Difference between revisions of "Muscles Degenerative - Pathology"
Jump to navigation
Jump to search
(Redirected page to Category:Muscles - Degenerative Pathology) |
|||
| (32 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
| − | # | + | {{review}} |
| + | |||
| + | {{toplink | ||
| + | |backcolour =CDE472 | ||
| + | |linkpage =Musculoskeletal System - Pathology | ||
| + | |linktext =Musculoskeletal System | ||
| + | |maplink = Musculoskeletal System (Content Map) - Pathology | ||
| + | |pagetype =Pathology | ||
| + | |sublink1=Muscles - Pathology | ||
| + | |subtext1=MUSCLES | ||
| + | }} | ||
| + | <br> | ||
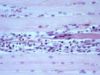
| + | ==Degeneration== | ||
| + | [[Image:Degenerate muscle fibres.jpg|right|thumb|100px|<small><center>Degenerate muscle fibres (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | ||
| + | |||
| + | *Different types of degeneration | ||
| + | *May, or may not, be reversible | ||
| + | *Cloudy swelling, hydropic, vacuolar, granular and fatty change | ||
| + | *Occur following many different types of insult and are usually '''segmental''' | ||
| + | *If regeneration does not occur after formation of small vacuoles, [[Muscles Degenerative - Pathology#Necrosis|necrosis]] follows | ||
| + | **Vacuolation -> floccular degeneration -> granular degeneration -> [[Degenerations and Infiltrations - Pathology#Hyaline Degeneration|hyaline]] and [[Zenker Degeneration - Pathology|Zenker’s degeneration]] | ||
| + | *[[Degenerations and Infiltrations - Pathology#Vacuolar Degeneration|'''Vacuolar degeneration''']]: | ||
| + | **Due to swelling of organelles or due to glycogen or fat accumulation | ||
| + | **May be caused by hypokalaemia, hyperkalaemia or necrosis | ||
| + | *Histologically: | ||
| + | **Swollen | ||
| + | **Hypereosinophilic | ||
| + | **Lost cross striations | ||
| + | |||
| + | |||
| + | ===Calcification=== | ||
| + | |||
| + | *Due to: | ||
| + | **Old age - myofibres | ||
| + | **Following necrosis - [[Pigmentation and Calcification - Pathology#Dystrophic|dystrophic calcification]] | ||
| + | ***May be visible grossly as white foci | ||
| + | |||
| + | |||
| + | ===Ossification=== | ||
| + | |||
| + | *Metaplasia of muscle to bone | ||
| + | *'''Localised''' | ||
| + | **Only in single muscle or a single group of muscles | ||
| + | **May be associated with trauma | ||
| + | **Seen in horses and dogs | ||
| + | **Histologically: | ||
| + | ***Central zone - proliferating undifferentiated cells and [[Chronic Inflammation - Pathology#Fibroblasts|fibroblasts]] | ||
| + | ***Middle zone - [[Bones - normal#Normal structure|osteoblasts]] depositing osteoid and bone | ||
| + | ***Outer zone - [[Bones - normal#Bone organisation|trabecular bone]] remodelled by [[Bones - normal#Normal structure|osteoclasts]] | ||
| + | *'''Progressive''' (fibrodysplasia ossificans progressiva) | ||
| + | **In connective tissue associated with skeletal muscle | ||
| + | **Secondary involvement of muscle tissue | ||
| + | **In pigs and cats | ||
| + | **Histologically: | ||
| + | ***Bundles of dense fibrous connective tissue | ||
| + | ***May contain accumulations of cartilage, bone or calcium | ||
| + | **Hyperplastic connective tissue -> compression of adjacent skeletal muscle -> [[Muscles Degenerative - Pathology#Atrophy|atrophy]] | ||
| + | |||
| + | |||
| + | ===Pigmentation=== | ||
| + | |||
| + | *[[Pigmentation and Calcification - Pathology#Lipofuscin|'''Lipofuscin''']] | ||
| + | **Wear and tear pigment accumulating in secondary lisosomes -> converted into compact residual bodies | ||
| + | **Due to old age, past or recent cachexia or starvation | ||
| + | **Mostly stored in skeletal muscle of old high producing dairy cattle | ||
| + | **Masseters and diaphragm mainly involved | ||
| + | **No clinical importance | ||
| + | **Histologically: | ||
