Difference between revisions of "Lamb Dysentery"
| (11 intermediate revisions by 2 users not shown) | |||
| Line 1: | Line 1: | ||
| − | + | Also known as: '''''Clostridium perfringens'' type B Enterotoxaemia | |
| − | + | ==Introduction== | |
| − | + | Lamb dysentery is a peracute and fatal enterotoxaemia of young lambs caused by the beta and epsilon toxins of ''Clostridium perfringens'' type B. ''C. perfringens'' is a large, gram positive, anaerobic bacillus that is ubiquitous in the environment and commensalises the gastrointestinal tract of most mammals<sup>1</sup>. Five genotypes of ''Clostridium perfringens'' exist, named A-E, and all genotypes produce potent exotoxins. There are 12 exotoxins in total, some of which are lethal and others which are of minor significance<sup>2</sup>. These are produced as pro-toxins, and are converted to their toxic forms by digestive enzymes. The enterotoxaemias are a group of diseases caused by proliferation of ''C. perfringens'' in the lumen of the gastrointestinal tract and excessive production of exotoxin. | |
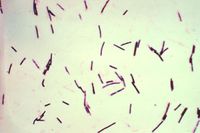
| + | [[Image:clostridium perfringens.jpg|thumb|right|200px|Clostridium Perfingens. Source: Wikimedia Commons; Author:Don Stalons (1974)]] | ||
| + | In healthy animals, there is a balance between multiplication of ''Clostridium perfringens'' and its passage in the faeces. This ensures that infection is maintained at a low level. However, ''C. perfringens'' is saccharolytic and is therefore able to multiply rapidly when large quantities of fermentable carbohydrate are introduced to the anaerobic conditions of the abomasum and small intestine, leading to build-up of exotoxin. Gut stasis, for example due to insufficient dietray fibre or a high gastrointestinal parasite burden, can also contribute to the accumulation of toxins. | ||
| − | + | Enterotoxaemia due to ''Clostridium perfringens'' type B causes severe enteritis and dysentery with a high mortality in young lambs (lamb dysentery), but also affects calves, pigs, and foals. The β toxin it produces is highly necrotising and is responsible for severe intestinal damage. ε toxin also plays a part in pathogenesis. The incidence of lamb dysentery declined over the past 20 years or so, due to the widespread use of clostridial vaccines<sup>3</sup>, but the condition is now becoming a problem again as complacency reduces the use of vaccination. Outbreaks of lamb dysentery typically occur during cold, wet lambing periods when lambing ewes are confined to small areas of shelter which rapidly become unhygienic. Most cases are seen in stronger, single lambs<sup>3</sup> because these animals consume the largest quantities of milk, which functions as a growth medium for ''C. perfringens''. | |
| − | |||
| − | |||
| − | |||
| − | Enterotoxaemia due to ''Clostridium perfringens'' type B causes severe enteritis and dysentery with a high mortality in young lambs (lamb dysentery), but also affects calves, pigs, and foals. The β toxin it produces is highly necrotising and is responsible for severe intestinal damage. ε toxin also plays a part in pathogenesis. The incidence of lamb dysentery declined over the past 20 years or so, due to the widespread use of clostridial vaccines<sup>3</sup>, but the condition is now becoming a problem again as complacency reduces the use of vaccination. Outbreaks of lamb dysentery typically occur during cold, | ||
==Signalment== | ==Signalment== | ||
| − | |||
Affected animals are unvaccinated lambs of less than two to three weeks old. The condition is most common in neonates between one and three days of age, and typically affects well-fed singletons<sup>3</sup>. | Affected animals are unvaccinated lambs of less than two to three weeks old. The condition is most common in neonates between one and three days of age, and typically affects well-fed singletons<sup>3</sup>. | ||
==Diagnosis== | ==Diagnosis== | ||
| − | |||
A provisional diagnosis of lamb dysentery can be made on the basis of a history of sudden deaths in well-grown, unvaccinated lambs. This is supported by post-mortem findings and laboratory testing may also be useful. | A provisional diagnosis of lamb dysentery can be made on the basis of a history of sudden deaths in well-grown, unvaccinated lambs. This is supported by post-mortem findings and laboratory testing may also be useful. | ||
| − | === | + | ===Clinical Signs=== |
| − | |||
