Difference between revisions of "Gastric Ulceration - Dog"
TestStudent (talk | contribs) |
|||
| (35 intermediate revisions by 4 users not shown) | |||
| Line 1: | Line 1: | ||
| − | {{ | + | {{OpenPagesTop}} |
| − | + | Also known as: '''''Gastrointestinal ulceration | |
| − | + | ||
| − | + | ==Introduction== | |
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | + | See also:'''[[Gastric Ulceration - all species]]''' | |
| − | [[ | ||
| − | + | Gastric ulcer is a round or oval punched out lesion of the gastric mucosa ranging from 1-4 cm in diameter. | |
| − | |||
There are many disease associations including: | There are many disease associations including: | ||
| Line 26: | Line 17: | ||
|- | |- | ||
|'''Hypotension''' | |'''Hypotension''' | ||
| − | |[[Shock | + | |[[Shock|Shock]], Sepsis |
|- | |- | ||
|'''Drug - induced''' | |'''Drug - induced''' | ||
| Line 35: | Line 26: | ||
|- | |- | ||
|'''Inflammatory''' | |'''Inflammatory''' | ||
| − | |[[Gastritis, Acute|Gastritis]], [[Pancreatitis - Dog | + | |[[Gastritis, Acute|Gastritis]], [[Pancreatitis - Dog|Pancreatitis]] |
|- | |- | ||
|'''Neoplastic''' | |'''Neoplastic''' | ||
| − | |Adenocarcinoma, lymphosarcoma, leiomyoma, [[Gastrinoma|gastrinoma]] (Zollinger-Ellison syndrome), | + | |Adenocarcinoma, lymphosarcoma, leiomyoma, [[Gastrinoma|gastrinoma]], (Zollinger-Ellison syndrome), Mast cell Tumours. |
|- | |- | ||
|'''Metabolic/endocrine''' | |'''Metabolic/endocrine''' | ||
| Line 44: | Line 35: | ||
|} | |} | ||
| − | Gastric ulceration is caused by damage to the gastric mucosa through the above mechanisms. [[NSAIDs|NSAIDs]] directly damage the mucosa and interfere with | + | Gastric ulceration is caused by damage to the gastric mucosa through the above mechanisms. [[NSAIDs|NSAIDs]] directly damage the mucosa and interfere with prostaglandin synthesis. Gastric ulceration is worsened by the use of NSAIDs in combination with [[Steroids|corticosteroids]]. This risk can be minimised by using cyclooxygenase-1 (COX-1) sparing NSAIDs. |
| − | Gastric acid hypersecretion following mast cell degranulation of histamine and gastrin secretion from gastrinomas is a major cause of gastric ulceration. | + | Gastric acid hypersecretion following mast cell degranulation of histamine and gastrin secretion from [[Gastrinoma|gastrinomas]] is a major cause of gastric ulceration. |
==Signalment== | ==Signalment== | ||
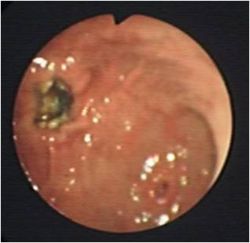
| + | [[Image:Gastric ulceration.jpg|thumb|right|250px|Gastric Ulceration - by David Walker RVC]] | ||
Sled dogs are prone to gastric ulceration. | Sled dogs are prone to gastric ulceration. | ||
| − | |||
==Clinical Signs== | ==Clinical Signs== | ||
History may involve access to toxins and drugs such as [[NSAIDs|NSAIDs]]. | History may involve access to toxins and drugs such as [[NSAIDs|NSAIDs]]. | ||
Clinical Signs can include vomiting, haematemesis, malaena, pale mucous membranes, abdominal pain, weakness, inappetance and hypersalivation which can progress to circulatory compromise. | Clinical Signs can include vomiting, haematemesis, malaena, pale mucous membranes, abdominal pain, weakness, inappetance and hypersalivation which can progress to circulatory compromise. | ||
| − | |||
==Laboratory Tests== | ==Laboratory Tests== | ||
===Haematology=== | ===Haematology=== | ||
| − | [[ | + | [[Regenerative and Non-Regenerative Anaemias|Anaemia]] which may be regenerative initially, and can progress to microcytic, hypochromic and minutely regenerative anaemia. |
| − | A thrombocytosis may also be present. If a stress leucogram (lymphopenia and neutrophilia) is not present this is supportive of | + | A thrombocytosis may also be present. If a [[Stress Leucogram|stress leucogram]] (lymphopenia and neutrophilia) is not present this is supportive of hypoadrenocorticism. |
