Lymphoma
Also known as: Lymphosarcoma — Malignant Lymphoma
Introduction
Lymphoma is caused by malignant clonal expansion of lymphoid cells and most commonly arises from lymphoid tissues including the bone marrow, thymus, lymph nodes and spleen. Lymphoma is documented to be the most common haematopoietic neoplasm in dogs.
Classification
- Cytological classification
- Well differentiated (lymphocytic) - The malignant cells represent normal lymphocytes, although in excessive numbers.
- Poorly differentiated (lymphoblastic) - The malignant cells represent atypical lymphocytic cells with lymphoblastic characteristics.
- Tumour distribution
- Nodular/ follicular - A well organised pattern of slow growth, no metastasis, they are of the B-lymphocyte type
- Diffuse - Result in effacement of normal lymphoid architecture by a very homogeneous population of lymphoid cells.
- Anatomical classification
- Thymic - Only the thymus is affected.
- Alimentary - Gut and associated lymphoid tissue affected.
- Multicentric - Widespread involvement of lymph nodes.
- Cutaneous lymphoma - Usually presents as generalised skin disease, but is a malignant transformation of T cells with a propensity for epithelial sites.
- Type of lymphocyte - T-cell, B-cell or NK-cell
- Time scale - Acute or Chronic
Order of prevalence in UK is cats, dogs, cattle, pigs and sheep. In the cat and ox, viral agents have been identified as the causal agents.
Dog
Lymphoma is one of the prevalent neoplasms in the dog. The incidence is about 28 per 100,000 dogs. Blood of affected dogs shows neither a relative nor absolute increase in the number of lymphocytes until the late stages of the disease. When this stage is reached, poorly differentiated cells may appear in the blood.
In the dog, multicentric lymphoma is most common representing 80% of cases. Alimentary, cutaneous, mediastinal and extranodal sites are less common. Additionally the majority of lymphoma cases in dogs are of the B-cell immunophenotype.
Cat
FeLV is an important cause of lymphoma in the cat. Following the introduction of widespread FeLV testing and vaccination the most common type of lymphoma affecting cats is alimentary when previously it had been mediastinal and multicentric forms. Only 10% of lymphoma cases in cats are now associated with FeLV, whereas it used to be 70%.
The alimentary form arises from the mesenteric lymph nodes or intestine, liver. The thymic form presents as a thymic mass. The bronchial, cranial mediastinal and pre-sternal lymph nodes may potentially be affected. The multicentric form is rare in the cat. This form originates in the peripheral lymph nodes, later involving liver, spleen and other organs, eventually bone marrow in some cases. Cats can also develop extra-nodal lymphoma in several sites including the CNS and kidneys. A leukaemic form affecting the bone marrow alone is rare.
Horse
In horses, lymphoma is the most common haemopoietic neoplasm. It has been characterised into four main forms: alimentary, cutaneous, mediastinal and multicentric, however, it takes mainly the alimentary form.
Cattle
Cattle suffer both lymphosarcoma and leukosis in a variety of cytological forms. Bovine lymphoma is caused by Bovine Leukaemia Virus (BLV). There is a juvenile form of bovine lymphoma seen in young cattle which is not associated with BLV.
Pig
Porcine disease is mainly multicentric affecting lymph nodes, liver and spleen.
Sheep
Ovine lymphoma is uncommon. It may be multicentric or thymic.
Signalment
Dog
Affected dogs have a wide age range, most are middle-aged however young animals can be affected, 80% of cases affect the 5 to 11 year old age group. There may also be a male predilection.
Cat
The median age of affected cats is 9-10 years and oriental cat breeds may be predisposed.
Horse
There are no sex, age or breed predilections.
Clinical Signs
Dogs
Multicentric Lymphoma
- The most common presenting sign in dogs is a lymphadenopathy, with only 10-20% of dogs presenting clinically unwell. Dogs that do present with clinical signs may be anorexic, lethargic and have lost weight.
For other types of lymphoma affecting dogs the clinical signs will demonstrate the anatomical site affected.
Mediastinal forms may present with dyspnoea due to compression of the trachea and lungs. Dogs with mediastinal lymphoma can also have pitting oedema of the head and neck due to compression of the cranial vena cava, called caval syndrome. On ausculatation there is often an absence of lung sounds cranially and caudal displacement of the normal cardiac sounds, and dullness on percussion of the cranial thorax. Polyuria and polydypsia may be present due to paraneoplastic hypercalcaemia. Differential diagnoses for a cranial mediastinal mass include: thymoma, thyroid adenocarcinoma, a mediastinal abscess, or a branchial cyst.
