Difference between revisions of "Coagulation Tests"
| Line 22: | Line 22: | ||
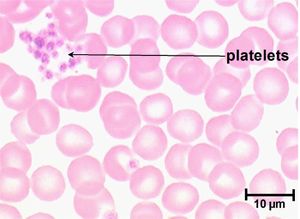
A platelet count can give valuable information in all critically ill animals and is an essential laboratory test for patients where there are concerns about abnormal bleeding. Platelet numbers may be rapidly estimated by examination of a stained blood smear, or quantified by manual or automated counting techniques. [[Platelet_Abnormalities#Artefactual_or_spurious_thrombocytopaenia|Platelet clumping]] can give an artificially low platelet count when using manual or automated counting methods. To estimate the platlet number using a blood smear, the slide should first be scanned for evidence of clumping that would artificially reduce the count. The average number of platelets in ten oil-immersion fields should be counted, and a mean calculated. Each platelet in a high-power field represents 15,000 platelets per microlitre<sup>2</sup>. A "normal" platelet count therefore gives around 10-15 platelets per oil-immersion field. | A platelet count can give valuable information in all critically ill animals and is an essential laboratory test for patients where there are concerns about abnormal bleeding. Platelet numbers may be rapidly estimated by examination of a stained blood smear, or quantified by manual or automated counting techniques. [[Platelet_Abnormalities#Artefactual_or_spurious_thrombocytopaenia|Platelet clumping]] can give an artificially low platelet count when using manual or automated counting methods. To estimate the platlet number using a blood smear, the slide should first be scanned for evidence of clumping that would artificially reduce the count. The average number of platelets in ten oil-immersion fields should be counted, and a mean calculated. Each platelet in a high-power field represents 15,000 platelets per microlitre<sup>2</sup>. A "normal" platelet count therefore gives around 10-15 platelets per oil-immersion field. | ||
| − | The reference range given for platelet number is usually around 200-500x10<sup>9</sup> per litre, although this varies depending on the laboratory equipment used. Clinical signs due to thrombocytopenia are not commonly encountered until the platelet count drops below 50x10<sup>9</sup>/l, when increased bleeding times may be seen. Haemorrhage during surgery becomes a concern with counts lower than 20x10<sup>9</sup>/l, and spontaneous bleeding arises when platelets are fewer than 5x10<sup>9</sup>/l<sup>2</sup>. These cut-offs are lowered if platelet function is concurrently affected | + | The reference range given for platelet number is usually around 200-500x10<sup>9</sup> per litre, although this varies depending on the laboratory equipment used. Clinical signs due to thrombocytopenia are not commonly encountered until the platelet count drops below 50x10<sup>9</sup>/l, when increased bleeding times may be seen. Haemorrhage during surgery becomes a concern with counts lower than 20x10<sup>9</sup>/l, and spontaneous bleeding arises when platelets are fewer than 5x10<sup>9</sup>/l<sup>2</sup>. These cut-offs are lowered if platelet function is concurrently affected by other factors such as the use of non-steroidal anti-inflammatory drugs<sup>1</sup>. |
===Buccal Mucosal Bleeding Time=== | ===Buccal Mucosal Bleeding Time=== | ||
Revision as of 16:17, 8 October 2010
Also known as: coagulation profile — clotting profile — clotting tests — tests of haemostasis
Introduction
Normally, haemostastis is maintained by three key events:
- Primary haemostasis involves platelets and the blood vessels themselves and is triggered by injury to a vessel - platelets become activated, adhere to endothelial connective tissue and aggregate with other platelets. A fragile plug is formed which helps to stem haemorrhage from the vessel. Substances released from platelets during primary haemostasis include vasoactive compounds to induce vasoconstriction and other mediators that cause continued platelet activation and aggregation, as well as contraction of the platelet plug. Primary haemostasis ceases once defects in the vessels are sealed and bleeding stops.
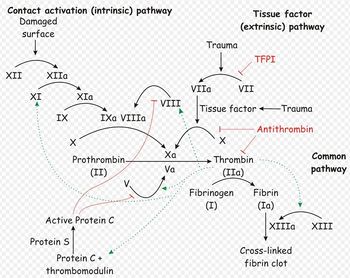
- Secondary haemostasis occurs when proteinaceous clotting factors interact in a cascade to produce fibrin to reinforce the clot. Two arms of the cascade are activated simultaneously to achieve coagulation: the intrinsic and extrinsic pathways. The intrinsic pathway is activated by contact with collagen due to vessel injury and involves the clotting factors XII, XI, IX and VIII. The extrinsic pathway is triggered by tissue injury and is effected via factor VII. These pathways progress independently before converging at the common pathway, which involves the factors X, V, II and I and ultimately results in the formation of fibrin from fibrinogen. Factors II, VII, IX and X are dependent upon vitamin K to become active.