| + | ***Rounded yellow to brown granules at both poles of nucleus of the skeletal myofiber | ||
| + | *[[Pigmentation and Calcification - Pathology#Melanin|'''Melanin''']] | ||
| + | **As part of congenital melanosis of calves in fascial sheaths and epimysium | ||
| + | **Grossly - black foci | ||
| + | *'''Myoglobin''' | ||
| + | **After extensive muscle necrosis - '''rhabdomyolysis''' | ||
| + | **Leaks to adjacent tissue after sudden injury | ||
| + | *May also be present after some types of intramuscular injections e.g. iron dextran or tetracycline | ||
| + | |||
| + | |||
| + | ==Necrosis== | ||
| + | |||
| + | *Necrosis of an entire myofibre is uncommon | ||
| + | *Segmental necrosis is more typical | ||
| + | *Muscle cell contents may leak into the blood if the cell membrane is damaged | ||
| + | *Creatine kinase (CK) is an enzyme which leaks following injury | ||
| + | **Used to measure the extent of muscle damage | ||
| + | *Often is followed by [[Muscle Regeneration - Anatomy & Physiology|regeneration]] | ||
| + | *Histologically: | ||
| + | **Hyaline hypercontracted fiber rounded at cross-section and increased diameter and eosin staining | ||
| + | ***May also be an artifact due to hypercontraction of normal fibres at fixation | ||
| + | **Fragmenting portions of fibre -> floccular or granular | ||
| + | **Normal portion of fibre may detach from necrotic part -> retraction caps | ||
| + | **Infarction may cause '''discoid degeneration''' - necrotic fibres detach at '''Z lines''' | ||
| + | **May [[Muscles Degenerative - Pathology#Calcification|mineralise]] | ||
| + | *[[Zenker Degeneration - Pathology|'''Zenker's degeneration''']] - secondary to systemic disease | ||
| + | **Scattered small segments of necrosis and fast regeneration | ||
| + | **Sacrolemmal tubes are intact | ||
| + | |||
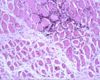
| + | ==Atrophy== | ||
| + | [[Image:Atrophic muscle fibres.jpg|right|thumb|100px|<small><center>Atrophic muscle fibres (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | ||
| + | |||
| + | *Decreased myofibre or whole muscle diameter | ||
| + | *Myofibrils removed by disintegration -> sacrolemma too large -> forms folds | ||
| + | *Caused by: | ||
| + | **<u>'''Disuse'''</u> (e.g. fracture, failure to use limb, recumbency) | ||
| + | ***Slower than denervation atrophy | ||
| + | ***Reversible unless too prolonger or severe to cause loss of myofibres | ||
| + | **<u>'''Denervation'''</u> | ||
| + | ***Any interference or damage to its nerve supply results in muscle atrophy | ||
| + | ****Can be rapid - over 50% of muscle mass may be lost in a few weeks e.g. roarer horses with [[Larynx Degenerative - Pathology#Laryngeal hemiplegia|laryngeal hemiplegia]] | ||
| + | ***May be reversible if innervation re-established | ||
| + | ***Histologically: | ||
| + | ****Fibres become rounded in cross section unless compressed by normal fibres | ||
| + | ****Increased concentration of nuclei as they take much longer to disintegrate | ||
| + | ****Fibrous stroma of epimysium and endomysium condenses -> more prominent | ||
| + | ****End result in muscle consisting of almost only fibrous tissue | ||
| + | ***Sometimes replaced by fat tissue -> increased size of muscle = ''pseudohypertrophy'' | ||
| + | ***Muscle may have a mixture of atrophied and [[Muscles Hyperplastic and Neoplastic - Pathology#Hypertrophy|hypertrophied]] (due to increased work load) fibres if some motor units are not damaged | ||
| + | **<u>'''Metabolisation of muscle protein'''</u> for nutrients during: | ||
| + | ***Malnutrition, cachexia, senility | ||
| + | ***Gradual onset except for some febrile diseases causing cachexia | ||
| + | ***Postural muscles are not affected, sometimes even [[Muscles Hyperplastic and Neoplastic - Pathology#Hypertrophy|hypertrophy]] | ||
| + | ***Histologically: | ||