Examination of the buffy coat may detect mastocytosis. | Examination of the buffy coat may detect mastocytosis. | ||
| − | A [[ | + | A [[Neutrophilia|Neutrophilia]] and a left shift are indicative of inflammation or gastric perforation. |
| − | There may also be abnormalities in [[Haemostasis | + | There may also be abnormalities in [[:Category:Haemostasis and Bleeding Disorders|haemostasis]]. |
===Biochemistry=== | ===Biochemistry=== | ||
Increased liver enzymes and bilirubin, decreased urea, albumin and cholesterol will indicate hepatic disease as an underlying problem. | Increased liver enzymes and bilirubin, decreased urea, albumin and cholesterol will indicate hepatic disease as an underlying problem. | ||
If renal disease is present, an azotaemia will be present on biochemistry. | If renal disease is present, an azotaemia will be present on biochemistry. | ||
| − | If | + | If Hypoadrenocorticism is the cause of the ulceration, it is likely biochemistry will show a Sodium:Potassium ratio of less than 27:1. |
If the animal is vomiting this will lead to electrolyte and acid-base abnormalities, a metabolic alkalosis, hypokalaemia and hypochloraemia. | If the animal is vomiting this will lead to electrolyte and acid-base abnormalities, a metabolic alkalosis, hypokalaemia and hypochloraemia. | ||
===Urinalysis=== | ===Urinalysis=== | ||
| − | Animals will be dehydrated resulting in | + | Animals will be dehydrated resulting in hypersthenuria. If renal disease is the underlying cause, urine may be isosthenuric. |
===Plain radiography=== | ===Plain radiography=== | ||
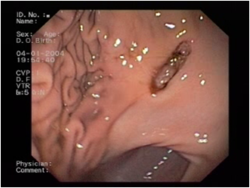
| − | [[Image:Gastric ulceration.png|thumb|right|250px|Gastric Ulceration - | + | [[Image:Gastric ulceration.png|thumb|right|250px|Gastric Ulceration - by David Walker RVC]] |
| − | Not usually diagnostic but can rule out differentials such as foreign bodies and [[Peritonitis|peritonitis]]. | + | Not usually diagnostic but can rule out differentials such as [[Gastric Foreign Objects|foreign bodies]] and [[Peritonitis|peritonitis]]. |
===Positive contrast radiography=== | ===Positive contrast radiography=== | ||
| Line 85: | Line 75: | ||
===Endoscopy and Biopsy=== | ===Endoscopy and Biopsy=== | ||
| − | Diagnostic test of choice and allows biopsies to be taken. | + | Diagnostic test of choice and allows biopsies to be taken. NSAID related ulcers are regularly located in the antrum and there is limited mucosal thickening or irregularity whereas ulcerated [[Gastric Neoplasia - Dog and Cat|gastric tumours]] will have thickened mucosa and edges. Any biopsies should be taken at the edge of normal and diseased tissue to avoid further deepening or perforation. |
==Treatment== | ==Treatment== | ||
| − | The main aim is to treat any primary underlying cause whilst giving general support. This may be hydrating, restoring electrolytes and acid-base and also helping the gastric lining to recover. Anti-ulcerative therapy should be continued for up to 6-8 weeks. | + | The main aim is to treat any primary underlying cause whilst giving general support. This may be hydrating, restoring electrolytes and acid-base and also helping the gastric lining to recover. [[Gastroprotective Drugs|Anti-ulcerative]] therapy should be continued for up to 6-8 weeks. |
| + | |||
| + | ===[[Principles of Fluid Therapy|Fluid Therapy]]=== | ||
| + | Depends upon the degree of dehydration, presence of shock and any other diseases that are affected by volume. Prolonged vomiting or anorexia may lead to hypokalaemia so KCl may need adding to any fluids given. Normal rates for treatment of shock apply with dehydration being overcome by a fluid rate over 24 hours to replace the deficits along with a maintenance rate. | ||
| − | |||
| − | |||
| − | |||
===Reducing acid secretion=== | ===Reducing acid secretion=== | ||
[[Gastroprotective Drugs#Histamine (H2) Receptor Antagonists|Histamine receptor antagonists]] inhibit acid secretion and include cimetidine, ranitidine and famotidine. | [[Gastroprotective Drugs#Histamine (H2) Receptor Antagonists|Histamine receptor antagonists]] inhibit acid secretion and include cimetidine, ranitidine and famotidine. | ||
| − | Omeprazole is the drug of choice to treat ulceration associated with mass cell tumours and gastrinomas. It inhibits the hydrogen-potassium ATPase which prevents hydrogen ion | + | [[Gastroprotective Drugs#Proton Pump Inhibitors|Omeprazole]] is the drug of choice to treat ulceration associated with mass cell tumours and gastrinomas. It inhibits the hydrogen-potassium ATPase which prevents hydrogen ion production by the parietal cells. |
| − | |||
| − | |||
| − | |||
===Mucosal protectants=== | ===Mucosal protectants=== | ||
| − | Such as misoprostol can be given alongside NSAIDs to decrease the risk of ulceration. | + | Such as misoprostol can be given alongside NSAIDs to decrease the risk of ulceration. [[Gastroprotective Drugs#Binding Agents|Sucralfate]] which is polyaluminium sucrose sulphate, binds to damaged mucosa and assists in the treatment of gastric ulceration. It is best given 2 hours after acid inhibitors to prevent interference. |
===Prophylaxis=== | ===Prophylaxis=== | ||
| − | Prophylactic treatment has been shown not to prevent gastric ulceration. | + | Prophylactic treatment has been shown not to prevent gastric ulceration. Sucralfate is reported to be the best drug in patients receiving high doses of glucocorticoids. |
===Anti-emetics=== | ===Anti-emetics=== | ||
| Line 113: | Line 100: | ||
Is best provided by [[Opioids|opiods]] such as buprenorphine, pethidine and fentanyl. | Is best provided by [[Opioids|opiods]] such as buprenorphine, pethidine and fentanyl. | ||
| − | === | + | ===Antibiotics=== |
| − | Animals suffering from shock and gastric barrier dysfunction may require prophylactic antibiotic cover. First line drugs include [[Penicillins|ampicillin]] or a [[Cephalosporins|cephalosporin]] which are effective against Gram-positive, some Gram-negative and some anaerobic bacteria. These can be combined with an [[Aminoglycosides|aminoglycoside]] which are effective against Gram-negative aerobes if sepsis is present. [[Fluoroquinolones|Enrofloxacin]] can also be used instead of an | + | Animals suffering from shock and gastric barrier dysfunction may require prophylactic [[Antibiotics|antibiotic]] cover. First line drugs include [[Penicillins|ampicillin]] or a [[Cephalosporins|cephalosporin]] which are effective against Gram-positive, some Gram-negative and some anaerobic bacteria. These can be combined with an [[Aminoglycosides|aminoglycoside]] which are effective against Gram-negative aerobes if sepsis is present. [[Fluoroquinolones|Enrofloxacin]] can also be used instead of an aminoglycoside in skeletally mature animals. |
===Surgery=== | ===Surgery=== | ||
| − | May be required to investigate or to resect | + | May be required to investigate or to resect perforating ulcers which may lead to [[Peritonitis - Cats and Dogs|peritonitis]]. |
==Prognosis== | ==Prognosis== | ||
For animals with peptic ulcers is good. Prognosis is poorer for patients with renal or hepatic failure related ulcers. It is also poor for animals with gastric carcinoma and gastrinoma. | For animals with peptic ulcers is good. Prognosis is poorer for patients with renal or hepatic failure related ulcers. It is also poor for animals with gastric carcinoma and gastrinoma. | ||
| + | |||
| + | {{Learning | ||
| + | |Vetstream = [https://www.vetstream.com/canis/Content/Disease/dis01152.asp, Gastric ulceration] | ||
| + | |literatures search = [http://www.cabdirect.org/search.html?q=%28title%3A%28gastr*%29+OR+title%3A%28stomach%29%29+AND+title%3A%28ulcer*%29+AND+od%3A%28dogs%29 Gastric Ulceration in Dogs publications] | ||
| + | }} | ||
==References== | ==References== | ||
| Line 126: | Line 118: | ||
Hall, J.E., Simpson, J.W. and Williams, D.A., (2005) '''BSAVA Manual of Canine and Feline Gastroenterology (2nd Edition)''' ''BSAVA'' | Hall, J.E., Simpson, J.W. and Williams, D.A., (2005) '''BSAVA Manual of Canine and Feline Gastroenterology (2nd Edition)''' ''BSAVA'' | ||
| − | + | Ettinger, S.J, Feldman, E.C. (2005) '''Textbook of Veterinary Internal Medicine''' (6th edition, volume 2) ''W.B. Saunders Company'' | |
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | + | {{review}} | |
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| + | {{OpenPages}} | ||
| − | + | [[Category:Gastric_Ulceration]][[Category:Gastric Diseases - Dog]] | |
| − | [[Category:Gastric_Ulceration]][[Category:Dog]] | + | [[Category:Expert_Review - Small Animal]] |
| − | [[Category: | ||
Latest revision as of 13:21, 6 September 2015
Also known as: Gastrointestinal ulceration
Introduction
See also:Gastric Ulceration - all species
Gastric ulcer is a round or oval punched out lesion of the gastric mucosa ranging from 1-4 cm in diameter.
There are many disease associations including:
| Disease type | E.g. |
|---|---|
| Hypotension | Shock, Sepsis |
| Drug - induced | Non-steroidal anti-inflammatory drugs (NSAIDs) |
| Idiopathic | Stress, exercise induced |
| Inflammatory | Gastritis, Pancreatitis |
| Neoplastic | Adenocarcinoma, lymphosarcoma, leiomyoma, gastrinoma, (Zollinger-Ellison syndrome), Mast cell Tumours. |
| Metabolic/endocrine | Hypoadrenocorticism, liver disease, uraemia, Disseminated Intravascular Coagulation (DIC), mastocytosis and hypergastrinaemia |
Gastric ulceration is caused by damage to the gastric mucosa through the above mechanisms. NSAIDs directly damage the mucosa and interfere with prostaglandin synthesis. Gastric ulceration is worsened by the use of NSAIDs in combination with corticosteroids. This risk can be minimised by using cyclooxygenase-1 (COX-1) sparing NSAIDs.
Gastric acid hypersecretion following mast cell degranulation of histamine and gastrin secretion from gastrinomas is a major cause of gastric ulceration.
Signalment
Sled dogs are prone to gastric ulceration.
Clinical Signs
History may involve access to toxins and drugs such as NSAIDs. Clinical Signs can include vomiting, haematemesis, malaena, pale mucous membranes, abdominal pain, weakness, inappetance and hypersalivation which can progress to circulatory compromise.
Laboratory Tests
Haematology
Anaemia which may be regenerative initially, and can progress to microcytic, hypochromic and minutely regenerative anaemia. A thrombocytosis may also be present. If a stress leucogram (lymphopenia and neutrophilia) is not present this is supportive of hypoadrenocorticism. Examination of the buffy coat may detect mastocytosis. A Neutrophilia and a left shift are indicative of inflammation or gastric perforation. There may also be abnormalities in haemostasis.
Biochemistry
Increased liver enzymes and bilirubin, decreased urea, albumin and cholesterol will indicate hepatic disease as an underlying problem. If renal disease is present, an azotaemia will be present on biochemistry. If Hypoadrenocorticism is the cause of the ulceration, it is likely biochemistry will show a Sodium:Potassium ratio of less than 27:1. If the animal is vomiting this will lead to electrolyte and acid-base abnormalities, a metabolic alkalosis, hypokalaemia and hypochloraemia.
Urinalysis
Animals will be dehydrated resulting in hypersthenuria. If renal disease is the underlying cause, urine may be isosthenuric.
Plain radiography
Not usually diagnostic but can rule out differentials such as foreign bodies and peritonitis.
Positive contrast radiography
May show filling defects.
Ultrasonography
Shows gastric thickening and rules out other differential diagnoses.
Endoscopy and Biopsy
Diagnostic test of choice and allows biopsies to be taken. NSAID related ulcers are regularly located in the antrum and there is limited mucosal thickening or irregularity whereas ulcerated gastric tumours will have thickened mucosa and edges. Any biopsies should be taken at the edge of normal and diseased tissue to avoid further deepening or perforation.
Treatment
The main aim is to treat any primary underlying cause whilst giving general support. This may be hydrating, restoring electrolytes and acid-base and also helping the gastric lining to recover. Anti-ulcerative therapy should be continued for up to 6-8 weeks.
Fluid Therapy
Depends upon the degree of dehydration, presence of shock and any other diseases that are affected by volume. Prolonged vomiting or anorexia may lead to hypokalaemia so KCl may need adding to any fluids given. Normal rates for treatment of shock apply with dehydration being overcome by a fluid rate over 24 hours to replace the deficits along with a maintenance rate.
Reducing acid secretion
Histamine receptor antagonists inhibit acid secretion and include cimetidine, ranitidine and famotidine.
Omeprazole is the drug of choice to treat ulceration associated with mass cell tumours and gastrinomas. It inhibits the hydrogen-potassium ATPase which prevents hydrogen ion production by the parietal cells.
Mucosal protectants
Such as misoprostol can be given alongside NSAIDs to decrease the risk of ulceration. Sucralfate which is polyaluminium sucrose sulphate, binds to damaged mucosa and assists in the treatment of gastric ulceration. It is best given 2 hours after acid inhibitors to prevent interference.
Prophylaxis
Prophylactic treatment has been shown not to prevent gastric ulceration. Sucralfate is reported to be the best drug in patients receiving high doses of glucocorticoids.
Anti-emetics
Anti-emetics are indicated if vomiting is severe causing fluid and electrolyte imbalances and discomfort.
Analgesia
Is best provided by opiods such as buprenorphine, pethidine and fentanyl.
Antibiotics
Animals suffering from shock and gastric barrier dysfunction may require prophylactic antibiotic cover. First line drugs include ampicillin or a cephalosporin which are effective against Gram-positive, some Gram-negative and some anaerobic bacteria. These can be combined with an aminoglycoside which are effective against Gram-negative aerobes if sepsis is present. Enrofloxacin can also be used instead of an aminoglycoside in skeletally mature animals.
Surgery
May be required to investigate or to resect perforating ulcers which may lead to peritonitis.
Prognosis
For animals with peptic ulcers is good. Prognosis is poorer for patients with renal or hepatic failure related ulcers. It is also poor for animals with gastric carcinoma and gastrinoma.
| Gastric Ulceration - Dog Learning Resources | |
|---|---|
To reach the Vetstream content, please select |
Canis, Felis, Lapis or Equis |
References
Hall, J.E., Simpson, J.W. and Williams, D.A., (2005) BSAVA Manual of Canine and Feline Gastroenterology (2nd Edition) BSAVA
Ettinger, S.J, Feldman, E.C. (2005) Textbook of Veterinary Internal Medicine (6th edition, volume 2) W.B. Saunders Company
| This article has been peer reviewed but is awaiting expert review. If you would like to help with this, please see more information about expert reviewing. |
Error in widget FBRecommend: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69a204f26ce4a2_63574435 Error in widget google+: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69a204f27740b1_66949109 Error in widget TwitterTweet: unable to write file /var/www/wikivet.net/extensions/Widgets/compiled_templates/wrt69a204f2850ef7_88447553
|
| WikiVet® Introduction - Help WikiVet - Report a Problem |