Lamb dysentery often presents as sudden death of lambs less than 2-3 weeks old<sup>2, 3, 4, 5</sup>. When clinical signs are seen, these include cessation of suckling, depression and recumbency<sup>4</sup>. Animals suffer acute abdominal pain, and semi-fluid blood-stained faeces may be passed<sup>2, 3, 4, 5</sup>. However, the rapid course of disease means that faeces are often observed to be normal. In 2-3 week old lambs, lamb dysentery may present with non-specific neurological signs<sup>3</sup>. | Lamb dysentery often presents as sudden death of lambs less than 2-3 weeks old<sup>2, 3, 4, 5</sup>. When clinical signs are seen, these include cessation of suckling, depression and recumbency<sup>4</sup>. Animals suffer acute abdominal pain, and semi-fluid blood-stained faeces may be passed<sup>2, 3, 4, 5</sup>. However, the rapid course of disease means that faeces are often observed to be normal. In 2-3 week old lambs, lamb dysentery may present with non-specific neurological signs<sup>3</sup>. | ||
===Laboratory Tests=== | ===Laboratory Tests=== | ||
| − | + | Intestinal contents or peritoneal fluid may be collected post-mortem and submitted for an [[ELISA testing|ELISA test]] to identify clostridial exotoxins. A positive result supports a diagnosis of enterotoxaemia but does not confirm it: animals with immunity to ''Clostridium perfringens'' may have high concentrations of toxin without suffering from its effects. | |
| − | Intestinal contents or | ||
Intestinal smears and scrapings readily reveal gram-positive rods<sup>3, 6</sup>. Culture of intestinal contents can yield almost pure growths of ''C. perfringens''<sup>6</sup>, but again this is supportive rather than diagnostic of lamb dysentery<sup>3</sup>. | Intestinal smears and scrapings readily reveal gram-positive rods<sup>3, 6</sup>. Culture of intestinal contents can yield almost pure growths of ''C. perfringens''<sup>6</sup>, but again this is supportive rather than diagnostic of lamb dysentery<sup>3</sup>. | ||
===Pathology=== | ===Pathology=== | ||
| + | On post-mortem examination, segments of the intestines appear dark red-purple and distended, and show mucosal ulceration<sup>3, 6</sup>. The peritoneal fluid is blood-stained and liver may be pale and friable. The kidneys are often enlarged<sup>3</sup>. | ||
| − | + | Histologically, numerous gram-positive rods are present in intestinal smears and scrapings<sup>3, 6</sup>. | |
| − | + | ==Treatment and Control== | |
| + | Presentation of lamb dysentery is usually peracute, with sudden deaths occurring before treatment can be implemented. Even if animals are found prior to death, treatment is usually unrewarding as organs are irreversibly damaged by toxins by the time signs present<sup>2</sup>. Instead, a definitive diagnosis should be pursued before greater losses occur, and the farmer should be encouraged to submit the carcase for further investigations. | ||
| + | |||
| + | As treatment is so ineffective, much emphasis is put on to the control of lamb dysentery. '''Vaccination''' in the face of an outbreak has been shown to be effective<sup>7</sup>, and specific hyperimmune serum can also be administered<sup>4, 6t</sup>. Oral antibiotics may be given<sup>4</sup> but are regarded as a less appropriate therepautic. Management measures such as removing the flock from a particular pasture or reducing concentrate feeding may be implemented in other clostridial diseases but are of no benefit in lamb dysentery: over-ingestion of the dam's milk combined with poor hygiene are responsible for this disease. Therefore, sufficient supervision should be given at lambing time to ensure adequate intakes of colostrum and the maintenance of good hygiene. | ||
| − | + | Lamb dysentery can be controlled through vaccination against clostridial diseases. Before the development of modern clostridial vaccines in the 1970s, catastrophic losses of up to 30% of the lamb crop could occur due to lamb dysentery<sup>2</sup>. The vaccines used today are effective against a variety of clostridial diseases and some vaccines are combined for effects against ''Pasteurella''. The vaccines consist of toxoids which are inactivated forms of the toxins produced by clostridial organisms. The principles of vaccination are the same whether a clostridium-only or ''Pasteurella''-combined product is used: a sensitising dose must be given 4-6 weeks before a second, confirming dose<sup>2</sup>. As immunity wanes over a period of a year booster doses are required annually. Therefore, ewes should receive the primary vaccination course before entering the breeding flock and an annual booster approximately six weeks before lambing. Timing the booster vaccination in this way affords passive protection to lambs until they are around sixteen weeks of age. Lambs born to unvaccinated ewes should be vaccinated between 3 and 12 weeks old, with a second injection given at least four weeks later. | |