| + | ****Some nuclei disappear as myofibre volume is decreased | ||
| + | ***Grossly: | ||
| + | ****Smaller, darker, thinner muscles | ||
| + | |||
| + | |||
| + | ==Toxic myopathy== | ||
| + | |||
| + | *'''Plants''' | ||
| + | **E.g. ''Cassia occidentalis'' (coffee senna), ''Karwinskia humboldtiana'' (coyotillo), ''Eupatorium rugosum'' (white snakeroot), cotton seed | ||
| + | **Lesion an skeletal and cardiac muscle | ||
| + | **Grossly: | ||
| + | ***Pale areas with ill-defined borders | ||
| + | ***May involve very extensive [[Muscles Degenerative - Pathology#Necrosis|necrosis]] | ||
| + | **Histologically: | ||
| + | ***Segmental necrosis, no calcification | ||
| + | ***[[Muscle Regeneration - Anatomy & Physiology|Regeneration]] may occur in surviving animals | ||
| + | *'''Drugs''' | ||
| + | **E.g. corticosteroids, cholinesterase inhibitors, vincristine, dimethyl sulfoxide (DMSO) | ||
| + | **'''Monensin''' is a coccidiostat toxic to horses, donkeys, zebras, cattle, sheep, dogs and birds | ||
| + | ***Causes muscle necrosis in heart and skeletal muscle | ||
| + | ***Grossly: | ||
| + | ****Pale streaks, mostly in hind limbs | ||
| + | ***Histologically: | ||
| + | ****[[Muscles Degenerative - Pathology#Necrosis|Segmental necrosis]] | ||
| + | ****Possibly [[Muscle Regeneration - Anatomy & Physiology|regeneration]] in surviving animals | ||
| + | ***Can cause rapid onset recumbency and potentially death | ||
| + | ***Usually due to mixing errors in feed | ||
| + | **Also from intramuscular injections, e.g. oxytetracycline, lidocaine, chloramphenicol, produce local necrosis | ||
| + | ***As satellite cells are destroyes, repair is via fibrosis with some budding | ||
| + | *'''Chemicals''' | ||
| + | **Iron injections can cause local myonecrosis | ||
| + | *'''Mycotoxins''' | ||
| + | **Metabolites cause persistent tremors | ||
| + | **Lesions in skeletal muscle only, possibly secondary to sustained contractions (similar to [[Muscles Degenerative - Pathology#Exertional myopathies|exertional myopathy]]) | ||
| + | **Histologically: | ||
| + | ***Tiny foci of [[Muscles Degenerative - Pathology#Necrosis|segmental necrosis]] | ||
| + | |||
| + | |||
| + | ==Endocrine myopathy== | ||
| + | |||
| + | *[[Adrenal Glands - Pathology#Adrenal Hyperfunction|Hyperadrenocorticism]] | ||
| + | **Muscle weakness is a clinical sign | ||
| + | **-> [[Muscles Degenerative - Pathology#Atrophy|muscle atrophy]] | ||
| + | ***Type II myofibre atrophy is non-specific | ||
| + | ***Type IIB myofibre atrophy is preferential in hyperadrenocorticism | ||
| + | *[[Thyroid Gland - Pathology#Hypothyroidism|Hypothyroidism]] can cause muscle atrophy | ||
| + | |||
| + | |||
| + | ==Nutritional myopathy== | ||
| + | [[Image:White muscle disease.jpg|right|thumb|100px|<small><center>White muscle disease (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | ||
| + | [[Image:White muscle disease histo.jpg|right|thumb|100px|<small><center>White muscle disease (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | ||
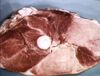
| + | ===[[White Muscle Disease - Pathology|White muscle disease]]=== | ||
| + | *Very important economic disease of sheep, cattle and pig | ||
| + | *Caused by: | ||
| + | **Deficiency of selenium, vitamin E or both | ||
| + | **Exacerbated by rapid growth, unaccustomed exercise or other dietary factor | ||
| + | *Pathogenesis: | ||
| + | **Oxygen free radicals (OFR) can damage cell membranes | ||
| + | **Vitamin E usually mops up OFRs | ||
| + | **Selenium as part of glutathione peroxidase neutralises effects of OFRs | ||
| + | **If Vit E or Se are deficient -> the balance shifts to membrane damage, calcium entry and mitochondrial damage -> cell swells and dies -> segmental muscle [[Muscles Degenerative - Pathology#Necrosis|necrosis]] | ||
| + | *Grossly: | ||
| + | **Lesions are bilaterally symmetrical in hard working muscles (vary with species) | ||
| + | **Early lesions are pale areas and streaks | ||
| + | ***Difficult to see especially in pale muscles | ||
| + | **Later becoming calcified necrotic areas | ||
| + | ***More obvious | ||
| + | **Pigs also have lesions in their [[Myocardial - Pathology#Hyaline degeneration|heart]] and [[Liver General Pathology - Pathology#Hepatosis dietica|liver]] | ||
| + | *Histologically: | ||
| + | **[[Muscles Degenerative - Pathology#Necrosis|Segmental necrosis]] +/- [[Muscles Degenerative - Pathology#Calcification|calcification]] and [[Muscle Regeneration - Anatomy & Physiology|regeneration]] | ||
| + | **Multifocal and multiphasic lesions | ||
| + | |||
| + | ==Exertional myopathies== | ||
| + | |||
| + | *Caused by intensive and exhaustive activity of major muscle masses | ||
| + | *Glycogen used up -> local heat and lactic acid -> muscle degeneration | ||
| + | *Other forms include '''capture myopathy''', racing greyhounds, sheep chased by dogs | ||
| + | |||
| + | |||
| + | ===Equine rhabdomyolysis=== | ||
| + | |||
| + | *'''Azoturia''' (Monday morning disease) | ||
| + | **Acute | ||
| + | **Due to exercise following a prolonged period of rest | ||
| + | **Clincal signs: | ||
| + | ***Unable to move | ||
| + | ***Sweating | ||
| + | ***Tremors | ||
| + | ***Swollen and hard lumbar, gluteal and femoral muscles | ||
| + | **Myoglobin leaks from muscle cells -> leaks into urine -> urine is dark red/brown (myoglobinuria) -> damages renal tubules | ||
| + | **Grossly: | ||
| + | ***Salmon pink muscles -> dark, moist, swollen +/- pale streaks | ||
| + | **Histologically: | ||
| + | ***Segmental myofibre [[Muscles Degenerative - Pathology#Necrosis|necrosis]] | ||
| + | ****Multifocal and monophasic, but may be multiphasic if repeated bouts | ||
| + | ***Both, type IIA and IIB fibres affected; type IIB preferentially affected in acute disease | ||
| + | ***Minor inflammatory reaction and calcification | ||
| + | |||
| + | *'''Tying-up''' | ||
| + | **Similar to azoturia but much milder | ||
| + | **Grossly - normal muscle | ||
| + | **Histologically - same as azoturia | ||
| + | |||
| + | |||
| + | ===Porcine stress syndrome=== | ||
| + | |||
| + | *'''Malignant hyperthermia''' | ||
| + | *Pigs, dogs, humans | ||
| + | *Possibly a cellular defect resulting in high intacellular calcium ion concentration | ||
| + | **-> Activates myofibrillar ATPase -> rapid intracellular glycolysis -> increase in body heat -> denature protein -> cell death -> leakage of cellular content -> oedema | ||
| + | *Grossly: | ||
| + | **Muscles are pale, soft and exudative | ||
| + | *Histologically: | ||
| + | **Segmental hypercontraction | ||
| + | **Monophasic, multifocal [[Muscles Degenerative - Pathology#Necrosis|segmental necrosis]] | ||
| + | *Inherited | ||
| + | *Triggered by halothane anaesthesia, stress of handling, transportation or slaughter | ||
| + | |||
| + | ==Neuromuscular junction diseases== | ||
| + | |||
| + | ===Aquired myasthenia gravis=== | ||
| + | |||
| + | *See [[Muscles Developmental - Pathology#Myasthenia gravis (MG)|congenital MG]] | ||
| + | |||
| + | |||
| + | ===Botulism=== | ||
| + | |||
| + | *Caused by: | ||
| + | **Ingestion of ''[[Clostridium botulinum]]'' toxin which inhibits acetyl choline release | ||
| + | *Diagnosis by demonstration of toxin in faeces, ingested material or serum | ||
| + | |||
| + | |||
| + | ==Circulatory disturbances== | ||
| + | |||
| + | ===Congestion=== | ||
| + | |||
| + | *Localised or generalised stasis -> dark red muscle | ||
| + | *E.g. in ruminal tympany ([[Bloat|bloat]]) - congestion of muscles cranial to thoracic inlet | ||
| + | *May resemble haemorhage grossly | ||
| + | |||
| + | |||
| + | ===Ischaemia=== | ||
| + | |||
