Difference between revisions of "Insulinoma"
Michuang0720 (talk | contribs) |
JamesSwann (talk | contribs) |
||
| (15 intermediate revisions by 2 users not shown) | |||
| Line 1: | Line 1: | ||
| − | {{ | + | {{unfinished}} |
| − | == | + | *[[Adenoma|Adenomas]] and [[Carcinoma|carcinomas]] deerived from beta cells |
| + | *Respond rapidly to iv glucose | ||
| + | *Can be identified by immunocytochemical means | ||
| + | *Dogs 5-12 years of age most commonly affected | ||
| + | *Older cattle, associated with periodic convulsions | ||
| + | ====Clinical signs==== | ||
| + | *Hyperinsulinism | ||
| + | *Hypoglycaemia - often episodic | ||
| + | **Neurologic signs - stupor, confusion, coma, seizures, peripheral neuropathy may also develop | ||
| + | |||
| + | |||
| + | |||
| + | |||
| + | |||
| + | |||
| + | ==Description== | ||
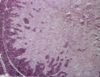
[[Image:Islet cell tumour.jpg|right|thumb|100px|<small><center>Islet cell tumour (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | [[Image:Islet cell tumour.jpg|right|thumb|100px|<small><center>Islet cell tumour (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | ||
| − | '''Insulinomas''' are slow growing, well-encapsulated, functional tumours of the [[Pancreas - Anatomy & Physiology#Endocrine|beta cells]] of the pancreatic | + | '''Insulinomas''' are slow growing, well-encapsulated, functional tumours of the [[Pancreas - Anatomy & Physiology#Endocrine|beta cells]] of the pancreatic islet cells. They secrete inappropriately high amount of [[Pancreas - Anatomy & Physiology#Insulin|insulin]], irrespective of the serum glucose level. They are predominantly [[Neoplasia - Pathology#Classification|malignant]] (90% of canine insulinomas), with a high metastatic rate to regional [[Lymph Nodes - Pathology|lymph nodes]], [[Liver - Anatomy & Physiology|liver]] and omentum. 60% of isulinomas are [[Neoplasia - Pathology#Nomenclature|carcinomas]], which are more likely to be endocrinologically active whereas the others are [[Neoplasia - Pathology#Nomenclature|adenomas]]. |
| − | Blood glucose concentration is | + | Blood glucose concentration is maintained within a narrow homeostatic range because several tissues are able to use only glucose as an energetic substrate. These tissues are particularly affected by the hypoglycaemia which occurs with hyperinsulinaemia and they include neurones, blood cells, renal medullary cells and fibroblasts in healing wounds. The release of hormones antagonistic hormones (such as glucagon, growth hormone, glucocorticoids and catecholamines) also contributes to the pathogenesis and clinical signs observed in animals with insulinoma. |
==Signalment== | ==Signalment== | ||
| − | Insulinomas occur most commonly in middle-aged or older dogs of the larger breeds. There is no sex predilection and the condition occurs less commonly in cats | + | Insulinomas occur most commonly in middle-aged or older dogs of the larger breeds. There is no sex predilection and the condition occurs less commonly in cats. |
==Diagnosis== | ==Diagnosis== | ||
===Clinical Signs=== | ===Clinical Signs=== | ||
| − | The following signs are related primarily to | + | The following signs are related primarily to hypoglycaemia but the release of catecholamines during episodes of hypogylcaemia may be contributory: |
*'''Collapse''' | *'''Collapse''' | ||
*'''Seizures''' | *'''Seizures''' | ||
| Line 20: | Line 35: | ||
*'''Exercise intolerance''' | *'''Exercise intolerance''' | ||
| − | These signs may be intermittent early in the course of the disease, but they become more frequent and sustained with time. In between hypoglycaemic episodes, the animals often appear to be normal. Hypoglycaemic episodes may occur shortly after feeding (as insulin secretion is stimulated) or a long time after feeding (as the animal cannot maintain its blood glucose in the acceptable range) and they may also be associated with exercise or excitement. | + | These signs may be intermittent early in the course of the disease, but they become more frequent and sustained with time. In between hypoglycaemic episodes, the animals often appear to be normal. Hypoglycaemic episodes may occur shortly after feeding (as insulin secretion is stimulated) or a long time after feeding (as the animal cannot maintain its blood glucose in the acceptable range) and they may also be associated with exercise or excitement. |
A presumptive diagnosis can be made on the basis of '''Wipple's triad''', which refers to the presence of: | A presumptive diagnosis can be made on the basis of '''Wipple's triad''', which refers to the presence of: | ||
| Line 36: | Line 51: | ||
*'''Serum fructosamine levels''' can also be assessed to gauge whether the animal has been persistently hypoglycaemic over the previous 2-3 weeks. A level <250-350 umol/l is suggestive of insulinoma | *'''Serum fructosamine levels''' can also be assessed to gauge whether the animal has been persistently hypoglycaemic over the previous 2-3 weeks. A level <250-350 umol/l is suggestive of insulinoma | ||
| − | === | + | ===Histopathology=== |