- Fibrinolysis is the final stage of restoring haemostasis - it prevents uncontrolled, widespread clot formation and breaks down the fibrin within blood clots. The two most important anticoagulants involved in fibrinolysis are antithrombin III (ATIII) and Protein C. The end products of fibinolysis are fibrin degratation products (FDPs).
Abnormalities can develop in any of the components of haemostasis. Disorders of primary haemostasis include vessel defects (i.e. vasculitis), thrombocytopenia (due to decreased production or increased destruction) and abnormalities in platelet function (e.g. congenital defects). These lead to the occurence of multiple minor bleeds and prolonged bleeding times; petechial or ecchymotic haemorrhages may be seen for example, on the skin and mucous membranes, or ocular bleeds may arise. Generally, intact secondary haemostasis prevents major haemorrhage in disorders of primary haemostasis. When secondary haemostasis is abnormal, larger bleeds are frequently seen. Haemothorax, haemoperitoneum, or haemoarthrosis may occur, in addition to subcutaneous and intramuscular haemorrhages. Petechiae and ecchymoses are not usually apparent, as intact primary haemostasis prevents minor capillary bleeding. Examples of secondary haemostatic disorders include clotting factor deficiencies (e.g. hepatic failure, vitamin K deficiency, hereditary disorders) and circulation of substances inhibitory to coagulation (FDPs in disseminated intravascular coagulation, lupus anticoagulant). If fibrinolysis is defective, thrombus formation and infarctions may result. Thrombus formation may be promoted by vascular damage, circulatory stasis or changes in anticoagulants or procoagulants. For example, ATIII may be decreased. This can occur by loss due to glomerular disease or accelerated consumption in disseminated intravascular coagulation or sepsis.
It is therefore important that all aspects of haemostasis can be independantly evaluated. This will help to identify the phase affected and to pinpoint what the abnormality is. There are tests available to assess primary haemostasis, secondary haemostasis and fibrinolysis.
Tests Evaluating Primary Haemostasis
Primary haemostasis is dependent on the activity of platelets and, to a lesser extent, the blood vessels themselves. Platelets are the smallest solid formed component of blood, and are non-nucleated, flattened disc-shaped structures1. Their activity leads to vascoconstriction and the formation of platelet plugs to occlude vessel defects. Platelets develop in the bone marrow, and have a life span of around 7.5 days. Around two thirds of platelets are found in the circulation at any one time, with the remainder residing in the spleen1.
Apart from unusual cases involving vasculitis, there are two causes of defects in primary haemostasis: thrombocytopenia (reduced platelet number), or thrombocytopathia (defective platelet function)2.
Platelet Number
A platelet count can give valuable information in all critically ill animals and is an essential laboratory test for patients where there are concerns about abnormal bleeding. Platelet numbers may be rapidly estimated by examination of a stained blood smear, or quantified by manual or automated counting techniques. Platelet clumping can give an artificially low platelet count when using manual or automated counting methods. To estimate the platlet number using a blood smear, the slide should first be scanned for evidence of clumping that would artificially reduce the count. The average number of platelets in ten oil-immersion fields should be counted, and a mean calculated. Each platelet in a high-power field represents 15,000 platelets per microlitre2. A "normal" platelet count therefore gives around 10-15 platelets per oil-immersion field.
The reference range given for platelet number is usually around 200-500x109 per litre, although this varies depending on the laboratory equipment used. Clinical signs due to thrombocytopenia are not commonly encountered until the platelet count drops below 50x109/l, when increased bleeding times may be seen. Haemorrhage during surgery becomes a concern with counts lower than 20x109/l, and spontaneous bleeding arises when platelets are fewer than 5x109/l2. These cut-offs are lowered if platelet function is concurrently affected by other factors such as the use of non-steroidal anti-inflammatory drugs1.
Buccal Mucosal Bleeding Time
The buccal mucosal bleeding time is a simple test that gives a rapid assessment of platelet function, providing platelet numbers are normal. If platelet numbers are below 50x109/l, this test should not be performed since the results will be affected by thrombocytopenia, making them unreliable. The small wound inflicted may also not stop bleeding easily.