| + | *Firstly [[Muscles Degenerative - Pathology#Necrosis|segmental necrosis]] | ||
| + | *-> death of satellite cells | ||
| + | **Causes [[Muscle Regeneration - Anatomy & Physiology|regeneration]] but myoblast precursors have to be recruited from viable fibres | ||
| + | *-> death of all cells | ||
| + | *Mostly healed by fibrosis and scar formation | ||
| + | *May attempt regeneration by [[Muscle Regeneration - Anatomy & Physiology|budding]] | ||
| + | Main causes: | ||
| + | *'''Vascular occlusion''' | ||
| + | **Infarction from embolism is rare due to collateral circulation | ||
| + | **Extension of infarcts depends on size of vessels occluded | ||
| + | ***Small capillaries -> segmental [[Muscles Degenerative - Pathology#Necrosis|necrosis]] | ||
| + | ***Large arteries -> whole muscle areas, including sattelite cells, are killed | ||
| + | **Healed by fibrosis | ||
| + | **May be due to: | ||
| + | ***Blockage of iliac arteries by aortic-iliac thrombosis in horses | ||
| + | ***Blockage of aortic bifurcation in cats | ||
| + | ***[[Dirofilaria immitis|''Dirofilaria immitis'']] arteritis in dogs | ||
| + | ***Vasculitis due to [[Reoviridae#Bluetongue Virus|bluetongue virus]] in sheep | ||
| + | ***[[Haemorrhage - Pathology#Purpura haemorrhagica|'''Equine purpura haemorrhagica''']] | ||
| + | ****Non-contagious, sporadic | ||
| + | ****Grossly: | ||
| + | *****Subcutaneous oedema | ||
| + | *****Scattered haemorrhagic foci throughout skin and muscles | ||
| + | *****Vasculitis -> infarcts of muscles | ||
| + | ****May cause myoglobinuria if extensive | ||
| + | ****Possibly immune mediated | ||
| + | ****In horses post [[:Category:Streptococcus species|streptococal]] infection, especially [[Respiratory Bacterial Infections - Pathology#Strangles|strangles]] | ||
| + | *'''External pressure''' | ||
| + | **During prolonged recumbency, e.g. anaesthesia, inability to rise, or due to too tightly fitting bandages or casts | ||
| + | **Post anaesthesia myopathy especially in horses | ||
| + | ***Dorsal recumbancy -> gluteals and longissimus ischaemia | ||
| + | ***Lateral recumbancy -> triceps brachii, pectoralis, deltoideus and brachiocephalicus ischaemia | ||
| + | **Caused by pressure on muscle > perfusion pressure of capillaries | ||
| + | **Downer cows - vetral recumbency -> ischaemia of pectoral muscles and muscles of limbs tucked under the animal | ||
| + | **Pregnant ewes with twins or triplets -> internal abdominal oblique muscle ischaemic necrosis -> potential rupture | ||
| + | *'''Muscle swelling''' where it cannot expand | ||
| + | **E.g. supracoracoid muscle infarction in some breeds of turkeys after flapping their wings | ||
| + | ***Surrounded by inelastic fascial sheath and bone | ||
| + | |||
| + | ==Trauma== | ||
| + | |||
| + | *Due to: | ||
| + | **Direct transection of myofibres | ||
| + | **Compression of myofibres | ||
| + | **Secondary from haemorrhage (bruising) | ||
| + | ***May increase muscle pressure -> [[Muscles Degenerative - Pathology#Ischaemia|ischaemia]] -> [[Muscles Degenerative - Pathology#Necrosis|necrosis]] | ||
| + | **Partial rupture - ''e.g.'' of diaphragm in road traffic accident | ||
| + | **Complete rupture - ''e.g.'' quadriceps of racing greyhounds | ||
| + | **Myorrhexis (tearing) - ''e.g.'' slippery floor causing 'splits' in cattle -> adductor muscle tear | ||
| + | *Healing is by [[Muscle Regeneration - Anatomy & Physiology|regeneration]] | ||
| + | *Fibrosis (scarring) will compromise function | ||
| + | *During [[Bones Fractures - Pathology|fractures]], fragments may cause further trauma if moved | ||
Revision as of 12:54, 28 May 2010
| This article has been peer reviewed but is awaiting expert review. If you would like to help with this, please see more information about expert reviewing. |
|
|
Degeneration
- Different types of degeneration
- May, or may not, be reversible
