Difference between revisions of "Parathyroid Glands - Pathology"
Jump to navigation
Jump to search
(Redirected page to Category:Parathyroid Glands - Pathology) |
(New page: {{toplink |backcolour = FAFAD2 |linkpage =Endocrine System - Pathology |linktext =Endocrine System |maplink = Endocrine System (Content Map) - Pathology |pagetype =Pathology }} <br> ==Anat...) |
||
| (12 intermediate revisions by 3 users not shown) | |||
| Line 1: | Line 1: | ||
| − | # | + | {{toplink |
| + | |backcolour = FAFAD2 | ||
| + | |linkpage =Endocrine System - Pathology | ||
| + | |linktext =Endocrine System | ||
| + | |maplink = Endocrine System (Content Map) - Pathology | ||
| + | |pagetype =Pathology | ||
| + | }} | ||
| + | <br> | ||
| + | ==Anatomy and Physiology== | ||
| + | Anatomy and Physiology of the Parathyroid glands can be found [[Endocrine System - Parathyroid Glands - Anatomy & Physiology|here]]. | ||
| + | ==Hypercalcaemia== | ||
| + | * Hypercalcaemia should not be ignored in an unwell animal. | ||
| + | ** The consequences of hypercalcaemia may be serious: prolonged untreated hypercalcaemia can lead to irreversible damage to many organs, particularly the kidneys. | ||
| + | ** There are multiple causes of hypercalcaemia, but if it is caught early a specific diagnosis and treatment are often possible. | ||
| + | * The clinical signs of hypercalcaemia are often vague. | ||
| + | ** Signs commonly include: | ||
| + | *** PU/PD | ||
| + | *** Anorexia | ||
| + | *** Dehydration | ||
| + | *** Weakness or lethargy | ||
| + | *** [[Control of Feeding - Anatomy & Physiology#The Vomit Reflex|Vomiting]] | ||
| + | *** Prerenal azotaemia | ||
| + | ** More uncommonly, hypercalcaemia may present with: | ||
| + | *** Constipation | ||
| + | *** Cardiac arrhythmia | ||
| + | *** Seizures or twitching | ||
| + | *** [[Kidney - Renal failure#Acute|Acute renal failure]] | ||
| + | *** Death | ||
| + | * Causes of hypercalcaemia may be: | ||
| + | *# Nonpathologic | ||
| + | *#* This may be due to: | ||
| + | *#** Age - young animals have naturally higher calcium levels. | ||
| + | *#** Lab error | ||
| + | *#** Lipaemia | ||
| + | *#* It is important to establish whether hypercalcaemia is true before persuing further diagnosis and treatment. | ||
| + | *# Transient... | ||
| + | *#* ...hypoadrenocorticism | ||
| + | *#* ...haemoconcentration | ||
| + | *#* ...hyperproteinaemia | ||
| + | *# Pathological | ||
| + | *#* Malignancy | ||
| + | *#* Lymphoma | ||
| + | *#* [[Parathyroid Glands - Pathology#Apocrine Gland Adenocarcinoma|Anal sac adenocarcinoma]] | ||
| + | *#* [[Kidney - Renal failure|Renal failure]] | ||
| + | *#* [[Bones - metabolic#Hypervitaminosis D|Hypervitaminosis D]] | ||
| + | *#* Granulomatous disease | ||
| + | *#** E.g fungal infections | ||
| + | *#* [[Parathyroid Glands - Pathology#Primary|Primary hyperparathyroidism]] | ||
| + | *#* Skeletal lesions | ||
| + | ==Hypocalcaemia== | ||
| + | * Hypocalcaemia is a relatively common finding in | ||
| + | ** Small animals | ||
| + | *** Most often associated with decreased albumin concentrations. | ||
| + | *** Usually clinically insignificant. | ||
| + | ** Farm animals | ||
| + | *** For example, dairy cows following parturition. | ||
| + | **** More clinically significant. | ||
| + | * Clinical signs may not always be present (i.e. clinically insignificant). | ||
| + | ** Clinical signs are most often seen in associated with lactation or post-operative causes. | ||
| + | ** When they seen, signs commonly include: | ||
| + | *** Facial rubbing | ||
| + | *** Muscle tremors or cramps | ||
| + | *** Stiff gait | ||
| + | *** Behavioural changes | ||
| + | ** The following are seen less commonly: | ||
| + | *** Panting | ||
| + | *** Pyrexia | ||
| + | *** Lethargy | ||
| + | *** Anorexia | ||
| + | *** Tachycardia or ECG abnormalities | ||
| + | *** Hypotension | ||
| + | *** Death | ||
| + | * Some causes of hypocalcaemia are also more common than others. | ||
| + | ** Common causes are: | ||
| + | *** Chronic renal failure | ||
| + | *** Hypoalbuminaemia | ||
| + | *** Eclampsia | ||
| + | *** Acute pancreatitis | ||
| + | *** Iatrogenic | ||
| + | *** Post thyroidectomy | ||