To perform the BMBT test, a standardised tool producing a uniform incision is used2, 3 to incise the buccal mucosa of the upper lip, and the time between making the incision and the cessation of bleeding is measured2. During the procedure the lip should be kept turned outwards, with excess blood being gently absorbed at a site away from the incision, without disturbing clot formation or applying pressure. Normally, bleeding should stop within 3 minutes, and a BMBT of greater than 5 minutes is considered prolonged2.
Acquired platelet function abnormalities are often drug induced, for example by non-steroidal anti-inflammatory drugs2, 3, or caused by uraemia. Hereditary defects in platelet function also exist, and von Willebrand's disease is the most common of these.
The BMBT is influenced by all the aspects of this phase, including vasoconstriction, platelet adherence and plately aggregation. Although this makes BMBT an effective screening test for the vascular/platelet (primary) phase of haemostasis, it also means it is not purely a test for thrombocytopathia, as it is often considered: BMBT depends on an intact vasospastic response and adequate platelet numbers as well as platelet function3. BMBT is a fairly crude test, and has been found to be normal in some patients with a known platelet function disorder and vice versa3. Therefore, the results of this test should be interpreted with some caution.
Tests Evaluating Secondary Haemostasis
Secondary haemostasis describes the formation of a cross linked fibrin meshwork in the blood clot and is dependent on soluble coagulation factors. Abnormalities in secondary coagulation can occur from insufficient coagulation factors, the presence of inactive coagulation factors or inhibition of factors. The soluble coagulation factors are traditionally divided into the intrinsic, extrinsic and common pathways, as described in the introduction.
Activated Clotting Time
The activated clotting time (ACT) allows rapid evaluation of secondary haemostasis. The ACT is the time taken for 2ml of fresh whole blood to clot in a tube with a contact activator (diatomaceous earth2), but an automated analyser can perform a test with a similar principle. The reaction must occur at body temperature to give a reliable indication of haemostatic ability: this can be achieved by the use of a warm water bath, or by holding the tubes under an arm. The normal ACT is 90-120 seconds and less than 75 seconds in dogs and cats respectively2.
The contact activator used in the ACT test triggers the intrinsic pathway, and so ACT allows assessment of the intrinsic and common pathways. ACT will therefore be prolonged when factors I, II, V, VIII, IX, X, XI or XII are deficient or abnormal, such as in DIC, liver disease, vitamin K antagonist toxicosis or haemophilia A or B2. Thrombocytopenia may also increase ACT.
Activated Partial Thromboplastin Time
The APTT is measures the time necessary to generate fibrin from activation of the intrinsic pathway3. It therefore assesses functionality of the components of the intrinsic and common pathways of coagulation. The test is performed on citrated plasma, and so blood should be collected into a sodium citrate tube if the APTT test is to be undertaken. Once a sample is obtained, factor XII is activated by an external agent that will not also activate factor VII, such as kaolin1, 3. Since the intrinsic arm of the cascade requires platelet factors to function, the test also provides a phospholipid emuslion in place of these factors. Calcium is added, the preparation is incubated, and the time for clumping of kaolin is measured. Classically, partial thromboplastin time was measured after activation by contact with a glass tube, but use of an external activating agent in the newer, "activated" partial thromboplastin time method makes results more reliable3.
APPT evaluates the same pathways as ACT, and so will be prolonged by abnormalities or deficiencies in factors XII, XI, IX, VIII, X, V, II or I. However, APTT is not affected by thrombocytopenia and is also considered to be a more sensitive test than ACT: APTT becomes prolonged when 70% of a factor is depleted, compared to 90% depletion of ACT. APTT can also be prolonged in the presence of a circulating inhibitor to any of the intrinsic pathway factors. To differentiate factor deficiency from inhibition, a "mixing study" can be performed where the test is repeated on a 1:1 mix of patient and normal plasma. Complete correction indicates a deficiency, and partial or no resolution shows that an inhibitor is present. This difference stems from the above mentioned fact that the APTT will be normal in the presence of 50% normal activity3.
Conditions in which APTT is prolonged include inherited disorders, such as haemophilia A and B and other congential absences of intrinsic and common factors. Acquired factor deficiency also occurs, for example with vitamin K deficiency, liver dysfunction, prolonged bleeding or disseminated intravascular coagulation. The most common inhibitors found to prolong APTT are the antithrombins, which inhibit the activity of thrombin on the conversion of fibrinogen to fibrin. Examples include heparin and fibrin degradation products.
