Difference between revisions of "Tuberculosis - Cattle"
Jump to navigation
Jump to search
(Redirected page to Mycobacterium bovis) |
|||
| (37 intermediate revisions by 2 users not shown) | |||
| Line 1: | Line 1: | ||
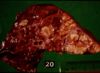
| − | # | + | [[Image:Tuberculosis M bovis.jpg|right|thumb|100px|<small><center>Tuberculosis caused by ''M. bovis'' (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] |
| + | |||
| + | *Caused by ''[[Mycobacterium bovis]]'' and ''M. tuberculosis'' | ||
| + | *Reside primarily within macrophages where they multiply and result in characteristic [[Lungs Inflammatory - Pathology#Granulomatous pneumonia|granulomatous inflammation]] (macrophages and giant cells, epithelioid cells) | ||
| + | *Cattle can be infected by inhalation of the organism or through milk | ||
| + | *'''The primary complex''' | ||
| + | **Describes the initial focus of infection at the portal of entry (lungs) plus involvement of regional lymph nodes | ||
| + | **90% of cases exhibit the pulmonary form | ||
| + | **Grossly: | ||
| + | ***Small tubercles in dorsocaudal subpleural areas which progress to larger confluent areas of caseous necrosis | ||
| + | ***Usually start at bronchio-alveolar junction an progress to the alveoli | ||
| + | ***Caseous lesions, may calcify or be encapsulated | ||
| + | ***Multiple foci may coalesce | ||
| + | ***Ulcers in [[Trachea Inflammatory - Pathology|trachea]] and [[Bronchi and Bronchioles Inflammatory - Pathology#Infectious causes of bronchitis or bronchiolitis|bronchi]] due to coughed up bacteria | ||
| + | ***Spreads into [[Pleural Cavity & Membranes Inflammatory - Pathology|pleura]] | ||
| + | **Microscopically: | ||
| + | ***Typical granulomatous inflammation | ||
| + | ***Epitheliod and giant cells at centre of tubercles | ||
| + | ****Macrophages with ingested bacteria, forming epithelioid cells - large vesicular nuclei, abundant pale cytoplasm | ||
| + | ****Giant cells, formed by fusion of macrophages, with multiple nuclei | ||
| + | ***Narrow layer of lymphocytes, mononuclear cells and plasma cells at the periphery of the tubercle | ||
| + | ***With time, peripheral fibroplasia and central necrosis develop | ||
| + | *If the infection is not contained in the primary complex described above, the mycobacteria can disseminate via lymphatics to other organs and lymph nodes | ||
| + | *This can allow the development of '''miliary tuberculosis''', i.e. numerous small foci of infection in many organs/ tissues | ||
| + | |||
| + | |||
| + | |||
| + | |||
| + | *inhalation of ''Mycobacterium bovis'' most common via droplets | ||
| + | *some tubercle bacilli enter the lymph and travel to the bronchial or mediastinal nodes | ||
| + | *inhaled bacilli reach the alveoli, set up a focus of inflammation | ||
| + | *phagocytosed by alveolar macrophages | ||
| + | *two processes may develop if the animal has not encountered the organism before: | ||
| + | :- the organism may grow in the phagocytes as intracellular parasites | ||
| + | ::- produces a nodule of parasitised swollen macrophages known as a tuburculous nodule or a tubercle granuloma | ||
| + | ::- ultimately, macrophages are killed and infection spreads | ||
| + | :- the organism may be broken down and some antigens taken up by the immune system | ||
| + | ::- cell mediated immune system produces cytotoxic T-lymphocytes | ||
| + | ::- T-lymphocytes can attack and destroy cells harbouring bacilli | ||
| + | ::- leads to type IV (delayedd type) hypesensitivity | ||
| + | ::- 'caseous' or cheesy type of necrosis | ||
| + | ::- if bacterium destroyed, further infection/disease is prevented | ||
| + | |||
| + | ====Sequelae==== | ||
| + | *chronicity | ||
| + | =====Tuberculosis pleurisy===== | ||
| + | *caseous lymph node ruptures | ||
| + | *results from extensive tissue necrosis | ||
| + | :- if located in lung alveoli, the follicle may rupture into a bronchus, causing spread of the disease to all the other lobules served by that bronchus | ||
| + | :- if the ensuing necrosis erodes the wall of a large pulmonary vessel, this ruptures into the lung and a fatal haemoptysis might follow | ||
| + | |||
| + | |||
| + | [[Category:Cattle]][[Category:To_Do_-_Clinical]] | ||
| + | [[Category:Respiratory_Bacterial_Infections]] | ||
Revision as of 11:00, 20 July 2010
- Caused by Mycobacterium bovis and M. tuberculosis
- Reside primarily within macrophages where they multiply and result in characteristic granulomatous inflammation (macrophages and giant cells, epithelioid cells)
- Cattle can be infected by inhalation of the organism or through milk
- The primary complex
- Describes the initial focus of infection at the portal of entry (lungs) plus involvement of regional lymph nodes
- 90% of cases exhibit the pulmonary form
- Grossly:
- Small tubercles in dorsocaudal subpleural areas which progress to larger confluent areas of caseous necrosis
- Usually start at bronchio-alveolar junction an progress to the alveoli
- Caseous lesions, may calcify or be encapsulated
- Multiple foci may coalesce
- Ulcers in trachea and bronchi due to coughed up bacteria
- Spreads into pleura
- Microscopically:
- Typical granulomatous inflammation
- Epitheliod and giant cells at centre of tubercles
- Macrophages with ingested bacteria, forming epithelioid cells - large vesicular nuclei, abundant pale cytoplasm
- Giant cells, formed by fusion of macrophages, with multiple nuclei
- Narrow layer of lymphocytes, mononuclear cells and plasma cells at the periphery of the tubercle
- With time, peripheral fibroplasia and central necrosis develop
- If the infection is not contained in the primary complex described above, the mycobacteria can disseminate via lymphatics to other organs and lymph nodes
- This can allow the development of miliary tuberculosis, i.e. numerous small foci of infection in many organs/ tissues
- inhalation of Mycobacterium bovis most common via droplets
- some tubercle bacilli enter the lymph and travel to the bronchial or mediastinal nodes
- inhaled bacilli reach the alveoli, set up a focus of inflammation
- phagocytosed by alveolar macrophages
- two processes may develop if the animal has not encountered the organism before:
- - the organism may grow in the phagocytes as intracellular parasites
- - produces a nodule of parasitised swollen macrophages known as a tuburculous nodule or a tubercle granuloma
- - ultimately, macrophages are killed and infection spreads
- - the organism may be broken down and some antigens taken up by the immune system
- - cell mediated immune system produces cytotoxic T-lymphocytes
- - T-lymphocytes can attack and destroy cells harbouring bacilli
- - leads to type IV (delayedd type) hypesensitivity
- - 'caseous' or cheesy type of necrosis
- - if bacterium destroyed, further infection/disease is prevented
Sequelae
- chronicity
Tuberculosis pleurisy
- caseous lymph node ruptures
- results from extensive tissue necrosis
- - if located in lung alveoli, the follicle may rupture into a bronchus, causing spread of the disease to all the other lobules served by that bronchus
- - if the ensuing necrosis erodes the wall of a large pulmonary vessel, this ruptures into the lung and a fatal haemoptysis might follow