| − | + | ==Literature Search== | |
| + | [[File:CABI logo.jpg|left|90px]] | ||
| − | |||
| − | |||
| − | + | Use these links to find recent scientific publications via CAB Abstracts (log in required unless accessing from a subscribing organisation). | |
| + | <br><br><br> | ||
| + | [http://www.cabdirect.org/search.html?q=title%3A%28%27%27Clostridium+perfringens%27%27+type+B+Enterotoxaemia%29+OR+title%3A%28%22lamb+dysentery%22%29 Lamb dysentery publications] | ||
==Links== | ==Links== | ||
| Line 62: | Line 61: | ||
#Lewis, C (2000) Vaccination of sheep: an update. ''In Practice'', '''22(1)''', 34-39. | #Lewis, C (2000) Vaccination of sheep: an update. ''In Practice'', '''22(1)''', 34-39. | ||
| − | [[Category:Enteritis,_Bacterial]][[Category:Enteritis,_Fibrinous/Haemorrhagic]] [[Category: | + | |
| − | [[Category: | + | {{review}} |
| + | [[Category:Enteritis,_Bacterial]][[Category:Enteritis,_Fibrinous/Haemorrhagic]] [[Category:Intestinal Diseases - Sheep]] | ||
| + | [[Category:Brian Aldridge reviewing]] | ||
Latest revision as of 17:57, 10 May 2011
Also known as: Clostridium perfringens type B Enterotoxaemia
Introduction
Lamb dysentery is a peracute and fatal enterotoxaemia of young lambs caused by the beta and epsilon toxins of Clostridium perfringens type B. C. perfringens is a large, gram positive, anaerobic bacillus that is ubiquitous in the environment and commensalises the gastrointestinal tract of most mammals1. Five genotypes of Clostridium perfringens exist, named A-E, and all genotypes produce potent exotoxins. There are 12 exotoxins in total, some of which are lethal and others which are of minor significance2. These are produced as pro-toxins, and are converted to their toxic forms by digestive enzymes. The enterotoxaemias are a group of diseases caused by proliferation of C. perfringens in the lumen of the gastrointestinal tract and excessive production of exotoxin.
In healthy animals, there is a balance between multiplication of Clostridium perfringens and its passage in the faeces. This ensures that infection is maintained at a low level. However, C. perfringens is saccharolytic and is therefore able to multiply rapidly when large quantities of fermentable carbohydrate are introduced to the anaerobic conditions of the abomasum and small intestine, leading to build-up of exotoxin. Gut stasis, for example due to insufficient dietray fibre or a high gastrointestinal parasite burden, can also contribute to the accumulation of toxins.
Enterotoxaemia due to Clostridium perfringens type B causes severe enteritis and dysentery with a high mortality in young lambs (lamb dysentery), but also affects calves, pigs, and foals. The β toxin it produces is highly necrotising and is responsible for severe intestinal damage. ε toxin also plays a part in pathogenesis. The incidence of lamb dysentery declined over the past 20 years or so, due to the widespread use of clostridial vaccines3, but the condition is now becoming a problem again as complacency reduces the use of vaccination. Outbreaks of lamb dysentery typically occur during cold, wet lambing periods when lambing ewes are confined to small areas of shelter which rapidly become unhygienic. Most cases are seen in stronger, single lambs3 because these animals consume the largest quantities of milk, which functions as a growth medium for C. perfringens.
Signalment
Affected animals are unvaccinated lambs of less than two to three weeks old. The condition is most common in neonates between one and three days of age, and typically affects well-fed singletons3.
Diagnosis
A provisional diagnosis of lamb dysentery can be made on the basis of a history of sudden deaths in well-grown, unvaccinated lambs. This is supported by post-mortem findings and laboratory testing may also be useful.
Clinical Signs
Lamb dysentery often presents as sudden death of lambs less than 2-3 weeks old2, 3, 4, 5. When clinical signs are seen, these include cessation of suckling, depression and recumbency4. Animals suffer acute abdominal pain, and semi-fluid blood-stained faeces may be passed2, 3, 4, 5. However, the rapid course of disease means that faeces are often observed to be normal. In 2-3 week old lambs, lamb dysentery may present with non-specific neurological signs3.