| − | + | This is needed for definitive confirmation of the diagnosis. The following features may be identified: | |
| − | + | *Usually single, or less often multiple, small (1-3cm) spherical nodules, yellow to dark red, in one or more lobes | |
| − | + | *Small islets of acinar tissue are sometimes present within the neoplasm | |
| − | |||
| − | |||
===Diagnostic Imaging=== | ===Diagnostic Imaging=== | ||
| Line 52: | Line 65: | ||
==Treatment== | ==Treatment== | ||
===Emergency Stabilisation=== | ===Emergency Stabilisation=== | ||
| − | In the event of a hypoglycaemic episode, a bolus | + | *In the event of a hypoglycaemic episode, a dextrose bolus should be given immdediately. |
| + | *This should be followed by intravenous fluid therapy with 2.5% dextrose. | ||
| + | *Alternatively, if the patient is able to eat, frequent feedings can be used instead of dextrose fluid therapy. This may be preferred to avoid the risk of rebound hypoglycaemia. | ||
| − | ===Medical | + | ===Medical=== |
| − | This is suitable for patients in which surgery has been declined or when | + | This is more suitable for patients in which surgery has been declined or when surgery is inappropriate or fails due to the presence of metastasis. |
*'''Small and frequent meals''' (3-6 times/day) of with high fat and protein content and some complex carbohydrate. | *'''Small and frequent meals''' (3-6 times/day) of with high fat and protein content and some complex carbohydrate. | ||
*'''Exercise restriction'''. | *'''Exercise restriction'''. | ||
| − | *[[Steroids|'''Glucocorticoids''']] such as prednisolone prescribed to increase hepatic gluconeogenesis and to decrease cellular glucose uptake. | + | *[[Steroids|'''Glucocorticoids''']] such as prednisolone may be prescribed to increase hepatic gluconeogenesis and to decrease cellular glucose uptake. |
| − | *'''Diazoxide''', an oral hyperglycaemic drug, used to inhibit pancreatic insulin secretion and tissue glucose uptake | + | *'''Diazoxide''', an oral hyperglycaemic drug, may be used to inhibit pancreatic insulin secretion and tissue glucose uptake. |
| − | |||
| − | === | + | ===Surgery=== |
| − | A '''partial pancreatectomy''' is suitable for patients with a solitary tumour and any suspected metastases may be removed or biopsied | + | A '''partial pancreatectomy''' is suitable for patients with a solitary tumour and any suspected metastases may be removed or biopsied at the same time. Possible post-operative complication include: |
| − | *'''Persistent hypoglycaemia''', probably due to the presence of unidentified metastases | + | *'''Persistent hypoglycaemia''', probably due to the presence of unidentified metastases |
| − | *[[Pancreatitis|'''Pancreatitis]]''' or ''' | + | *[[Pancreatitis - Dog and Cat|'''Pancreatitis]]''' or '''Diabetes mellitus''' due to disruption to the pancreatic parenchyma during the procedure |
| − | *'''Epilepsy''' and '''diffuse polyneuropathy''' due to chronic hypoglycaemia | + | *'''Epilepsy''' and '''diffuse polyneuropathy''' due to chronic hypoglycaemia |
| − | |||
==Prognosis== | ==Prognosis== | ||
| − | This is | + | This is dependent on the WHO staging of the tumour. A stage I and II can expect a median survival time of 18 months whereas it is only 6 months for a stage III. Patients suitable for surgical excision has better prognosis than those treated medically. |
| − | |||
| − | |||
| − | |||
| − | |||
==References== | ==References== | ||
| Line 84: | Line 93: | ||
| − | |||
| − | |||
| − | |||
[[Category:Pancreas_-_Hyperplastic_and_Neoplastic_Pathology]][[Category:Endocrine_System_-_Pathology]] | [[Category:Pancreas_-_Hyperplastic_and_Neoplastic_Pathology]][[Category:Endocrine_System_-_Pathology]] | ||
[[Category:Neoplasia]][[Category:Pancreas_-_Hyperplastic_and_Neoplastic_Pathology]][[Category:Endocrine_System_-_Pathology]] | [[Category:Neoplasia]][[Category:Pancreas_-_Hyperplastic_and_Neoplastic_Pathology]][[Category:Endocrine_System_-_Pathology]] | ||
| − | + | [[Category:Neoplasia]] | |
| − | [[Category: | + | [[Category:To_Do_-_James]] |
| − | [[Category: | + | [[Category:Cat]][[Category:Dog]] |
| − | |||
Revision as of 19:02, 6 July 2010
| This article is still under construction. |
- Adenomas and carcinomas deerived from beta cells
- Respond rapidly to iv glucose
- Can be identified by immunocytochemical means
- Dogs 5-12 years of age most commonly affected
- Older cattle, associated with periodic convulsions
Clinical signs
- Hyperinsulinism
- Hypoglycaemia - often episodic
- Neurologic signs - stupor, confusion, coma, seizures, peripheral neuropathy may also develop
Description
Insulinomas are slow growing, well-encapsulated, functional tumours of the beta cells of the pancreatic islet cells. They secrete inappropriately high amount of insulin, irrespective of the serum glucose level. They are predominantly malignant (90% of canine insulinomas), with a high metastatic rate to regional lymph nodes, liver and omentum. 60% of isulinomas are carcinomas, which are more likely to be endocrinologically active whereas the others are adenomas.