| + | *** Post parathyroidectomy | ||
| + | *** Blood transfusion | ||
| + | ** More uncommonly: | ||
| + | *** Lab error | ||
| + | *** Ethylene glycol toxicity | ||
| + | *** NaHCO<sub>3</sub> administration | ||
| + | *** Hypovitaminosis D | ||
| + | *** Hypomagnesaemia | ||
| + | *** Intestinal malabsorption | ||
| + | *** Primary hypoparathyroidism | ||
| + | ==Hyperparathyroidism== | ||
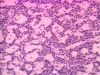
| + | [[Image:parathyroidadeoma.jpg|thumb|right|100px|Parathyroid adenoma. Image courtesy of Biomed Archive.]] | ||
| + | ===Primary=== | ||
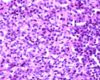
| + | * Primary hyperparathyroidism is caused by glandular hyperplasia or neoplasia. [[Image:parathyroidhyperplasia.jpg|thumb|right|100px|Parathyroid hyperplasia. Image courtesy of Biomed Archive.]] | ||
| + | * Rare. | ||
| + | ===Secondary=== | ||
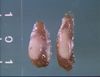
| + | * Secondary hyperparathyroidism causes [[Bones - metabolic#Hyperparathyroidism|fibrous osteodystrophy or "rubber jaw"]]. | ||
| + | * In secondary hyperparathyroidism, the gland is overactive due to another condition coexisting in the body, rather than a primary parathyroid gland defect. | ||
| + | * There are two common forms of secondary hyperparathyroisism: | ||
| + | *# [[Parathyroid Glands - Pathology#Nutritional Hyperparathyroidism|'''Nutritional Hyperparathyroidism''']] | ||
| + | *#* This includes [[Parathyroid Glands - Pathology#Metabolic Bone Disease|Metabolic Bone Disease]]. | ||
| + | *# [[Parathyroid Glands - Pathology#Renal Hyperparathyroidism|'''Renal Hyperparathyroidism''']] | ||
| + | * Both forms result in increased osteoclastic resorption of bone and deposition of fibro-osteoid matrix that fails to mineralise. | ||
| + | ** Flat bones of the skull swell. | ||
| + | ** Fibrous tissue is seen around the tooth roots. | ||
| + | ** Bone softens in adult animals. | ||
| + | *** This is what gives rise to the term "rubber jaw". | ||
| + | *** Long bones become soft with thin cortices. | ||
| + | **** These fracture easily. | ||
| + | ====Nutritional Hyperparathyroidism==== | ||
| + | [[Image:secondaryhyperparathyroidism.jpg|thumb|right|100px|Secondary hyperparathyroidism - "rubber jaw". Image courtesy of Biomed Archive.]] | ||
| + | * Nutritional hyperparathyroidism is also known as nutritional osteodystrophy. | ||
| + | * This occurs most commonly in: | ||
| + | ** Young, fast-growing animals | ||
| + | ** Animals with a poor diet, for example: | ||
| + | *** Swine fed unsupplemented cereal grain | ||
| + | *** Dogs and cats fed all-meat diets | ||
| + | *** Horses fed bran | ||
| + | **** In this case, nutritional hyperparathyroidism is known as "bran disease". | ||
| + | =====Pathogenesis===== | ||
| + | * Pathogenesis follows low calcium/high phosphate diets. | ||
| + | ** These lead to decreased serum calcium levels, stimulating [[Parathyroid Glands - Pathology#Hormonal Control|PTH]] release. | ||
| + | ** The increase in PTH gives an increase in bone resorption, causing pathology. | ||
| + | =====Pathology===== | ||
| + | * '''Gross''' | ||
| + | ** Severe cases may show: | ||
| + | *** Maxillary and mandibular swelling | ||
| + | *** [[Oral Cavity - Teeth & Gingiva - Anatomy & Physiology|Teeth]] lost or buried in soft tissue | ||
| + | *** Nasal and frontal bone enlargement, leading to dyspnoea | ||
| + | *** Long bone fracture | ||
| + | *** Detatchment tendons and ligaments | ||
| + | ** Early or less severe cases are characterised by shifting lameness and ill thrift. | ||
| + | * '''Histological''' | ||
| + | ** Osteoclastic resorption | ||
| + | ** Fibrous replacement | ||
| + | =====Metabolic Bone Disease===== | ||
| + | * Metabolic bone disease affects lizards in captivity, particularly young green iguanas | ||
| + | * The condition is caused by: | ||
| + | ** Dietary deficiency of calcium and vitamin D | ||
| + | *** For example, due to poor lighting (which diminishes viatmin D production). | ||
| + | ** Dietary excess of phosphorus | ||
| + | ** Certain toxicities | ||
| + | ** Diseases of the kidneys, [[Liver - Anatomy & Physiology|liver]] or parathyroid | ||
| + | *** This aetiology is rare | ||
