofilaria immitis, and successful elimination of adult worms should results in the demise of circulating microfilariae four to six weeks later2. Single doses of ivermectin, milbemycin oxime, moxidection or selamectin are, however, effective at removing microfilariae from the circulation. The sudden death of large numbers of microfilariae may invoke an anaphylactic response, and oral prednisolone may be administered with microfilaricides to help prevent this.
Prevention
Heartworm prophylaxis should be implemented in all cats and dogs living in or visiting areas in which Dirofilaria immitis is endemic. In the UK, milbemycin oxime and selamectin are licensed for the prevention of heartworm disease and should be administered on a monthly basis as they are capable of killing migrating larvae up to week six post-infection. In the event of non-compliance or a missed dose, it may be necessary to test the animal for Dirofilaria immitis six months later if they are likely to have been exposed to infection during the time they were unprotected. Drugs that persist in the long term, such as injectable moxidectin, can help overcome this issue.
Prognosis
In mildly symptomatic or asymptomatic animals, the course of dirofilariasis is usually uneventful following treatment and the prognosis is excellent3. Animals with severe infection carry a guarded prognosis with a higher risk of complications.
Links
References
- Merck & Co (2008) The Merck Veterinary Manual (Eighth Edition), Merial.
- Ferasin, L (2004) Disease risks for the travelling pet: Heartworm disease, In Practice, 26(6), 350-357.
- Tilley, L P and Smith, F W K (2004) The 5-minute Veterinary Consult (Fourth Edition),Blackwell.
- Venco, L (2007) Heartworm (Dirofilaria immitis) disease in dogs. Dirofilaria immitis and D. repens in dog and cat and human infections, 117-125.
- Venco, L (2007) Heartworm (Dirofilaria immitis) disease in cats. Dirofilaria immitis and D. repens in dog and cat and human infections, 126-132.
- Ridyard, A (2005) Heartworm and lungworm in dogs and cats in the UK, In Practice, 27(3), 147-153.