- Cloudy swelling, hydropic, vacuolar, granular and fatty change
- Occur following many different types of insult and are usually segmental
- If regeneration does not occur after formation of small vacuoles, necrosis follows
- Vacuolation -> floccular degeneration -> granular degeneration -> hyaline and Zenker’s degeneration
- Vacuolar degeneration:
- Due to swelling of organelles or due to glycogen or fat accumulation
- May be caused by hypokalaemia, hyperkalaemia or necrosis
- Histologically:
- Swollen
- Hypereosinophilic
- Lost cross striations
Calcification
- Due to:
- Old age - myofibres
- Following necrosis - dystrophic calcification
- May be visible grossly as white foci
Ossification
- Metaplasia of muscle to bone
- Localised
- Only in single muscle or a single group of muscles
- May be associated with trauma
- Seen in horses and dogs
- Histologically:
- Central zone - proliferating undifferentiated cells and fibroblasts
- Middle zone - osteoblasts depositing osteoid and bone
- Outer zone - trabecular bone remodelled by osteoclasts
- Progressive (fibrodysplasia ossificans progressiva)
- In connective tissue associated with skeletal muscle
- Secondary involvement of muscle tissue
- In pigs and cats
- Histologically:
- Bundles of dense fibrous connective tissue
- May contain accumulations of cartilage, bone or calcium
- Hyperplastic connective tissue -> compression of adjacent skeletal muscle -> atrophy
Pigmentation
- Lipofuscin
- Wear and tear pigment accumulating in secondary lisosomes -> converted into compact residual bodies
- Due to old age, past or recent cachexia or starvation
- Mostly stored in skeletal muscle of old high producing dairy cattle
- Masseters and diaphragm mainly involved
- No clinical importance
- Histologically:
- Rounded yellow to brown granules at both poles of nucleus of the skeletal myofiber
- Melanin
- As part of congenital melanosis of calves in fascial sheaths and epimysium
- Grossly - black foci
- Myoglobin
- After extensive muscle necrosis - rhabdomyolysis
- Leaks to adjacent tissue after sudden injury
- May also be present after some types of intramuscular injections e.g. iron dextran or tetracycline
Necrosis
- Necrosis of an entire myofibre is uncommon
- Segmental necrosis is more typical
- Muscle cell contents may leak into the blood if the cell membrane is damaged
- Creatine kinase (CK) is an enzyme which leaks following injury
- Used to measure the extent of muscle damage
- Often is followed by regeneration
- Histologically:
- Hyaline hypercontracted fiber rounded at cross-section and increased diameter and eosin staining
- May also be an artifact due to hypercontraction of normal fibres at fixation
- Fragmenting portions of fibre -> floccular or granular
- Normal portion of fibre may detach from necrotic part -> retraction caps
- Infarction may cause discoid degeneration - necrotic fibres detach at Z lines
- May mineralise
- Hyaline hypercontracted fiber rounded at cross-section and increased diameter and eosin staining
- Zenker's degeneration - secondary to systemic disease
- Scattered small segments of necrosis and fast regeneration
- Sacrolemmal tubes are intact
Atrophy
- Decreased myofibre or whole muscle diameter
- Myofibrils removed by disintegration -> sacrolemma too large -> forms folds
- Caused by:
- Disuse (e.g. fracture, failure to use limb, recumbency)
- Slower than denervation atrophy
- Reversible unless too prolonger or severe to cause loss of myofibres
- Denervation
- Any interference or damage to its nerve supply results in muscle atrophy
- Can be rapid - over 50% of muscle mass may be lost in a few weeks e.g. roarer horses with laryngeal hemiplegia
- May be reversible if innervation re-established
- Histologically:
- Fibres become rounded in cross section unless compressed by normal fibres