| + | * Clinical signs include: | ||
| + | ** Lethargy | ||
| + | ** Inability to support weight | ||
| + | ** Rounded skull | ||
| + | ** Spontaneous fractures | ||
| + | ** Adult animals also show signs of [[Parathyroid Glands - Pathology#Hypocalcaemia|hypocalcaemia]] | ||
| + | * The skeleton shows reduced density on radiography. | ||
| + | ====Renal Hyperparathyroidism==== | ||
| + | * Renal Hyerparathyroidism is mostly seen in the dog as an expression of chronic renal disease. | ||
| + | =====Pathogenesis===== | ||
| + | [[Image:renalhyperparathyroidism.jpg|thumb|right|100px|Parathyroid hyperplasia in renal hyperparathyroidism. Image courtesy of Biomed Archive.]] | ||
| + | # Chronic renal disease results in reduced glomerular filtration. | ||
| + | # As glomerular filtration is reduced, phosphate is retained. Chronic renal failure also causes inadequate vitamin D production in the kidneys. | ||
| + | # Hyperphosphataemia develops due to phosphate retention. | ||
| + | #* Hypocalcaemia also occurs, as high levels of phosphate depress calcium levels. | ||
| + | # PTH is released in an attempt to maintain the correct blood calcium:phosphorous ratio. This can have several effects: | ||
| + | #* Parathyroid hyperplasia | ||
| + | #** I.e. '''renal secondary hyperparathyroidism'''. | ||
| + | #* Soft tissue mineralisation | ||
| + | #** Particularly seen in dogs | ||
| + | #** Calcium is commonly deposited in the subpleural connective tissue of the intercostal spaces. | ||
| + | #** Calcification also occurs in other sites, e.g. [[Forestomach - Anatomy & Physiology|stomach]] wall, lungs, kidneys. | ||
| + | #* Increased bone resorption | ||
| + | #** This causes fibrous osteodystrophy, or "rubber jaw". | ||
| + | =====Pathology===== | ||
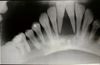
| + | [[Image:Renal_osteodystrophy.jpg|thumb|right|100px|"Rubber jaw" in renal osteodystrophy. Image courtesy of Biomed Archive.]] | ||
| + | * Pathology seen in renal hyperparathyroidism is very similar to that seen in nutritional hyperparathyroidism. | ||
| + | * '''Gross''' | ||
| + | ** The major gross presentation is a fibrous osetodystrophy, or rubber jaw. | ||
| + | *** The maxillae and mandible appear swollen. | ||
| + | *** Radiographically, bone shows reduced density, and [[Oral Cavity - Teeth & Gingiva - Anatomy & Physiology|teeth]] hence appear embedded in soft tissue. | ||
| + | *** However, only a few cases of chronic renal disease show such severe bone lesions. | ||
| + | ** Other lesions may also be seen. | ||
| + | *** Intercostal muscles may be calcified. | ||
| + | *** Bone marrow lesions may cause anaemia. | ||
| + | *** The lung may show oedema, and have calcified alveolar walls. | ||
| + | * '''Histological''' | ||
| + | ** Osteoclastic resorption | ||
| + | ** Fibrous replacement | ||
| + | ==Pseudo-Hyperparathyroidism== | ||
| + | * Non-endocrine tumours may be capable of secreting hormones, or hormone-like factors. | ||
| + | ** A parathormone-like substance may be secreted in such a manner. | ||
| + | ===Apocrine Gland Adenocarcinoma=== | ||
| + | * Malignant tumours of the anal sac apocrine glands can produce PTH-related peptide (PTHrp). | ||
| + | ** This induces a pseudo-hyperparathyroidism and hypercalcaemia. | ||
| + | ===[[Lymph Nodes - Pathology#Neoplasia|Lymphosarcoma]]=== | ||
| + | * 10 to 40% of cases in dogs may cause a pseudo-hyperparathyroidism. | ||
| + | ===Other Carcinomas=== | ||
| + | Some other carcinomas may also be capable of causing pseudo-hyperparathyroidism. | ||
| + | ==Hypoparathyroidism== | ||
| + | * Hypoparathyroidism may result from primary gland hypofunction. | ||
| + | ** Gland hypofunction occurs due to: | ||
| + | **# Destruction of secretory cells by a disease process. | ||
| + | **#* For example, this may be immune mediated, or another inflammatory cause. | ||
| + | **# A biochemical defect in synthetic pathway of the hormone. | ||
| + | **#* These are usually genetic aberrations. | ||
| + | **#* Defects in synthesis are not commonly identified in the veterinary species. | ||
Revision as of 10:32, 31 July 2008
|
|
Anatomy and Physiology
Anatomy and Physiology of the Parathyroid glands can be found here.
