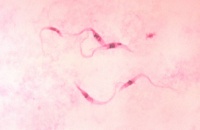
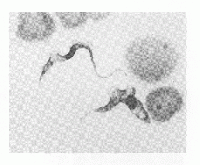
Trypanosomosis
Also Known As: Nagana — Trypanosomiasis — Chagas' Disease — Sleeping Sickness — Parrot Sickness — Dourine
Introduction
Trypanosomosis is a disease caused by protozoan pathogens of the genus Trypanosoma. They are obligate parasites and can infect mammals, birds, reptiles, amphibians and fish.
Trypanosomes are divided into two categories depending upon their lifecycle: Stercorarian trypanosomes develop within an insect vector and are transmitted to mammals in the faeces of the vector.
Salivarian trypanosomes develop within tsetse flies and mammals are infected through their bites.
For more information about the various species see Trypanosoma page.
Trypanosomosis causes a wasting disease in cattle and sleeping sickness in humans.
T. cruzi is the cause of Chagas disease in humans but can also affect dogs, cats and pigs. T. vivax and T. congolense are the main pathogens of cattle. In horses, T. equiperdum is the cause of Dourine.
Trypanosomosis is notifiable to the World Organisation for Animal Health (OIE).
Signalment
Some breeds appear trypanotolerant and able to resist clinical disease and anaemia, such as African buffalo and N’dama and Keteku cattle.
Calves less than a year old are more resistant than adults, but lambs and kids appear more susceptible to T. congolense infections. Cattle 6-9yrs old appear most susceptible to trypanosomosis.
Transmission
Trypanosomosis is spread by Tsetse flies and other insect vectors.
Horse flies and stable flies can also act as mechanical vectors for some trypanosoma species, but the parasites cannot undergo lifecycle development within these hosts.
T. vivax and T. evansi are reported to achieve transplacental transmission. [1]
Distribution
Worldwide
T. brucei, T. uniforme, T. congolense and T. simiae are found only in the tsetse fly belt of Africa due to the restricted spread of their vector. T. vivax is more widespread occurring in Sub-saharan Africa as well as South America.
Clinical Signs
Clinical disease varies widely with death occurring from 1 week to months after infection. T. vivax is known for its rapid mortality while T. brucei and T. congolense hosts often survive for prolonged periods. Infection of large numbers of insect vectors is common in these circumstances.
Significant losses may also be caused by increased susceptibility and prevalence of other concurrent diseases where trypanosomosis is present.
Multisystemic signs can be seen in any species so diagnosis from clinical examination is often impossible as no pathognomonic signs are evident.
Ruminants
Enlarged lymph nodes and spleen are the most common sign. Later in the disease course the lymph nodes and spleen shrink due to lymphoid exhaustion.
Haemolytic anaemia is a cardinal feature. Chronic infection causes heart failure and associated signs and death.
Plasma cell hypertrophy and hypergammaglobulinaemia are evident on haematology and biochemistry.
Emaciation, abortion, premature births and infertility are features, and orchitis in males reduces fertility.
Horses
Oedema of the limbs and genitalia is very common.
Dourine – genital and abdominal oedema, paraphimosis, urticarial plaques known as “silver dollar spots” and neurological signs may all be present. The disease is usually mild and recurrent but can be fatal.
Donkeys
See donkey skin infections page for details.
Dogs and Cats
Pyrexia, myocarditis, myositis, corneal opacity and occasionally neurological signs may all be present.
Diagnosis
Microscopic identification on trypanosome parasites in the host blood on a smear with Giemsa staining is commonly performed. Where low levels of parasitaemia are present, filtration or haemolysis of a whole blood sample may be required and motile trypanosomes may be demonstrable in a haematocrit tube at the plasma: buffy coat interface.
On post-mortem examination, carcasses are often pale and oedematous due to anaemia and emaciation. Degenerative lesions can be found on the heart, liver, lymph nodes, testes, brain, conjunctiva, cornea, spleen, kidney and endocrine organs.
Many other seroimmunological techniques are also available variably in laboratories.
Treatment
A variety of drugs can be used to treat trypanosomosis including diminazene, homidium, isometadium, suramin and melarsomine.
Diminazene aceturate is most commonly used and is frequently curative. It however causes frequent local reactions in horses so should be given in multiple deep muscular sites and massaged well. The drug is also contraindicated in dogs and camels due to vascular damage. Diminazene also has a prophylactic effect for up to 3 months.
Resistance is increasing in Africa to trypanosomicidal drugs so multiple treatments may be required in some areas.
Control
Separation of livestock and wild animals is effective but difficult.
Use of trypanotolerant livestock breeds is the only option is some areas where economic restraints prevent constant treatment and control.
Tsetse fly control by sprays, traps, dips and release of sterile male flies is effective but expensive and time-consuming.
Prophylactic drug therapy is also effective but costly.
| Trypanosomosis Learning Resources | |
|---|---|
 Test your knowledge using flashcard type questions |
Trypanosomosis Flashcards |
References
- ↑ Ikede, B. O., Loso, G. J.(1972). Hereditary transmission of Trypanosoma vivax. Brit Vet J, 128:i-ii
Merck Veterinary Manual, Tsetse-transmitted Trypanosomiasis accessed online 03/06/2011 @ http://www.merckvetmanual.com/mvm/index.jsp?cfile=htm/bc/10413.htm

|
This article was originally sourced from The Animal Health & Production Compendium (AHPC) published online by CABI during the OVAL Project. The datasheet was accessed on 5 June 2011. |
| This article has been expert reviewed by Nick Lyons MA VetMB CertCHP MRCVS Date reviewed: 15 October 2011 |
Error in widget FBRecommend: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69ad484ab6ca08_68881676 Error in widget google+: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69ad484ac3c5f4_51660951 Error in widget TwitterTweet: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69ad484aca3bf9_36357358
|
| WikiVet® Introduction - Help WikiVet - Report a Problem |