Laboratory Tests
Intestinal contents or peritoneal fluid may be collected post-mortem and submitted for an ELISA test to identify clostridial exotoxins. A positive result supports a diagnosis of enterotoxaemia but does not confirm it: animals with immunity to Clostridium perfringens may have high concentrations of toxin without suffering from its effects.
Intestinal smears and scrapings readily reveal gram-positive rods3, 6. Culture of intestinal contents can yield almost pure growths of C. perfringens6, but again this is supportive rather than diagnostic of lamb dysentery3.
Pathology
On post-mortem examination, segments of the intestines appear dark red-purple and distended, and show mucosal ulceration3, 6. The peritoneal fluid is blood-stained and liver may be pale and friable. The kidneys are often enlarged3.
Histologically, numerous gram-positive rods are present in intestinal smears and scrapings3, 6.
Treatment and Control
Presentation of lamb dysentery is usually peracute, with sudden deaths occurring before treatment can be implemented. Even if animals are found prior to death, treatment is usually unrewarding as organs are irreversibly damaged by toxins by the time signs present2. Instead, a definitive diagnosis should be pursued before greater losses occur, and the farmer should be encouraged to submit the carcase for further investigations.
As treatment is so ineffective, much emphasis is put on to the control of lamb dysentery. Vaccination in the face of an outbreak has been shown to be effective7, and specific hyperimmune serum can also be administered4, 6t. Oral antibiotics may be given4 but are regarded as a less appropriate therepautic. Management measures such as removing the flock from a particular pasture or reducing concentrate feeding may be implemented in other clostridial diseases but are of no benefit in lamb dysentery: over-ingestion of the dam's milk combined with poor hygiene are responsible for this disease. Therefore, sufficient supervision should be given at lambing time to ensure adequate intakes of colostrum and the maintenance of good hygiene.
Lamb dysentery can be controlled through vaccination against clostridial diseases. Before the development of modern clostridial vaccines in the 1970s, catastrophic losses of up to 30% of the lamb crop could occur due to lamb dysentery2. The vaccines used today are effective against a variety of clostridial diseases and some vaccines are combined for effects against Pasteurella. The vaccines consist of toxoids which are inactivated forms of the toxins produced by clostridial organisms. The principles of vaccination are the same whether a clostridium-only or Pasteurella-combined product is used: a sensitising dose must be given 4-6 weeks before a second, confirming dose2. As immunity wanes over a period of a year booster doses are required annually. Therefore, ewes should receive the primary vaccination course before entering the breeding flock and an annual booster approximately six weeks before lambing. Timing the booster vaccination in this way affords passive protection to lambs until they are around sixteen weeks of age. Lambs born to unvaccinated ewes should be vaccinated between 3 and 12 weeks old, with a second injection given at least four weeks later.
Literature Search
Use these links to find recent scientific publications via CAB Abstracts (log in required unless accessing from a subscribing organisation).
Lamb dysentery publications
Links
- The Merck Veterinary Manual: Enterotoxemia Caused by Clostridium perfringens Types B and C
- The Center for Food Security and Public Health Animal Disease Factsheet: Epsilon toxin of Clostridium perfringens.
- NOAH: Vaccination of farm animals
- Clostridia.net - Clostridium perfringens
References
- Van Metre (2006) Clostridial Infections of the Ruminant GI Tract. Proceedings of the North American Veterinary Conference 2006.
- Lewis, C (1998) Aspects of clostridial disease in sheep. In Practice, 20(9), 494-499.
- Sargison, N (2004) Differential diagnosis of diarrhoea in lambs. In Practice, 26(1), 20-27.
- Merck & Co (2008) The Merck Veterinary Manual (Eighth Edition), Merial.
- Songer, J G (1998) Clostridial diseases of small ruminants. Veterinary Research, 29, 219-232.
- Watt, A (1980) Neonatal losses in lambs. In Practice, 2(2), 5-9.
- West, D M (1993) Vaccines as therapeutics. Proceedings of the Third International Sheep Veterinary Society Conference, 17, 111-115.
- The Center for Food Security and Public Health, Iowa State University (2004) Animal Disease Factsheet: Epsilon toxin of Clostridium perfringens.
- Lewis, C (2000) Vaccination of sheep: an update. In Practice, 22(1), 34-39.
| This article has been peer reviewed but is awaiting expert review. If you would like to help with this, please see more information about expert reviewing. |