Hypercalcaemia
- Hypercalcaemia should not be ignored in an unwell animal.
- The consequences of hypercalcaemia may be serious: prolonged untreated hypercalcaemia can lead to irreversible damage to many organs, particularly the kidneys.
- There are multiple causes of hypercalcaemia, but if it is caught early a specific diagnosis and treatment are often possible.
- The clinical signs of hypercalcaemia are often vague.
- Signs commonly include:
- PU/PD
- Anorexia
- Dehydration
- Weakness or lethargy
- Vomiting
- Prerenal azotaemia
- More uncommonly, hypercalcaemia may present with:
- Constipation
- Cardiac arrhythmia
- Seizures or twitching
- Acute renal failure
- Death
- Signs commonly include:
- Causes of hypercalcaemia may be:
- Nonpathologic
- This may be due to:
- Age - young animals have naturally higher calcium levels.
- Lab error
- Lipaemia
- It is important to establish whether hypercalcaemia is true before persuing further diagnosis and treatment.
- This may be due to:
- Transient...
- ...hypoadrenocorticism
- ...haemoconcentration
- ...hyperproteinaemia
- Pathological
- Malignancy
- Lymphoma
- Anal sac adenocarcinoma
- Renal failure
- Hypervitaminosis D
- Granulomatous disease
- E.g fungal infections
- Primary hyperparathyroidism
- Skeletal lesions
- Nonpathologic
Hypocalcaemia
- Hypocalcaemia is a relatively common finding in
- Small animals
- Most often associated with decreased albumin concentrations.
- Usually clinically insignificant.
- Farm animals
- For example, dairy cows following parturition.
- More clinically significant.
- For example, dairy cows following parturition.
- Small animals
- Clinical signs may not always be present (i.e. clinically insignificant).
- Clinical signs are most often seen in associated with lactation or post-operative causes.
- When they seen, signs commonly include:
- Facial rubbing
- Muscle tremors or cramps
- Stiff gait
- Behavioural changes
- The following are seen less commonly:
- Panting
- Pyrexia
- Lethargy
- Anorexia
- Tachycardia or ECG abnormalities
- Hypotension
- Death
- Some causes of hypocalcaemia are also more common than others.
- Common causes are:
- Chronic renal failure
- Hypoalbuminaemia
- Eclampsia
- Acute pancreatitis
- Iatrogenic
- Post thyroidectomy
- Post parathyroidectomy
- Blood transfusion
- More uncommonly:
- Lab error
- Ethylene glycol toxicity
- NaHCO3 administration
- Hypovitaminosis D
- Hypomagnesaemia
- Intestinal malabsorption
- Primary hypoparathyroidism
- Common causes are:
Hyperparathyroidism
Primary
- Primary hyperparathyroidism is caused by glandular hyperplasia or neoplasia.
- Rare.
Secondary
- Secondary hyperparathyroidism causes fibrous osteodystrophy or "rubber jaw".
- In secondary hyperparathyroidism, the gland is overactive due to another condition coexisting in the body, rather than a primary parathyroid gland defect.
- There are two common forms of secondary hyperparathyroisism:
- Both forms result in increased osteoclastic resorption of bone and deposition of fibro-osteoid matrix that fails to mineralise.
- Flat bones of the skull swell.
- Fibrous tissue is seen around the tooth roots.
- Bone softens in adult animals.
- This is what gives rise to the term "rubber jaw".
- Long bones become soft with thin cortices.
- These fracture easily.