- Increased concentration of nuclei as they take much longer to disintegrate
- Fibrous stroma of epimysium and endomysium condenses -> more prominent
- End result in muscle consisting of almost only fibrous tissue
- Sometimes replaced by fat tissue -> increased size of muscle = pseudohypertrophy
- Muscle may have a mixture of atrophied and hypertrophied (due to increased work load) fibres if some motor units are not damaged
- Any interference or damage to its nerve supply results in muscle atrophy
- Metabolisation of muscle protein for nutrients during:
- Malnutrition, cachexia, senility
- Gradual onset except for some febrile diseases causing cachexia
- Postural muscles are not affected, sometimes even hypertrophy
- Histologically:
- Some nuclei disappear as myofibre volume is decreased
- Grossly:
- Smaller, darker, thinner muscles
- Disuse (e.g. fracture, failure to use limb, recumbency)
Toxic myopathy
- Plants
- E.g. Cassia occidentalis (coffee senna), Karwinskia humboldtiana (coyotillo), Eupatorium rugosum (white snakeroot), cotton seed
- Lesion an skeletal and cardiac muscle
- Grossly:
- Pale areas with ill-defined borders
- May involve very extensive necrosis
- Histologically:
- Segmental necrosis, no calcification
- Regeneration may occur in surviving animals
- Drugs
- E.g. corticosteroids, cholinesterase inhibitors, vincristine, dimethyl sulfoxide (DMSO)
- Monensin is a coccidiostat toxic to horses, donkeys, zebras, cattle, sheep, dogs and birds
- Causes muscle necrosis in heart and skeletal muscle
- Grossly:
- Pale streaks, mostly in hind limbs
- Histologically:
- Segmental necrosis
- Possibly regeneration in surviving animals
- Can cause rapid onset recumbency and potentially death
- Usually due to mixing errors in feed
- Also from intramuscular injections, e.g. oxytetracycline, lidocaine, chloramphenicol, produce local necrosis
- As satellite cells are destroyes, repair is via fibrosis with some budding
- Chemicals
- Iron injections can cause local myonecrosis
- Mycotoxins
- Metabolites cause persistent tremors
- Lesions in skeletal muscle only, possibly secondary to sustained contractions (similar to exertional myopathy)
- Histologically:
- Tiny foci of segmental necrosis
Endocrine myopathy
- Hyperadrenocorticism
- Muscle weakness is a clinical sign
- -> muscle atrophy
- Type II myofibre atrophy is non-specific
- Type IIB myofibre atrophy is preferential in hyperadrenocorticism
- Hypothyroidism can cause muscle atrophy
Nutritional myopathy
White muscle disease
- Very important economic disease of sheep, cattle and pig
- Caused by:
- Deficiency of selenium, vitamin E or both
- Exacerbated by rapid growth, unaccustomed exercise or other dietary factor
- Pathogenesis:
- Oxygen free radicals (OFR) can damage cell membranes
- Vitamin E usually mops up OFRs
- Selenium as part of glutathione peroxidase neutralises effects of OFRs
- If Vit E or Se are deficient -> the balance shifts to membrane damage, calcium entry and mitochondrial damage -> cell swells and dies -> segmental muscle necrosis
- Grossly:
- Histologically:
- Segmental necrosis +/- calcification and regeneration
- Multifocal and multiphasic lesions
Exertional myopathies
- Caused by intensive and exhaustive activity of major muscle masses
- Glycogen used up -> local heat and lactic acid -> muscle degeneration
- Other forms include capture myopathy, racing greyhounds, sheep chased by dogs
Equine rhabdomyolysis
- Azoturia (Monday morning disease)
- Acute
- Due to exercise following a prolonged period of rest
- Clincal signs:
- Unable to move
- Sweating
- Tremors
- Swollen and hard lumbar, gluteal and femoral muscles
- Myoglobin leaks from muscle cells -> leaks into urine -> urine is dark red/brown (myoglobinuria) -> damages renal tubules
- Grossly:
- Salmon pink muscles -> dark, moist, swollen +/- pale streaks
- Histologically:
- Segmental myofibre necrosis
