| This article has been peer reviewed but is awaiting expert review. If you would like to help with this, please see more information about expert reviewing. |
|
|
Hyperaemia
- Localised of diffuse as part of acute inflammation
Congestion
- Decreased outflow of venous blood
- Most commonly caused by left-sided or bilateral cardiac failure
- Stagnant blood in pulmonary vessels -> red blood cells move into alveoli and are phagocytosed -> haemosiderin in macrophages (heart failure cells)
- One-sided in post-mortem hypostatic congestion
- Acute pulmonary congestion is seen after barbiturate euthanasia
- Leads to pulmonary oedema (below)
Pulmonary oedema
- Excessive fluid in the lung
- Normally, mechanisms are in place to protect the lung from the entry of circulatory fluid into alveolar spaces (See functional anatomy)
- Occurs when exudation of fluid from vessels into interstitium or alveoli exceeds the rate of alveolar or lymph removal
- Generally a sequel to or part of congestion or inflammatory process
- Generally begins as interstitial oedema characterised by expansion of perivascular and peribronchial and peribronchiolar fascia and distension of interstitial lymphatics
- Only when this interstitial compartment is overwhelmed does fluid flood the airspaces causing alveolar oedema
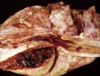
- Gross pathology:
- Heavy wet lungs which do not properly collapse
- Subpleural and interstitial tissue distended with fluid
- Foamy fluid oozing from the cut surface and airways
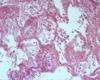
- Micro pathology:
- Pinkish fluid in alveoli and airways in association with air bubbles, and also in dilated lymphatics of the interstitium
- Colour of the fluid enhanced in cases where the endothelium is damaged - more protein present
- In slowly developing cases, macrophages contain haemosiderin
- The major causes of pulmonary oedema are:
- Increased capillary or type I epithelial permeability caused by
- Systemic toxins
- Shock
- Inhaled caustic gases
- Increased capillary hydrostatic pressure (cardiogenic oedema - left-sided or biventricular heart failure, sympathetic stimulation in acute brain damage)
- Decreased plasma oncotic pressure (hypoalbuminaemia)
- Overloading in excessive fluid therapy
- As part of inflammatory process
- Increased capillary or type I epithelial permeability caused by
Pulmonary haemorrhage
- Potential sequel of septicaemias, bleeding disorders, disseminated intravascular coagulation, and severe congestion, severe acute inflammation, "back splashing" at slaughter (aspiration of blood)
- Exercise-induced pulmonary hemorrhage (EIPH)
Embolism, thrombosis and infarction
- Lungs are strategically situated to catch emboli carried in venous blood
- Because the lung is supplied by both pulmonary and bronchial arteries and has extensive collateral channels, infarction usually does not follow embolism or thrombosis unless pulmonary circulation is already compromised
- In animals, greatest risk comes from:
- Tumor emboli
- From e.g.: osteosarcoma and haemangiosarcoma in dogs, uterine carcinoma in cattle
- Septic emboli
- From bacterial endocarditis, jugular thrombophlebitis, hepatic abscesses etc.
- May cause unexpected death if in large numbers
- May develop suppurative pneumonia -> pulmonary abscesses, arteritis, thrombosis
- Tumor emboli
- Pulmonary infarcts usually occur when there is embolisation or thrombosis during general circulatory collapse or passive congestion of heart failure
- Pulmonary thromboembolism is a sequel to in cattle to large emboli from liver abscesses close to the vena cava
- Death may ocur due to massive haemorrhaging into lung tissue
- Parasites (e.g. Dirofilaria immitis, Angiostrongylus vasorum) may be responsible
- Long-term intravenous catheterisation may cuse thrombi pieces breaking off and lodging in pulmonary vessels
Pulmonary hypertension
- Caused by left-to-right vascular shunts or increased resistance of the pulmonary vascular system
- In animals, it is most commonly a sequel of widespread fibrosis in the lung or chronic bronchitis or bronchiolitis which stimulates hypertrophy in the walls of small arteries
- Severe prolonged pulmonary hypertension leads to cor pulmonale, right-sided heart failure secondary to primary lung disease