Alimentary forms may present with signs such as vomiting, diarrhoea, anorexia and thickened loops of intestine or mass lesions on abdominal palpation.
Cutaneous lymphoma can also occur with a varied presentation but often present as cutaneous nodules or plaques.
Cats
In contrast to dogs, cats are more likely to present unwell. Again the clinical signs will depend on the anatomical location affected.
Alimentary cats often present with vomiting, diarrhoea, weight loss and anorexia.
Mediastinal cats may present with signs of compression of structures in the cranial thorax or with dyspnoea from an associated pleural effusion. Signs include dyspnoea, coughing and tachypnoea due to compression of the trachea. Weight loss and regurgitation may also occur secondary to compression of the oesophagus though these are rare. On auscultation, lung sounds are displaced caudally and lung sounds are decreased ventrally. There may be a loss of compressibility ('rib spring') over the cranial thorax. Differential diagnoses for a cranial mediastinal mass include: thymoma, thyroid adenocarcinoma, a mediastinal abscess, or a branchial cyst.
Renal lymphoma also occurs in cats and affected animals will typically present with bilateral renomegally and signs similar to renal failure.
Nasal lymphoma cases may present with any of dyspnoea, nasal discharge, epistaxis, facial pain or distortion and loss of airflow.
Horse
A thoracic effusion may occur in the alimentary and multicentric forms of the disease, which usually has the characteristics of a modified transudate.
Mediastinal lymphoma also produces clinical signs such as pointing of the forelimb, tachycardia, distension of the jugular vein and caudal displacement of the heart - it may be confused with colic. It should be differentiated from mediastinal abscessation by ultrasound of the mass and cytology of pleural fluid.
Intra-abdominal neoplasia (which can be multicentric or alimentary) may presents with a history of chronic weight loss and inappetance, recurring colic and intermittant pyrexia.
Physical Examination
Cat and Dog
Findings will depend on the anatomic region affected as described above. For example, an abdominal mass may be palpable and bowel loops may feel thickened in alimentary lymphoma. Additionally enlarged mesenteric lymph nodes and enlarged abdominal organs may be palpable. Muffled heart sounds and a non-compressible thoracic region may be found in mediastinal lymphoma. Petechiae, anaemia and icterus may also be present in any form of lymphoma.
Horse
Mediastinal masses can sometimes be palpable externally at the base of the jugular groove, due to the mass extending through the thoracic inlet.
Diagnosis
Laboratory Tests
Haematological analysis should always be performed with suspected lymphoma for staging purposes and for the recording of base-line parameters prior to the initiation of any treatment to assess the severity of any future myelosuppression. Potential abnormalities for those patients with bone marrow involvement may include lymphocytosis, thrombocytopenia, neutropenia and the presence of immature lymphoid precursors.
Affected cats and dogs are not usually leukemic.
On biochemistry abnormalities may include hypoproteinaemia, elevated hepatic enzymes and elevated Blood Urea Nitrogen /creatinine, but again these will depend on the area affected. A percentage of dogs will present with hypercalcemia of malignancy (see below), affecting both total and ionized calcium and in some cases causing a secondary azotaemia.
All cats with suspected lymphoma should be tested for FeLV and FIV, usually performed via enzyme-linked immunosorbent assay (ELISA) available in general practice in kit form (CITE test). False negatives are very rare but false positives can be seen depending on the sensitivity and specificity of the assay and if the diagnosis does not fit with the clinical picture, a confirmatory test should be performed such as viral isolation. Vaccination for FeLV does not lead to false positive results on the ELISA as the test looks for antigen. However, the current FIV vaccines available in the USA do not have a marker and so can lead to false positive FIV antibody SNAP tests.
Paraneoplastic Syndrome Dogs may present with hypercalcaemia, this is due to the release of parathyroid hormone - related protein (PTHrp) released by the tumor, which produces these effects by acting like parathyroid hormone. Affected cats are not usually hypercalcaemic.
Radiography
Nodal or organomegally may be visible radigraphically depending on the area affected. Other imaging modalities such as CT or MRI may be more appropriate for investigating nasal or CNS lymphoma, where available.
Ultrasonography
Superior to radiography in some areas for assessing abnormalities of tissue architecture and assessing the surrounding structures for metastasis. Guided aspirates or biopsies may also be taken at this time, including lymph node sampling, to evaluate degree of systemic involvement.