Nutritional Hyperparathyroidism
- Nutritional hyperparathyroidism is also known as nutritional osteodystrophy.
- This occurs most commonly in:
- Young, fast-growing animals
- Animals with a poor diet, for example:
- Swine fed unsupplemented cereal grain
- Dogs and cats fed all-meat diets
- Horses fed bran
- In this case, nutritional hyperparathyroidism is known as "bran disease".
Pathogenesis
- Pathogenesis follows low calcium/high phosphate diets.
- These lead to decreased serum calcium levels, stimulating PTH release.
- The increase in PTH gives an increase in bone resorption, causing pathology.
Pathology
- Gross
- Severe cases may show:
- Maxillary and mandibular swelling
- Teeth lost or buried in soft tissue
- Nasal and frontal bone enlargement, leading to dyspnoea
- Long bone fracture
- Detatchment tendons and ligaments
- Early or less severe cases are characterised by shifting lameness and ill thrift.
- Severe cases may show:
- Histological
- Osteoclastic resorption
- Fibrous replacement
Metabolic Bone Disease
- Metabolic bone disease affects lizards in captivity, particularly young green iguanas
- The condition is caused by:
- Dietary deficiency of calcium and vitamin D
- For example, due to poor lighting (which diminishes viatmin D production).
- Dietary excess of phosphorus
- Certain toxicities
- Diseases of the kidneys, liver or parathyroid
- This aetiology is rare
- Dietary deficiency of calcium and vitamin D
- Clinical signs include:
- Lethargy
- Inability to support weight
- Rounded skull
- Spontaneous fractures
- Adult animals also show signs of hypocalcaemia
- The skeleton shows reduced density on radiography.
Renal Hyperparathyroidism
- Renal Hyerparathyroidism is mostly seen in the dog as an expression of chronic renal disease.
Pathogenesis
- Chronic renal disease results in reduced glomerular filtration.
- As glomerular filtration is reduced, phosphate is retained. Chronic renal failure also causes inadequate vitamin D production in the kidneys.
- Hyperphosphataemia develops due to phosphate retention.
- Hypocalcaemia also occurs, as high levels of phosphate depress calcium levels.
- PTH is released in an attempt to maintain the correct blood calcium:phosphorous ratio. This can have several effects:
- Parathyroid hyperplasia
- I.e. renal secondary hyperparathyroidism.
- Soft tissue mineralisation
- Particularly seen in dogs
- Calcium is commonly deposited in the subpleural connective tissue of the intercostal spaces.
- Calcification also occurs in other sites, e.g. stomach wall, lungs, kidneys.
- Increased bone resorption
- This causes fibrous osteodystrophy, or "rubber jaw".
- Parathyroid hyperplasia
Pathology
- Pathology seen in renal hyperparathyroidism is very similar to that seen in nutritional hyperparathyroidism.
- Gross
- The major gross presentation is a fibrous osetodystrophy, or rubber jaw.
- The maxillae and mandible appear swollen.
- Radiographically, bone shows reduced density, and teeth hence appear embedded in soft tissue.
- However, only a few cases of chronic renal disease show such severe bone lesions.
- Other lesions may also be seen.
- Intercostal muscles may be calcified.
- Bone marrow lesions may cause anaemia.
- The lung may show oedema, and have calcified alveolar walls.
- The major gross presentation is a fibrous osetodystrophy, or rubber jaw.
- Histological
- Osteoclastic resorption
- Fibrous replacement
Pseudo-Hyperparathyroidism
- Non-endocrine tumours may be capable of secreting hormones, or hormone-like factors.
- A parathormone-like substance may be secreted in such a manner.
Apocrine Gland Adenocarcinoma
- Malignant tumours of the anal sac apocrine glands can produce PTH-related peptide (PTHrp).
- This induces a pseudo-hyperparathyroidism and hypercalcaemia.
Lymphosarcoma
- 10 to 40% of cases in dogs may cause a pseudo-hyperparathyroidism.
Other Carcinomas
Some other carcinomas may also be capable of causing pseudo-hyperparathyroidism.
Hypoparathyroidism
- Hypoparathyroidism may result from primary gland hypofunction.
- Gland hypofunction occurs due to:
- Destruction of secretory cells by a disease process.
- For example, this may be immune mediated, or another inflammatory cause.
- A biochemical defect in synthetic pathway of the hormone.
- These are usually genetic aberrations.
- Defects in synthesis are not commonly identified in the veterinary species.
- Destruction of secretory cells by a disease process.
- Gland hypofunction occurs due to: