Difference between revisions of "Lungs Inflammatory - Pathology"
Jump to navigation
Jump to search
| Line 227: | Line 227: | ||
=='''Other forms of pneumonia'''== | =='''Other forms of pneumonia'''== | ||
| − | |||
| − | |||
| − | |||
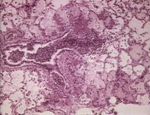
[[Image:Acute necrotising pneumonia.jpg|right|thumb|150px|<small><center>Acute necrotising pneumonia (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | [[Image:Acute necrotising pneumonia.jpg|right|thumb|150px|<small><center>Acute necrotising pneumonia (Image sourced from Bristol Biomed Image Archive with permission)</center></small>]] | ||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | [[ | + | ===[[Aspiration Pneumonia]]=== |
| Line 306: | Line 282: | ||
[[Category:Pneumonia]] | [[Category:Pneumonia]] | ||
| − | |||
| − | |||
=Test yourself with the Lungs Pathology Flashcards= | =Test yourself with the Lungs Pathology Flashcards= | ||
[[Lungs_Flashcards_-_Pathology|Lungs Pathology Flashcards]] | [[Lungs_Flashcards_-_Pathology|Lungs Pathology Flashcards]] | ||
Revision as of 18:19, 19 February 2011
Pneumonia - Introduction and Classification
- Pneumonia
- Inflammation that takes place in the alveoli and their walls
- Can be grouped either according to
- Nature of the inflammatory process
- Aetiological agent
- Pattern of the lesion
- Patterns of lung inflammation vary depending on the aetiology, route and method of exposure and multiple host factors including age, general health, and immune status
- There are five general patterns of pneumonia:
Bronchopneumonia
Bronchointerstitial Pneumonia
Lobar Pneumonia
Interstitial Pneumonia
Embolic Pneumonia
Granulomatous Pneumonia
Verminous Pneumonia
Stages of pneumonia
- Regardless of the pattern, all pneumonias pass through three stages:
- Exudative phase
- In this initial stage inflammatory exudate pours into alveolar spaces and alveolar capillaries are congested
- Type I alveolar epithelial cells are highly sensitive to injury and cannot proliferate in response to injury
- Necrosis and sloughing of injured type I cells, denuding alveolar spaces of lining epithelium
- Neutrophils begin to enter alveolar spaces distended with inflammatory oedema
- Proliferative phase
- Type II alveolar cells (less sensitive to and can proliferate in response to injury) begin to proliferate within 24 hours and eventually line the alveolar walls denuded of type I cells ***By 6 days cuboidal type II cells can completely line the alveoli
- Proliferation of type II cells marks the shift from the exudative to the proliferative stage of pneumonia, also heralded by decreased blood flow in alveolar capillaries
- Because the original squamous type I cells have been replaced by cuboidal type II cells, the microscopic appearance of pneumonic lungs at about 1 week has been described as “alveolar epithelialization”, “alveolar adenomatosis”, or “bronchiolisation of alveoli”
- Repair phase
- Resolution of pneumonia is accomplished by transformation of type II cells to type I cells
- Exudative phase
Pulmonary abscesses
Infectious causes of pneumonia
Other forms of pneumonia
Aspiration Pneumonia
Gangrenous pneumonia
- Can occur following severe infections in which tissue becomes necrotic and is then invaded by putrefactive saprophytes, however this is rare.
- The usual cause is administration of medicines (intended for the oesophagus!) or as a sequel to aspiration pneumonia
- The dead tissue undergoes liquefactive necrosis forming a cavity which is surrounded by intense hyperaemia and inflammation
Lipid pneumonia
- Associated with inhalation of oil, paraffin, etc.
- Reaction dominated by macrophages which fill the alveoli and interstitial thickening (mononuclear cells and fibrosis)
- Tends to acumulate in ventral regions bilterally
- Occurs subclinically in cats, sometimes dogs, unrelated to aspiration
- Gross lesion:
- Multifocal, firm, white nodules
- Microscopic lesions:
- Macrophages full of lipid forming foam within alveoli
- Interstitial lymphocyte and plasma cell infiltration, fibrosis
Uraemic pneumonia
- Severe uraemia causes increased permeability of the blood-air barrier and therefore can cause pulmonary oedema
- In addition to the oedema, there may also be degeneration and calcification of smooth muscle and connective tissue fibres
- Lungs do not collapse on opening the thorax in severe cases
Foetal pneumonia
- Especially foals and farm species
- Due to aspiration of amniotic fluid contaminated with meconium and bacteria
- Secondary to fetal distress
- Microscopic lesions of bronchopneumonia
- Involves all lobes (versus postnatal bronchopneumonia)
- Haematogenous spread
- Causes interstitial pneumonia
- Often caused by Listeria monocytogenes, Salmonella spp. or Chlamydia psittaci
- In viral abortions
- Cause bronchointerstitial pneumonia
- E.g.: IBR, PI-3 and equine viral rhinopneumonitis