Cytology
Cytology is a necessary tool in the work-up of a lymphoma case. It provides both a diagnosis and a prognosis when combined with the entire clinical picture. Lymphoma produces a cell population which is both distinct and recognisable, allowing identification and classification of the type of lymphoma by cytology. Fine needle aspiration is a quick, cheap, non-invasive and effective method for collecting cells for cytology, and should always be considered a first-line test. Ideally cytology should always be supported by histology for immunophenotyping to distinguish B and T cell forms. Hyperplastic or reactive lymph nodes can be difficult to interpret and a second opinion from a qualified cytologist should always be taken when available prior to commencing treatment.
Cytology can also be used to examine pleural fluid samples if there is a suspicion of neoplasia.
Smears should be stained and examined microscopically.
Cytological criteria for lymphoma:
- Large amounts of lymphoblasts
- Large nuclei and prominent nucleoli
- High mitotic rate - bizarre mitotic figures may be present
- Small volume of basophilic cytoplasm
- Coarse chromatin
These features can be assessed to determine the grade of tumour and therefore the likely treatment response and progression of disease though the prognostic ability of cytology remains poor. Small well-differentiated lymphocytes normally suggest a low-grade lymphoma, and large, poorly differentiated lymphoid cells suggest a higher grade of lymphoma and with that a poorer prognosis.
Dogs
- Canine lymphoma is most commonly multicentric, therefore the ideal method for collecting a sample for cytological examination is fine needle aspiration of the lymph nodes. Ideally samples should come from multiple nodes to give a representative sample. Popliteal and prescapular lymph nodes are easily accessible and therefore ideal for sampling. Submandibular lymph nodes should be avoided where possible as they are commonly enlarged and reactive as a result of dental disease. It should be noted that canine lymphoma can occur in any organ containing lymphoid tissue.
Cats
- Feline lymphoma is more variable in its presentation, with extra-nodal forms being the commonest in general practice in the UK. The sample taken for cytological examination should be appropriate for the type of lymphoma:
- Ultrasound guided aspirates, partial thickness endoscopic grab biopsies or full thickness biopsies via exploratory laparotomy for intestinal lymphoma
- Pleural fluid aspirate with or without supporting ultrasound-guided aspirate or core biopsy of a mediastinal mass (which will in most cases differentiate it from thymoma though for some flow cytometry is necessary to make this distinction)
- Peripheral lymph node aspirates for multicentric lymphoma
- Lymphoma can occur in any tissue containing lymphoid tissue, for example the eye, kidney, CNS, liver, upper respiratory tract, lungs and skin. Cytology is an essential tool for diagnosis in these cases, as the lymphoma can present with variable clinical signs and diagnosis can only be confirmed using cytology. As mentioned above, the cytological diagnosis should be supported by histopathology if possible, particularly if the cytological result is equivocal.
- NB. Lymphoma should not be confused with reactive lymphoid hyperplasia in the healthy cat. Generalised lymphadenopathy may present like multicentric lymphoma but is in fact a natural immune response in the healthy cat. The same should be considered in other types of lymphoma, for example hepatic lymphoma looks cytologically very similar to lymphocytic periportal hepatitis, and it is necessary to incorporate the entire clinical picture when making a diagnosis. Histopathological sampling is ideal for confirming the diagnosis.
Horse
- In equine lymphoma, neoplastic cells are not always present, but when they are this may allow diagnosis.
- A sample of pleural or peritoneal fluid may be taken and examined cytologically if it is present. Otherwise a direct fine needle aspirate of the mass of lymph nodes may be performed. The fluid should be a modified transudate and contain a mixed cell population. Neoplastic lymphocytes are pleomorphic round cells that demonstrate anisocytosis and anisokaryosis and have very basophilic cytoplasm. If these cells are present then the diagnosis of lymphoma can be confirmed, otherwise surgical biopsy may be necessary.
Biopsy
A biopsy may be required if diagnosis cannot be made from fine needle aspirates. This may occur if; the aspirate provided a low number of cells; the cells were badly preserved or the disease is in its early stages. If the lymph node is biopsied, it is best to remove the entire node in an excisional biopsy so the tissue architecture remains intact.
Biopsy may also be indicated it the neoplasia is localised to a specific organ which is not amenable to ultrasound guided FNA, for example the gastrointestinal tract.
Nasal lymphoma can be diagnosed by rhinoscopic or blind biopsy using a suction-catheter or grab-forceps technique.
Bone marrow aspiration or biopsy is needed to stage the disease.
Pathology
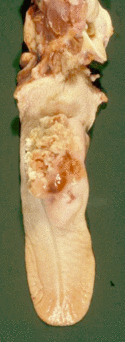
Secondary liver tumours are the most common secondary malignancy. They can be present as nodules or as diffuse infiltration along the portal tracts. Grossly, the liver is enlarged, turgid and friable with many minute pale foci. The whole organ is diffusely pale. Microscopically, tumour cells are seen to spread diffusely through the sinusoids.
Splenomegaly occurs in multicentric lymphosarcoma. Splenic enlargement may be marked if any form of lymphosarcoma is in leukaemic phase.
Staging
A staging system is used for multicentric lymphoma (Owen, 1980):
- Stage I - Involvement limited to a single node or lymphoid tissue in a single organ (excluding bone marrow)
- Stage II - Involvement of many lymph nodes in a regional area (+/- tonsils)
- Stage III - Generalised lymph node involvement
- Stage IV - Liver and/or spleen involvement (+ stage III)
- Stage V - Manifestations in the blood and involvement of bone marrow and/or other organ systems (+/-stages I-IV)
Each stage is then subclassifed as a) without systemic signs or b) with systemic signs. Other lymphomas such as primary hepatic are typically automatically classed as a grade V.
Treatment
Cats and Dogs
Surgery
- Firstly, a laparotomy is required for many cases of alimentary lymphoma to obtain biopsy material and in some cases to de-bulk and obstructing mass, though owners should be warned of the high potential of dehiscence post-operatively. For solitary masses without systemic disease, resection and anastomosis of the intestine is advised (single modality treatment). Local resection in cats has occasionally been curative. Other focal lymphoma may also be resected, however as there is typically systemic involvement, chemotherapy will be required (multimodal treatment).
Radiotherapy
- Lymphoma is highly radiosensitive and in theory radiotherapy should be efficient in treating all forms of lymphoma, however, surrounding tissues often have a low tolerance. The main site for which radiotherapy is used is in nasal lymphoma, though many oncologists combine this with systemic chemotherapy. Half body radiotherapy is currently being trialled in the USA as part of a multi-modal protocol.
Chemotherapy
- Combination chemotherapy is the most frequent method of treatment and the most commonly used protocols include:
- COP which consists of cyclophosphamide, vincristine and prednisolone. It is frequently used in cats and can be used for induction therapy (8 weeks) as well as a long term maintenance protocol.
- COAP consists of cyclophosphamide, vincristine, prednisolone and cytosine arabinoside
- CHOP consists of cyclophosphamide, vincristine, prednisolone and doxorubicin.
- Prednisolone and chlorambucil can provide good long term palliation in low grade lymphomas, for example feline small cell gastrointestinal lymphoma.
- Corticosteroids must not be administered prior to initiation of chemotherapy as they can cause resistance to cytotoxics and hence reduce the rate of response and the survival time. The aim is to induce remission and then continue with a maintenance regime, adjusting the dose as required with rescue therapy should relapse occur.
- Response to treatment can be monitored via reduction in tumour mass or size of lymph nodes. Haematological values should be frequently monitored to assess the effects of the drugs. In particular, animals should be monitored for the presence of azotaemia, neutropenia/sepsis, hypercalcaemia and pyrexia.
Supportive Therapy Whilst receiving chemotherapy. patients should receive a high quality, palatable diet to maintain calorific intake. If animals become anorexic, the cause should be investigated.
Prognosis Unfortunately it is unusual for animals with lymphoma to be cured, and whilst the disease goes into remission in most patients treated with multi-modal chemotherapy, typically they will relapse after a period of weeks to months. At this time, rescue chemotherapy can be performed but often does not provide a long second remission period.
Horses
Treatment is symptomatic and euthanasia may be required with the progression of clinical signs.
Prognosis
Cats and Dogs
The mean survival times for dogs and cats without therapy is 6-8 weeks. For those receiving corticosteroids alone it is thought to be around 3 months.
If chemotherapy is administered then the mean survival time increases to 6-12 months for canine multicentric lymphoma depending on the protocol used and a huge variety of other factors - the median survival of other disease sites and species is less well documented. Documented poor prognostic indicators in the dog include T cell immunophenotype, cranial mediastinal involvement, hypercalcemia, bone marrow involvement and being ill at diagnosis (substage b). Local canine lymphoma responds better to chemotherapy than the diffuse form of disease. Immunophenotype (T cell versus B cell lymphoma) does not appear to be associated with prognosis in cats as it can be in dogs. Factors indicating a better prognosis (overall survival) in cats include: an early presentation, a complete initial response to treatment and a clinically well patient (‘substage a’ disease).