Occasionally, a shortened APTT is seen. This may reflect increased levels of activated factors in a hypercoagulable state, for example in the early stages of DIC3.
Prothrombin Time
Prothrombin time (PT) gives an assessment of the extrinsic and common pathways by measuring the time necessary to generate fibrin after activation of factor VII3. It is performed by an automated analyser2 using citrated plasma1, 3. Blood should therefore be collected into a sodium citrate tube if prothrombin time is to be performed. In basic terms, the test procedure involves adding thromoplastin to the patient's plasma, warming, adding calcium and recording the time taken to clot1.
A prolonged PT may reflect a factor deficiency or the presence of a circulating inhibitor of coagulation. Repeating the test using a mix of test plasma and "normal" plasma can help differentiate these possibilities: PT returns to normal limits when normal plasma is added to factor-deficient plasma, but no change is seen when this is added to plasma containing inibitors3. PT is more sensitive than APTT for factor deficiencies.
PT is affected by abnormalities or deficiencies in coagulation factors I, II, VII or X, for example in DIC, liver disease, or poisoning with vitamin K antagonists. Inherited defects are possible. PT is also prolonged by the presence of circulating anticoagulants. Inhibitors are often directed at factor X or thrombin and can include fibrin degradation products or heparin3.
Tests for Individual Clotting Factors
Some specialised laboratories offer tests for specific clotting factors. Blood is required to be collected into a sodium citrate tube.
Proteins Induced by Vitamin K Antagonism Test
Factors II, VII, IX and X are produced in the liver as non-functional precursors which become activated by carboxylation of their glutamic acid residues in the presence of vitamin K. The inactive precursors are absent from the circulation of normal animals, as they are stored in the microsomal system of the liver. However, the absence of vitamin K results in an increase in these precursors, which spill into the circulation and become known as Proteins Induced by Vitamin K Antagonism (PIVKA). Concurrently, the levels of active factors II, VII, IX and X are depleted.
The PIVKA test is modified version of PT that is designed to be more sensitive than PT for abnormalities in the vitamin-K dependent clotting factors. Diluted plasma is used to give longer clotting times, and a test-specific reagent is added. The PIVKA test is reported to be sensitive to both increases in PIVKAs and decreases in the functional coagulation factors II, VII, IX and X, although there is some debate as to whether PIVKAs actually inhibit the reaction. Although intended to be more sensitive than the PT for factors of interest, studies in dogs have shown that a PIVKA test offers little diagnostic advantage4. Additionally, only certain laboratories offer the test and the turnaround time is longer than PT.
The PIVKA test is prolonged in vitamin K deficiency. This can result from anticoagulant rodenticide toxicity or cholestasis. Some animals in disseminated intravascular coagulation also have a prolonged PIVKA test.
Tests Evaluating Fibrinolysis
Fibrin Degradation Products
A latex agglutination test is available for fibrin degradation products (FDP). To perform the test, anti-FDP antibodies attached to latex particles are added to serial dilutions of test serum. If agglutination is seen at a particular dilution, the test is positive. The most dilute sample that agglutinates gives the overall result of the test. Normal values are between 1/4 and 1/16.
Although the test is simple to perform, interpretation may be challenging. This is because other small fragments involved in the homeostasis of fibrinogen and fibrin are measured by the test in addition to bona fide fibrin degradation products. In general, an increase in FDP correspons to increased fibrinolysis. This can be due to a local problem of fibrin generation such as thrombosis, trauma or chronic bleeding, or be related to a systemic process, usually DIC3.
Literature Search
Use these links to find recent scientific publications via CAB Abstracts (log in required unless accessing from a subscribing organisation).
Coagulation Tests publications
Links
References
- Fischbach, F T and Dunning, M B (2008) A manual of laboratory and diagnostic tests, Lippincott Williams and Wilkins.
- Hopper, K (2005) Interpreting coagulation tests. Proceedings of the 56th conference of La Società culturale italiana veterinari per animali da compagnia.
- Walker, K H et al (1990) Clinical Methods: The History, Physical and Laboratory Examinations (Third Edition), Butterworths.
- Cornell University Clinical Pathology Modules: Tests of Haemostasis - PIVKA
- Howard, M R and (2008) Haematology: an illustrated colour text, Elsevier Health Sciences.