- Multifocal and monophasic, but may be multiphasic if repeated bouts
- Both, type IIA and IIB fibres affected; type IIB preferentially affected in acute disease
- Minor inflammatory reaction and calcification
- Segmental myofibre necrosis
- Tying-up
- Similar to azoturia but much milder
- Grossly - normal muscle
- Histologically - same as azoturia
Porcine stress syndrome
- Malignant hyperthermia
- Pigs, dogs, humans
- Possibly a cellular defect resulting in high intacellular calcium ion concentration
- -> Activates myofibrillar ATPase -> rapid intracellular glycolysis -> increase in body heat -> denature protein -> cell death -> leakage of cellular content -> oedema
- Grossly:
- Muscles are pale, soft and exudative
- Histologically:
- Segmental hypercontraction
- Monophasic, multifocal segmental necrosis
- Inherited
- Triggered by halothane anaesthesia, stress of handling, transportation or slaughter
Neuromuscular junction diseases
Aquired myasthenia gravis
- See congenital MG
Botulism
- Caused by:
- Ingestion of Clostridium botulinum toxin which inhibits acetyl choline release
- Diagnosis by demonstration of toxin in faeces, ingested material or serum
Circulatory disturbances
Congestion
- Localised or generalised stasis -> dark red muscle
- E.g. in ruminal tympany (bloat) - congestion of muscles cranial to thoracic inlet
- May resemble haemorhage grossly
Ischaemia
- Firstly segmental necrosis
- -> death of satellite cells
- Causes regeneration but myoblast precursors have to be recruited from viable fibres
- -> death of all cells
- Mostly healed by fibrosis and scar formation
- May attempt regeneration by budding
Main causes:
- Vascular occlusion
- Infarction from embolism is rare due to collateral circulation
- Extension of infarcts depends on size of vessels occluded
- Small capillaries -> segmental necrosis
- Large arteries -> whole muscle areas, including sattelite cells, are killed
- Healed by fibrosis
- May be due to:
- Blockage of iliac arteries by aortic-iliac thrombosis in horses
- Blockage of aortic bifurcation in cats
- Dirofilaria immitis arteritis in dogs
- Vasculitis due to bluetongue virus in sheep
- Equine purpura haemorrhagica
- Non-contagious, sporadic
- Grossly:
- Subcutaneous oedema
- Scattered haemorrhagic foci throughout skin and muscles
- Vasculitis -> infarcts of muscles
- May cause myoglobinuria if extensive
- Possibly immune mediated
- In horses post streptococal infection, especially strangles
- External pressure
- During prolonged recumbency, e.g. anaesthesia, inability to rise, or due to too tightly fitting bandages or casts
- Post anaesthesia myopathy especially in horses
- Dorsal recumbancy -> gluteals and longissimus ischaemia
- Lateral recumbancy -> triceps brachii, pectoralis, deltoideus and brachiocephalicus ischaemia
- Caused by pressure on muscle > perfusion pressure of capillaries
- Downer cows - vetral recumbency -> ischaemia of pectoral muscles and muscles of limbs tucked under the animal
- Pregnant ewes with twins or triplets -> internal abdominal oblique muscle ischaemic necrosis -> potential rupture
- Muscle swelling where it cannot expand
- E.g. supracoracoid muscle infarction in some breeds of turkeys after flapping their wings
- Surrounded by inelastic fascial sheath and bone
- E.g. supracoracoid muscle infarction in some breeds of turkeys after flapping their wings
Trauma
- Due to:
- Direct transection of myofibres
- Compression of myofibres
- Secondary from haemorrhage (bruising)
- Partial rupture - e.g. of diaphragm in road traffic accident
- Complete rupture - e.g. quadriceps of racing greyhounds
- Myorrhexis (tearing) - e.g. slippery floor causing 'splits' in cattle -> adductor muscle tear
- Healing is by regeneration
- Fibrosis (scarring) will compromise function
- During fractures, fragments may cause further trauma if moved