In cats, response rate to induction chemotherapy is 26-79% and there is an apparently a poorer response rate in cats compared with dogs, however, 30-40% of cats that do have complete remission and will maintain complete remission for two years or more and long-term maintenance chemotherapy can frequently be stopped and many will then live free of disease. Hence, dogs may have higher remission rates but are less likely than cats to be able to maintain remission without chemotherapy.
Horse
The prognosis is poor and definitive diagnosis is usually achieved on post-mortem examination.
| Lymphoma Learning Resources | |
|---|---|
To reach the Vetstream content, please select |
Canis, Felis, Lapis or Equis |
 Test your knowledge using flashcard type questions |
Feline Medicine Q&A 12 Feline Medicine Q&A 19 Cytology Q&A 03 Cytology Q&A 10 Equine Internal Medicine Q&A 18 |
 Search for recent publications via CAB Abstract (CABI log in required) |
Lymphoma in dogs publications |
References
Copas, V (2011) Diagnosis and treatment of equine pleuropneumonia In Practice 2011 33: 155-16
Cowell, R. (2002) Diagnostic cytology and haematology of the horse Elsevier Health Sciences
Freeman, KP (2007) Self-Assessment Colour Review of Veterinary Cytology - Dog, Cat, Horse and Cow Manson
Gear, R (2009) Practical update on canine lymphoma : 1. Classification and Diagnosis In Practice 2009 31: 380-384
Hayes A. (2006) Feline lymphoma 1. Principles of diagnosis and management, In Practice, 28, pp 516-524
Hayes, A (2006) Feline lymphoma 2. Specific Disease Presentations In Practice 2006 28, pp 578-585
Head K. W, Else R. W, Dubielzig R.R, (2002) Tumours of the Alimentary Tract, in Tumours in Domestic Animals, 4th edition, Ed Menten D. J, Iowa State Press, Blackwell Publishing, Iowa, pp 471-472
Hewetson, M (2006) Investigation of false colic in the horse In Practice 2006 28: 326-33
Milne, E (2004) Peritoneal fluid analysis for the differentiation of medical and surgical colic in horses In Practice 2004 26: 444-44
Morris J, Dobson J (2001) Gastrointestinal Tract, in Small Animal Oncology, Blackwell Science, pp 228-239
Selting K. A, (2007), Intestinal Tumours, Cancer of the Gastrointestinal Tract, in Withrow and MacEwen's Small Animal Clinical Oncology, fourth edition, Eds Withrow S.J, Vail D.M, Missouri, Saunders Elsevier, pp 491-501
Sparks, AH & Caney, SMA (2005) Self-Assessment Colour Review Feline Medicine Manson
Stell, A (2009) Haemopoetic Neoplasia - Lymphoreticular and Haemopoetic System RVC Intergrated BVetMed Course, Royal Veterinary College
White, R. A. S, (2003), Tumours of the intestines, in BSAVA Manual of Canine and Feline Oncology, second edition, Eds Dobson J. M, Lascelles B. D. X, Gloucester, British Small Animal Veterinary Association, pp 229-233
| This article has been peer reviewed but is awaiting expert review. If you would like to help with this, please see more information about expert reviewing. |
Error in widget FBRecommend: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69c17db6917494_47123658 Error in widget google+: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69c17db697ca48_68341552 Error in widget TwitterTweet: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69c17db69efd86_66267598
|
| WikiVet® Introduction - Help WikiVet - Report a Problem |
- OpenPages
- Pages with broken file links
- Stomach and Abomasum - Proliferative Pathology
- Lymphoreticular and Haemopoietic Diseases
- Neoplasia
- Intestines - Proliferative Pathology
- Tongue - Pathology
- Intestinal Diseases - Dog
- Gastric Diseases - Dog
- Lymphoreticular and Haematopoietic Diseases - Dog
- Intestinal Diseases - Cat
- Gastric Diseases - Cat
- Lymphoreticular and Haematopoietic Diseases - Cat
- Alimentary Diseases - Horse
- Nasal Cavity - Hyperplastic/Neoplastic Pathology
- Respiratory System - Hyperplastic/Neoplastic Pathology
- Liver, Secondary Tumours
- Splenic Neoplasia
- Expert Review