Blood glucose concentration is maintained within a narrow homeostatic range because several tissues are able to use only glucose as an energetic substrate. These tissues are particularly affected by the hypoglycaemia which occurs with hyperinsulinaemia and they include neurones, blood cells, renal medullary cells and fibroblasts in healing wounds. The release of hormones antagonistic hormones (such as glucagon, growth hormone, glucocorticoids and catecholamines) also contributes to the pathogenesis and clinical signs observed in animals with insulinoma.
Signalment
Insulinomas occur most commonly in middle-aged or older dogs of the larger breeds. There is no sex predilection and the condition occurs less commonly in cats.
Diagnosis
Clinical Signs
The following signs are related primarily to hypoglycaemia but the release of catecholamines during episodes of hypogylcaemia may be contributory:
- Collapse
- Seizures
- Muscle tremors and weakness
- Ataxia
- Lethargy and depression
- Exercise intolerance
These signs may be intermittent early in the course of the disease, but they become more frequent and sustained with time. In between hypoglycaemic episodes, the animals often appear to be normal. Hypoglycaemic episodes may occur shortly after feeding (as insulin secretion is stimulated) or a long time after feeding (as the animal cannot maintain its blood glucose in the acceptable range) and they may also be associated with exercise or excitement.
A presumptive diagnosis can be made on the basis of Wipple's triad, which refers to the presence of:
- Clinical signs associated with hypoglycaemia
- Fasting hypoglycaemia
- Amelioration of clinical signs with the administration of glucose
Laboratory Tests
Biochemistry
- Hypoglycaemia which should be a persistent finding during fasting.
- Serum ALT and ALK are often elevated but the significance of these findings is not known.
Other Tests
- Serum insulin concentration is usually elevated in the face of profound hypoglycaemia, with an insulin: glucose ratio of >4.2 considered to be diagnostic for insulinoma.
- Serum fructosamine levels can also be assessed to gauge whether the animal has been persistently hypoglycaemic over the previous 2-3 weeks. A level <250-350 umol/l is suggestive of insulinoma
Histopathology
This is needed for definitive confirmation of the diagnosis. The following features may be identified:
- Usually single, or less often multiple, small (1-3cm) spherical nodules, yellow to dark red, in one or more lobes
- Small islets of acinar tissue are sometimes present within the neoplasm
Diagnostic Imaging
Radiography
Thoracic radiographs may be used to identify any pulmonary metastases, but it is uncommon for insulinomas to metastasise to the lungs.
Ultrasonography
Occasionally, it may be possible to visualise the location of the neoplasm on the pancreas as a hypoechoic nodule. However, this may not always be possible, especially if the tumour is very small. Metastases to lymph nodes and liver can sometimes be identified but suspected hepatic metastases should always be biopsied.
Treatment
Emergency Stabilisation
- In the event of a hypoglycaemic episode, a dextrose bolus should be given immdediately.
- This should be followed by intravenous fluid therapy with 2.5% dextrose.
- Alternatively, if the patient is able to eat, frequent feedings can be used instead of dextrose fluid therapy. This may be preferred to avoid the risk of rebound hypoglycaemia.
Medical
This is more suitable for patients in which surgery has been declined or when surgery is inappropriate or fails due to the presence of metastasis.
- Small and frequent meals (3-6 times/day) of with high fat and protein content and some complex carbohydrate.
- Exercise restriction.
- Glucocorticoids such as prednisolone may be prescribed to increase hepatic gluconeogenesis and to decrease cellular glucose uptake.
- Diazoxide, an oral hyperglycaemic drug, may be used to inhibit pancreatic insulin secretion and tissue glucose uptake.
Surgery
A partial pancreatectomy is suitable for patients with a solitary tumour and any suspected metastases may be removed or biopsied at the same time. Possible post-operative complication include:
- Persistent hypoglycaemia, probably due to the presence of unidentified metastases
- Pancreatitis or Diabetes mellitus due to disruption to the pancreatic parenchyma during the procedure
- Epilepsy and diffuse polyneuropathy due to chronic hypoglycaemia
Prognosis
This is dependent on the WHO staging of the tumour. A stage I and II can expect a median survival time of 18 months whereas it is only 6 months for a stage III. Patients suitable for surgical excision has better prognosis than those treated medically.
References
- Ettinger, S.J. and Feldman, E. C. (2000) Textbook of Veterinary Internal Medicine Diseases of the Dog and Cat Volume 2 (Fifth Edition) W.B. Saunders Company.
- Fossum, T. W. et. al. (2007) Small Animal Surgery (Third Edition) Mosby Elsevier
- Nelson, R.W. and Couto, C.G. (2009) Small Animal Internal Medicine (Fourth Edition) Mosby Elsevier.
- Polton, G. A., White, R. N., Brearley, M. J. and Eastwood, J. M. (2007) Improved survival in a retrospective cohort of 28 dogs with insulinoma Journal of Small Animal Practice 48:151-156 [1]